|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-II) |
Number 3 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-II) |
Number 3 |
||
|
|
||||
|
|
||||
Comparison of Effectiveness of Two Different
Premarin Dose in Hot Flash Treatment
Mojgan Barati1, Farideh Moramezi2, Sara Masihi3, Seiedeh Naiereh Moghadam4
ABSTRACT
Objective: Hot flush is the most common and severe problem of menopausal period. Estrogen is used for elimination of hot flush as an original and selective medicine. The objective was to determine the lowest useful dose because of estrogen’s side effects.
Methodology: This clinical trial was done on 180 menopausal women who were complaining of hot flush. They were randomly divided in three groups. Group one took 0.3mg conjugated estrogen plus 1.25mg medroxyprogestronacetate, group two took 0.15mg conjugated estrogen plus 1.25mg medroxyprogestronacetate and group three took placebo for one month. Hot flush improvements in these three groups were defined.
Results: The average improvement was 78.5% with median 80 and mode 80 in group one (0.3 mg). The average improvement was 63.3 percent with median 60 and mode 60 in group two (0.15mg). The average improvement was 13.8% with median one and mode one in group three (placebo).
Conclusion: Due to average improvement of 63.3% in 0.15mg conjugated esrogen user group it is logical to begin hot flush treatment with this 0.15mg conjugated estrogen dose.
KEY WORDS: Hot flush, Estrogen, Dose.
Pak J Med Sci April - June 2008 (Part-II) Vol. 24 No. 3 406-409
How to cite this article:
Barati M, Moramezi F, Masihi S, Moghadam SN. Comparison of effectiveness of two different Premarin dose, in hot flash treatment. Pak J Med Sci 2008;24(3):406-9.
1. Mojgan Barati MD,
Assistant Professor,
2. Farideh Moramezi MD,
Assistant Professor,
3. Sara Masihi,
Assistant Professor,
4. Seiedeh Naiereh Moghadam,
Gynecologist
1-4: Ahwaz Jondishapour University of Medical Science
Ahwaz – Iran.
Correspondence
Mojgan Barati
Obs and Gynae Ward,
Emam Khomaini Hospital,
24 Metry Street, Ahwaz – Iran.
E-mail: brati_m@yahoo.com
farideh330@yahoo.com
sara_hasan2002@yahoo.com
* Received for Publication: January 24, 2008
* Accepted: March 18, 2008
INTRODUCTION
The vasomotor flush is viewed as the hallmark of the female climacteric, experienced to some degree by most postmenopausal women.
1 The term hot flush is descriptive of a sudden onset of reddening of the skin over the head, neck, and chest, accompanied by a feeling of intense body heat and concluded by sometimes profuse perspiration. The duration varies from a few seconds to several minutes and, rarely, more. The frequency may be rare to recurrent every few minutes. Flushes are more frequent and severe at night or during the time of stress.1 In a cool environment, hot flushes are fewer, less intense, and in shorter duration compared with a warm environment.2Vasomotor symptoms affect up to 75% of perimenopausal women. Symptoms last for one to two years after menopause in most women, but may continue for longer in others.
3Hot flashes not only disturb women at work and interrupt daily activities but also disrupt sleep.
4 Systemic estrogen therapy is the most effective treatment available for vasomotor symptoms and associated sleep disturbance.3 The estrogen dose required to control hot flash may vary from person to person.Very-low-dose estrogen therapy also effectively treats hot flashes in the large number of women. Low-dose oral esterified and conjugated estrogens (0.3mg daily) or transdermal estradiol (0.025mg weekly) often is effective and is associated with minimal side effects and endometrial stimulation.
5-7 Given the known risks, HT should be used at the lowest effective dose for the shortest amount of time that meets treatment goals.3 Long-term use of HT is associated with an increased risk of breast cancer.8 Results from multiple studies indicate that postmenopausal hormone therapy increased the risk of venous thromboembolism about two fold, mostly in the first year or two of treatment. A conclusion supported by the reported results from the canceled estrogen-progestin arm of the WHI.9 Pancreatitis and severe hypertriglyceridemia can be precipitated by the administration of oral estrogen to women with elevated triglyceride levels.10,11The Nurses’ Health study indicated that oral estrogen therapy may carry a 1.5-2.0 fold increased risk of gallbladder disease.
