|
 |
|
Published
by : PROFESSIONAL MEDICAL PUBLICATIONS |
|
ISSN 1681-715X |
|
|
|
|
|
- |
|
ORIGINAL
ARTICLE |
|
- |
|
Volume 25 |
April
- June 2009 (Part-II) |
Number 3 |
|
|
|
Appendicitis in children: An increasing
health scourge in a developing country
Osarumwense David Osifo1, Scott. O. Ogiemwonyi2
ABSTRACT
Objectives: The incidence of appendicitis is rising
in developing countries. We aimed to determine the effects of late referrals
and wrong treatment on the outcome of appendicitis in Benin City, Nigerian.
Methodology: A retrospective analysis of all
children treated for appendicitis at the University of Benin Teaching
Hospital, between January 1998 and December 2007. Pre/post operative
morbidities, length of hospitalization, cost of treatment and mortality were
compared between children who presented early, within 24 hours of first
episode of symptoms, and those who presented later.
Results: A total of 481 children aged between 2 and
16 (mean 9.7 � 2.8) years, comprising 265 males and 216 females with
male/female ratio1.2:1 had appendicectomy which accounted for 5.7% of total
pediatric operations and 47.5% of pediatric abdominal operations. Only 206
(42.8%) children presented during the first episode of symptoms and in
clinically stable state while 275 (57.2%) were referred after wrong diagnosis
and treatment by general practitioners which resulted in different
complications ranging from appendix abscess 60 (12.5%), appendix mass 54
(11.2%), perforated appendix 47 (9.8%), gangrenous appendix 41 (8.5%) and
peritonitis 34 (7.0%). These influenced post operative outcome with wound
infection recorded in 91 (18.9%), wound break down 35 (7.3%), septicemia 31
(6.4%), pelvic abscess 13 (2.7%) and death 1 (0.2%). These were not recorded
among those who presented early who also had significantly lower duration of
hospitalization and cost of treatment (P<0.0001).
Conclusion: Late referral due to low index of
suspicion was rampant which significantly increased associated morbidities and
mortality among children managed with appendicitis.
KEYWORDS:
Appendicitis, Children, Incidence, Outcome, Developing country.
Pak J Med Sci April - June 2009 (Part-II)
Vol. 25 No. 3 490-495
How to cite this article:
Osifo OD, Ogiemwonyi SO. Appendicitis in children: An increasing health
scourge in a developing country. Pak J Med Sci 2009;25(3): 490-495.
1. Osarumwense David Osifo, MBBS, FWACS
2. Scott. O. Ogiemwonyi, WASC, MBBS
1,2: Paediatric Surgery Unit,
Dept. of Surgery,
University of Benin Teaching Hospital,
Benin City, Nigeria.
Correspondence
Osifo O.D,
E-mail: Leadekso@yahoo.com
* Received for Publication: Oct. 22, 2008
* Revision Received: May 13, 2009
* Revision Accepted: May 15, 2009
INTRODUCTION
Appendicitis, the inflammation of vermiform appendix which
can be acute, sub-acute or recurrent, is associated with high morbidity which
can be prevented by timed appendicectomy.
1,2
The incidence has been reported to be high in developed cities where diet is
rich in fat and low in roughages. Although the exact incidence in sub-Saharan
Africa is not known due to poor data base, it has been reported to be lower
than in developed countries. This lower incidence in sub-Saharan Africa has
been attributed to diet high in roughages which are said to be protective
against inflammatory bowel lesions.3,4
There is endemicity of enteric infectious diseases such as typhoid fever,
amoebic dysentery, gastroenteritis and helminthes infestation in this
subregion which present as abdominal pain mimicking appendicitis.
Consequently, many clinicians place appendicitis at a lower position in the
list of differential diagnoses of abdominal pain in Nigerian children.5-8
Also, ignorance and poverty lead to delayed presentation of children with
appendicitis which allow complications to occur, compounding the diagnostic
difficulty.
Whereas appendicectomy done on clinically stable children
with mildly inflamed appendix have favourable outcome, the reverse is the case
in perforated or gangrenous appendix in clinically compromised children who
may develop life threatening complications after surgery.