12 In the Nurses’ Health Study, newly diagnosed asthma was increased about 2-fold by hormone therapy.13METHODOLOGY
In this study 180 menopausal women who were complaining of hot fluh were selected and randomly divided in to three 60 persons groups and every other one is given different prescriptions for one month. The first and second groups were given different estrogen dose and third group selected as a control. The first group No.1 was given 0.3mg conjugated estrogen plus 1.25mg of medroxyprogesterone acetate daily for one month. The second group No.2 was given 0.15 conjugated estrogen plus 1.25 medroxyprogesterone acetate daily for one month. The control group No.3 was given one tablet of placebo daily for one month. After one month, the tested groups were asked about hot flush condition. Data were gathered through questionnaires and analyzed. The efficacy of the three remedies were studied and compared. The way of determination of hot flush intensity in patients was that, they were asked to give a score from 1 to 10 for their hot flush one was the least intensity of hot flush and 10 was the highest. Meanwhile they were asked for the number of hot flushes per day. Then, according to the formula the number of hot flushes was multiplied by intensity of hot flushes. The study was clinical trial and the method of calculation was as per the formula given below:
(Z1- /2+Z1-ß)˛ (p(1-p)×2)
n= ———————————— =0.005
(p-pą) Z1- /2=1.95
For 10% power Z(1-ß =0.84)
N= 60 P=0.8
P1-P2= 0.2
Methods of statistical analysis: For comparison of relations, Qi square test was utilized for quantitative data.
RESULTS
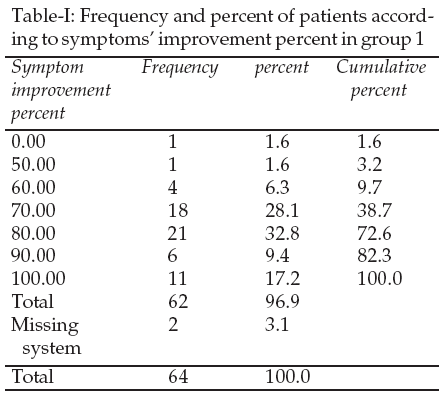
In the group one with 0.3mg estrogen conjugate, the average improvement was 78.5% with median 80 and mode 80. The response between 70 to 90 percent was seen among 70% of women. Seventy percent improvement was seen in 28 percent of women, 80 percent improvement was seen in 32 percent of women and 90 percent improvement was seen in 9 percent of women. The interesting point was 100% improvement in 17% of women. The least improvement was seen in 1.5% of women that have 50 percent improvement (Table-I).
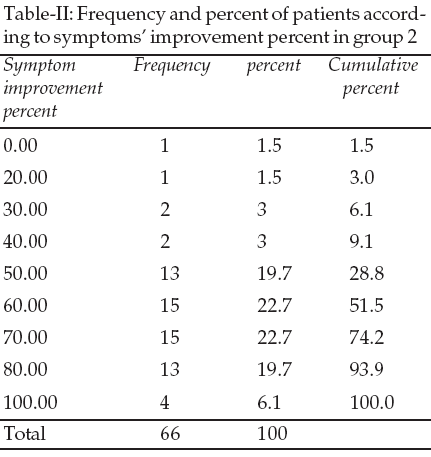
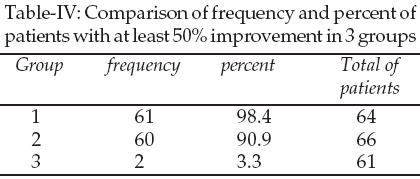
In the group two with 0.15mg estrogen conjugate, the average improvement was 63.3 percent with median 60 and mode 60. The response between 50 to 70 percent to remedy was seen in 63 percent in this group. 100% improvement was seen in 6% in this group. The least improvement was in 1.5% that showed 20% improvement (Table-II). Among 90 percent of women in group two, at least a decrease of 50 percent hot flush was seen (Table-III).
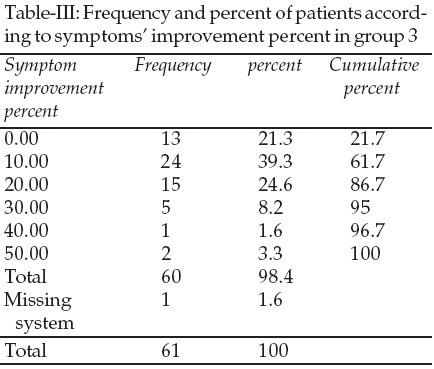
In the group three that was treated with placebo the average improvement was 13.8% with median one and mode one. No response was seen in 21 percent of this group. In 85% of this group the improvement rate was between 0 to 20 percent (Table-IV).
Meanwhile it was seen that hot flush frequency was in contrast with maternity number and women’s age. When the number of maternities is higher, the hot flush frequency is lower and when the women’s age is higher at the time of menopause, the milder hot flush could be seen. How flushes occur due to vasomotor instability caused by seduced circulating levels as the ovarian function of estrogen production declines due to ovarian failure.