1,2,9-11
Literatures3,4,12-15
searched on pediatric appendicitis in this subregion showed a progressive
increase in incidence from early 1960, but these have had minimal effect on
increasing awareness. As a result, severe morbidity resulting from delayed or
wrongly managed cases suspected to be due to other causes of abdominal pain
are increasing and have become worrisome. Moreover, African diets have been
westernized and enteric infections/infestation has been on the decline due to
improved standard of living. The need to reappraise the differential diagnosis
of abdominal pain in children in this subregion cannot be overemphasized.
The aim of this ten-year retrospective study was to review
cases of children treated for appendicitis with a view to determine the
incidence and compare the pre/post operative morbidities, length of
hospitalizations, cost of treatment and mortality between those who presented
early, within 24 hours of first episode of symptoms, and those who presented
later. This is to determine the effect of late referral on the outcome of
appendicitis so as to reduce avoidable morbidity and mortality in developing
countries.
METHODOLOGY
University of Benin Teaching Hospital is a tertiary
hospital located in Benin City, Edo State, in the South-South Geopolitical
Zone of Nigeria. It is a referral pediatric surgical center to which children
are referred from primary and secondary health institutions in the state.
Analysis of cases of children managed with appendicitis at the center between
January 1998 and December 2007 was done on retrieving their case files from
medical records department. Data collated were age, sex, pattern of
presentation, clinical state on arrival, diagnosis, preoperative morbidity,
operation, intraoperative findings, post operative morbidity, the treatment/
length of hospitalization and outcome. Also, the socioeconomic status of
parents, their level of education, place of residence and stable diets were
noted. Two children on whom sufficient data were not available because their
case files could not be retrieved were excluded from the study.
Statistical Analysis:
The data obtained were analyzed using
SPSS and presented as count, frequency and percentage. Continuous data were
expressed as mean/standard deviation while categorical data were analyzed
using Chi-square test and where necessary p-values less than 0.05 and
greater than 0.05 were regarded as significant and non-significant
respectively.
RESULTS
During the period, a total of 481 children were treated for
appendicitis at the center. They were aged between 2 and 16 years (mean 9.7
years � 2.8), comprising 265 males and 216 females with male/female
ratio1.2:1. Appendicectomy accounted for 5.7% of the total 8456 pediatric
operations and 47.5% of 1012 pediatric abdominal operations in ten years.
Majority of the patients, 361 (75.1%), were children who resided in semi-urban
and urban cities and whose parents belonged to the upper socioeconomic class
that were able to afford and consumed more westernized diets while 120 (24.9%)
were children of parents in low socioeconomic class. These children resided in
rural areas with their parents and consumed more of diets rich in roughages.
However, only 206 (42.8%) children presented to the unit directly within 24
hours of first episode of symptoms and in stable clinical state on arrival
while 275 (57.2%) were referred late after wrong diagnoses and treatment with
different complications.
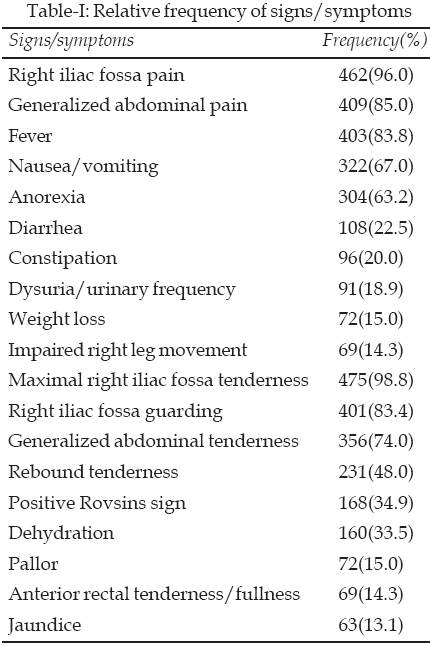
Table-I shows the relative frequency of the signs and
symptoms at presentation over ten years. Right iliac fossa pain 462 (96.0%)
was the most common symptom with the least common symptom being impaired right
leg movement and walking recorded in 69 (14.3%) children. Maximal right iliac
fossa tenderness was the most common sign as recorded in 475 (98.8%) with
jaundice recorded in 63 (13.1%) being the least frequent sign. The signs and
symptoms occurred in various combinations in especially those children who
presented with sub-acute and recurrent appendicitis. The classical signs and
symptoms of appendicitis were altered by medications taken before presentation
while many children already had complications on arrival. These resulted in
diagnostic difficulty in many of them.
Delayed referrals and complications were more among
children living in rural areas who did not seek medical attention early due
mainly to ignorance and financial constraints. Of the 275 children with late
referrals, 72 (26.2%) were referred from chemist shops after many years of
treatment of recurrent episodes of abdominal pain, while the others came from
private health institutions after 78 (28.4%) were treated for helminthes
infestations, 76 (27.6%) for typhoid enteritis and 49 (17.8%) for amoebic
dysentery. They were referred when they failed to respond to treatment with
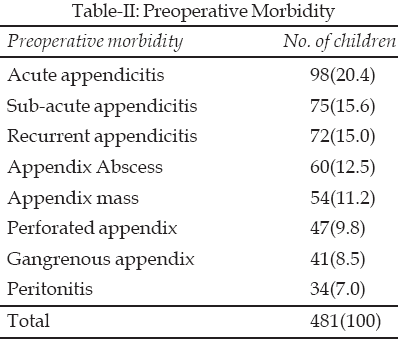
continued clinical deterioration. Due to late referrals, 236 children arrived
in the unit with life threatening preoperative morbidity ranging from appendix
abscess 60 (12.5%), appendix mass 54 (11.2%), perforated appendix 47 (9.8%),
gangrenous appendix 41 (8.5%) and peritonitis 34 (7.0%) which were confirmed
at exploratory laparotomy (Table-II). Therefore, an extremely significant
statistical difference was observed when post operative morbidity and
mortality recorded were compared between the children that presented early
without preoperative morbidity and those that presented late (P<0.0001).
Diagnostic imaging (abdominal ultrasound scan, CT scan and
plain abdominal X-rays) as well as relative leucocytosis on full blood count
were useful in making diagnosis, although appendicitis was correctly diagnosed
at exploratory laparotomy in 85 (17.7%) cases. Lanz incision centered at
McBurney�s point was the preferred access in those correctly diagnosed
preoperatively without features of peritonitis. Post operative morbidity was a
reflection of preoperative clinical state; hence post operative morbidities
were recorded among the 236 children who presented with complicated
appendicitis.
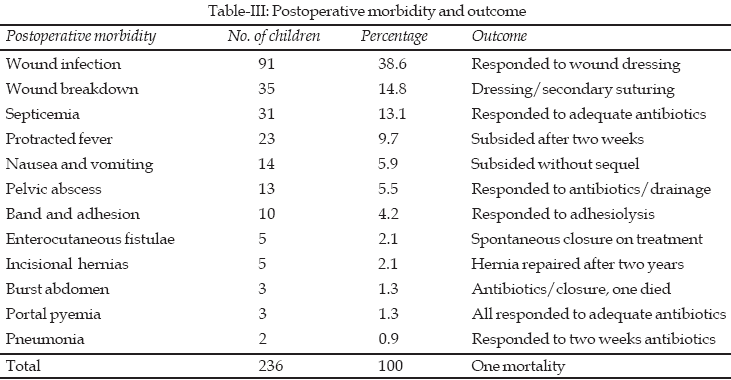
The post operative morbidity, their management and outcome
are shown in Table-III. Wound infection 91 (38.6%), wound break down 35
(14.8%), septicemia 31 (13.1%) and burst abdomen 3 (1.3%) were the most common
post operative complications resulting in prolonged hospital stay. Other
morbidities responded to treatment except one child with mortality recorded
among the 3 (1.3%) children with burst abdomen. Overall, 236 (49.1%) children
had post operative morbidities with 1 (0.2%) child succumbing to the illness
and no morbidity and mortality was recorded among children that presented
early and had appendicectomy. Also, mean hospital stay and total hospital
bills were 5 days � 2.1 and approximately 50 dollars � 0.2 respectively in
those that presented early, while those that presented late were 14 days � 2.8
and approximately 120 dollars � 0.9 respectively.
DISCUSSION
Rightly timed appendicectomy, open or laparoscopic, is the
gold standard treatment of inflamed appendix with an excellent outcome in
experienced hands. Neglected or wrongly managed appendicitis which allow
preoperative complications to occur is associated with life threatening post
operative morbidity as shown in this study and others.
9,10,16
Of the 481 children treated, only 206 (42.8%) presented early while 275
(57.2%) presented late, 236 (49.1%) of them with preoperative complications
that influenced post operative outcome. This resulted in an extremely
significant statistical difference observed when outcome was compared between
the children that presented early and those that presented late (P<0.0001)
which is similar to other results.1,2,9,16
The age/sex distribution of affected children in this study
tally with earlier reports but the incidence was much higher than what was
observed by earlier authors
3,4,12-15
which confirmed a steady increase in the incidence of appendicitis in
sub-Saharan Africa. In this study, appendicectomy accounted for 5.7% of total
pediatric operations and 47.5% of pediatric abdominal operations as against
0.43% and 18.0% in a similar research13
conducted a decade earlier in
western Nigeria. Also, appendicitis related morbidity due to delayed and
wrongly treated cases was correspondingly higher in this report than others4,13,14
which showed disparity between rising incidence of appendicitis and referrals
due to low index of suspicion by family doctors. Therefore, 78 (28.4%)
children in this series were treated for helminthes infestations, 76 (27.6%)
for typhoid enteritis and 49 (17.8%) for amoebic dysentery, and were referred
with complications when they failed to respond to the inappropriate treatment.5-7
Although clinical diagnosis of appendicitis is straight
forward in adult, it has been reported
8,17,18
to be more difficult in children
because of their inability to give accurate history, many differentials, lack
of cooperation during examination and absence of classical signs and symptoms,
which may be compounded by medications taken before presentation that may have
altered the clinical picture as shown in this study. In addition, the rapid
progression of appendicitis to complications in children and higher chance of
peritonitis due to poorly developed omentum as well as earlier literatures12,13
in this subregion which reported appendicitis to be uncommon in children led
to delay in presentation and diagnostic difficulty in many children in this
series which is similar to the experiences of earlier authors.8,18
Furthermore, preoperative morbidities recorded were more common and severe
among children who resided in rural areas that presented very late. Among such
children, life threatening preoperative morbidities, appendix abscess 60
(12.5%), appendix mass 54 (11.2%), perforated appendix 47 (9.8%), gangrenous
appendix 41 (8.5%) and peritonitis 34 (7.0%), were more frequent as reported
earlier.16,19
The importance of diagnostic imaging facilities in such cases have been
documented18,20
which would prevent negative appendicectomy when there is diagnostic
difficulty, but financial constraints in many developing countries make their
use to be restricted. Therefore, exploratory laparotomy which was diagnostic
as well as therapeutic was used more often in this series and others,14,15
in order to avoid further delay particularly in children with features of
peritonitis.
Consequent on wrong diagnosis and late referrals, post
operative wound infection in 91 (38.6%) children, wound break down 35 (14.8%),
septicemia 31 (13.1%) and pelvic abscess 13 (5.5%) were recorded which were
very challenging to manage and these resulted in prolonged hospitalization
with resultant increment in treatment bills as also reported by earlier
researcher.
1,2,10,21
Preoperative peritonitis has been reported to result in post operative band
and adhesion formation with resultant intestinal obstruction which may
necessitate re-exploration and adhesiolysis but these were rare in this series
(Table-II). Similarly, wound infections have resulted in incisional hernias
which are successfully repaired as seen in this and other studies.13,14
However, enterocutaneous fistula, portal pyemia and burst abdomen were
difficult post operative morbidities to manage in this study and one child who
had burst abdomen succumbed due to overwhelming sepsis. This is at variance
with previous report14
in this subregion in which no mortality was recorded despite similar spectrum
of post operative morbidity. The 0.2% mortality recorded in this study however
agreed with literatures1,2,10,21
but morbidity recorded in 236
(49.1%) children was exceptional.
CONCLUSION
In conclusion, the incidence of pediatric appendicitis is
rising in sub-Saharan Africa and the number of children treated in this review
was higher than earlier reports but under diagnosis, wrongly treated cases and
delayed referral which allowed life threatening complications to set in were
alarming. This is sequel to other causes of abdominal pains being given
priority as differential diagnosis because incidence of appendicitis was
believed to be very low in Nigerian children. However, appendicitis related
morbidity which led to increased length of hospitalization, cost of treatment
and mortality were worrisome, especially when no morbidity and mortality was
recorded in children that presented early and had timely appendicectomy.
Parents/caregivers should be suspicious of appendicitis and present children
with abdominal pain to hospital early. Physicians in this subregion should
give priority to appendicitis and refer children early for surgical
consultation because the classical clinical pictures of appendicitis may have
been altered by self medications before presentation.
REFERENCES
1. Young I, Moss KW. Acute appendicitis in children in a
community hospital: A five year review. Alaska Med 1997;39:34-42.
2. Rothrock SG, Pagane J. Acute appendicitis in children:
emergency department diagnosis and management. Ann Emerg Med 2000;36:39-51.
3. Mungadi IA, Jabo BA, Agwu NP. A review of appendicectomy
in Sokoto North-western Nigeria. Niger J Med 2004;13:240-243.
4. Nmadu PT, Dawam D. Childhood appendicitis in Zaria: A
retrospective study. East Afr Med J 1993;70:496-198.
5. Agugua NEN. Intestinal ascariasis in Nigerian children.
J Trop Pediatr 1983;29:237-9.
6. Uba AF, Chirdan LB, Huen AM, Mohammed AM. Typhoid
intestinal perforation in children. A continuing scourge in developing
country. Pediatr Surg Int 2007;23:33-9.
7. Adeniran JO, Taiwo JO, Abdul Rhaman LO. Salmonella
intestinal perforation: (27 perforations in one patient, 14 perforations in
another) are the goal posts changing? J Indian Assoc Pediatr 2005;4:248-51.
8. Lee SL, Ho HS. Acute appendicitis: is there a difference
between children and adults? Am Surg 2006;72:409-13.
9. Willmore WS, Hill AG. Acute appendicitis in a Kenyan
rural hospital. East Afr Med J 2001;78:355-57.
10. Cortesi N, Manenti A, Rossi A, Zanni C, Barberini G,
Gibertini G. Acute appendicitis and its postoperative complications. Apropos
of a series of 8738 cases. J Chir 1998;122:577-79.
11. Bekele A, Mekasha A. Clinical profile and risk factors
for perforation of acute appendicitis in children. East Afr Med J
2006;83:434-9.
12. Taiwo O, Hayemi SO, Seriki O. Acute appendicitis in
Nigerian children. Trop Georgr Med 1977;29:35-40.
13. Adejuyigbe O, Fadiora OA. Pattern of acute appendicitis
in Nigerian children. Ann Trop Pediatr 1989;9:93-7.
14. Achibong AE, Ekanem I, Jibrin P. Appendicitis in
South-eastern Nigerian Children. Cent Afr J Med 1995;41:94-7.
15. Ohene-Yoboah M, Togbe B. An audit of appendicitis and
appendicectomy in Kumasi, Ghana. West Afr J Med 2006;25:138-143.
16. Zoguereh DD, Lemaitre X, Ikoli JF, Delment J, Chamlian
A, Madaba JL, et al. Acute appendicitis at the National University Hospital in
Bangui, Central African Republic: epidemiologic, clinical, paraclinical and
therapeutic aspects. Sante 2001;11:117-125.
17. Holland A, Gollow IJ. Acute abdominal pain in children:
an analysis of admissions over a three year period. J Qual Clin Pract
1996;16:151-5.
18. Stamm D. Acute abdominal pain in children. Diagnostic
orientation. Rev Pract 2000;50:1923-30.
19. Okafor PI, Orakwe JC, Chianakwana GU. Management of
appendiceal masses in a peripheral hospital in Nigeria: review of thirty
cases. World J Surg 2003;27:800-03.
20. Weinberger E, Winters WD. Abdominal pain and vomiting
in infants and children: Imaging evaluation. Compr Ther 1997;23:679-86.
21. Perovic Z. Drainage of the abdominal cavity and complications in
perforating appendicitis in children. Med Pregl 2000;53:193-196.
HOME
| SEARCH
| CURRENT
ISSUE | PAST
ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@