DISCUSSION
Among existing problems in menopause, hot flushes are most common problem that exists in almost 80 percent of women in the first years of menopause. Sometimes hot flush is very severe and frequent causing fatigue and sleep disturbance. Many attempts have been made to cure menopausal symptoms. The selective method to cure hot flush is estrogen replacement. This method has the efficiency of 95% and is a remedy accepted by FDA. Estrogen especially in the case that frequent and overnight hot flushes disturb women’s life is really efficient in improvement of quality of life.
It is said that may be in the case of mild hot flush one can utilize remedies such as change of life style or consumption of vitamins and substances such as bean and clover but in the case of moderate and sever hot flushes, one should use estrogenic therapy. Estrogen therapy in adequate doses shows an early clinical response and must be continued for a reasonable period of a few months and then tappered off. In some cases it may be contin ued for months or few years depending on the need. It is said that with daily consumption of 0.25mg estradiol for three weeks, one can have 91 percent improvement.
Nowadays according to different studies 0.3mg estrogen conjugate along with progesterone is used daily. However there are different regimens of hormone replacement therapy for post menopausal symptoms.
Because of possibility of estrogen side effects, we used the lower dose of estrogen and compared these results with the common remedy in this study. In the group wherein usual consumption of 0.3mg estrogen was used, the response of 70 to 90 percent was seen in 70 percent of women and almost 17 percent of women felt complete recovery. The least improvement was 50 percent that was seen in 1.5 percent. In the group that was treated with 0.15mg estrogen, the response of 50 to 70 percent was seen in 63 percent of women.
The least improvement was 20 percent that was seen in 1.5 percent of women and 6% felt complete recovery. Due to average improvement of 63.3% and at least 50% improvement in 90% of patients in 0.15mg conjugated esrogen user group it is logical to begin the treatment with of 0.15mg estrogen conjugate consumption in women who don’t have an intense hot flush or estrogen consumption is dangerous for them. After at least one month, the response to therapy could be evaluated and in the case of improvement or satisfactory feelings it can be continued. If no or unsatisfactory response to remedy was seen, the drug dose should be increased until the symptoms of improvement are visible. In this way, in addition to elimination of menopausal symptoms, the high consumption of estrogen and its related dangers could be prevented. It is recommended that change of life style, living in cold places and exercise, deep breath, consumption of bean and clover are helpful. However, most of the later is a placebo effect.
REFERENCES
1. Sproff L. Clinical Gynecologic Endocrinology and infertility, sixth edition, Lippincott Williams and Wilkins. Philadelphia 2001;1000,640.
2. Kronnenberg F, Barnard RM. Modulation of Menopausal Hot Flashes by Ambient Temprature, J Them Biol 1992;17:43.
3. Berek JS. Berek, Novak’s Gynecology. 14th ed. Philadelphia: Lippincott Williams & Wilkins. 2007;1325-7.
4. SchilT I, Restein Q, Tulchinsky D. Effects of estrogens on sleep and psychological state of the hypogonadal woman. JAMA 1979;242:2405-7.
5. Utian W, Shoupe D, Bachmann G. Relief of vasomotor symptoms and vaginal atrophy with lower doses of conjugated equine estrogen and medroxypro-gesterone acetate. Fertil Streril 2001;6:1065.
6. Genant H, Lucas I, Weiss S. Low-dose esterified estrogen therapy. Arch Litem Med 1997;157:2609-15.
7. Weiss SR. Ellman H, Dolker I. A randomized controlled trial of four doses of transdermal estradiol for preventing postmenopausal bone loss. Obsrer Gye 1999;94:330-6.
8. Collaboration Group on Hormonal Factors in Breast Cancer. Breast cancer and hormone replacement therapy. Lancet 1997;350:1047-59.
9. Writssing Group for the Women’s Health Initiative Investigators, Risks and benefits of estrogen plus progestin in healthy postmenopausal women .Principal results from the Women’s Health Initiative randomized controlled trial. JAMA 2002;288:321.
10. Glueck CJ, Lang J, Hamer T, Tracy T, Severe hypertriglyceridemia and pancreatitis when estrogen replacement therapy is given to hypertriglyceridemic women. Int J Lab Clin Med 1994;123:59.
11. Goldenberg NM, Wang P, Glueck CJ. An observational study of severe hypertriglyceridemia, hypertriglyceridemic acute pancreatits and failure of triglyceride-lowering therapy when estrogens are given to women with and without familial hypertriglyceridemia. Clin Chim Acta 2003;332:11.
12. Grodstein F, Coldiz GA, Stampfer MJ. Postmenopausal hormone use and cholecystectomy in a large prospective study. Obstet Gynecol 1994;83:5.
13. Barr RG, Wentowdki CC, Grodstein F, Somers SC, Stampfer MJ, Schwartz J, et al. Prospective study of postmenopausal hormone use and newly diagnosed asthma and chronic obstructive pulmonary disease. Arch Intern Med 2004;164:379.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk