|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
April - June 2009 (Part-II) |
Number 3 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
April - June 2009 (Part-II) |
Number 3 |
||
|
|
||||
|
|
||||
Maternal risk factors affecting
newborn parameters
Oya Yucel1, Nursan Dede Cinar2
ABSTRACT
Objective: Pregestational body mass index (BMI) which is one of the best markers of nutritional status can be one of many variables affecting fetal growth. We wanted to determine the relations between various prepregnancy BMI categories, parity and newborn Ponderal indexes, birthweights in our population.
Methodology: For the assessment of the functional significance of BMI during pre-pregnancy, data from 264 women living in Sakarya were used. Maternal age, pregestational weight, height, parity were obtained from self-report at interview. We evaluated the relationship between maternal age, parity, pregestational weight and BMIs and newborn parameters as birthweight and Ponderal index.
Results: Average of the birth weight was 3.340±400gr, of the birth height was 50.53±1.66cm, of Ponderal index was 25.54±2.06. The mean of maternal BMI was 23.06±3.64, of parity was 2.14±1.17.
Conclusions: When BMI groups were compared with birthweight (p: 0.026) and parity (p: 0.02), it was observed that it had significant relationship. Statistical differences were not observed between maternal pregestational BMI and newborn Ponderal index (p:0.466). Nutritional conditions should be corrected in pregestational life to reduce the possibility of low birth weight newborn.
KEY WORDS: Body Mass Index, Ponderal Index, Prepregnancy, Birthweight, Maternal weight.
Pak J Med Sci April - June 2009 (Part-II) Vol. 25 No. 3 386-390
How to cite this article:
Yucel O, Cinar ND. Maternal risk factors affecting newborn parameters. Pak J Med Sci 2009;25(3): 386-390.
1. Oya Yucel, MD,
Asistant Professor,
2. Nursan Dede Çýnar, PhD,
Associate Professor,
1,2: School of Health Sciences,
Sakarya University,
Sakarya,
Turkey.
Correspondence
Dr. Nursan Dede CINAR,
Sakarya Üniversitesi Sađlýk Yüksekokulu,
Esentepe Campus,
54187 Sakarya,
Turkey.
E-mail: ndede@sakarya.edu.tr
* Received for Publication: November 26, 2008
* Accepted: May 7, 2009
INTRODUCTION
Women are exposed to different nutritional habits which contribute to women weight and body mass index. Pregestational body mass index (BMI) which is one of the best markers of nutritional status can be one of many variables affecting fetal growth.
1-4A number of anthropometric parameters have been used successfully for many years to estimate the prevalence of undernutrition in children. These include height for age, weight for age and Ponderal index. These are a part of the assessment of the overall nutritional status. The ponderal index can be comparable to body mass index, but generally it is used for evaluation of the newborn growth. It can help us learn the standardized measurements of newborn.
5,6 Because Ponderal index is an evaluation criteria of intrauterine fetal growth, reviewing of the interactions between mother’s nutritional status and fetus could be possible by evaluating the mother BMI and Ponderal index of newborn. In our study, it was aimed to determine the relations between various prepregnancy BMI categories, parity and newborn Ponderal indexes, birthweights in our population.METHODOLOGY
Study Group: For the assessment of the functional significance of BMI during pre-pregnancy, data from women living in Sakarya were used. The study included 264 women who had given birth to a liveborn singleton baby. Women with history of gestational diabetes, using tobacco, having multipl gestation or premature babies were excluded from our study. This is an analysis of data from a single hospital.
Study Parameters: Maternal age, pregestational weight, height and parity were obtained from self-report at interview. The maternal BMI was calculated by using pre-pregnant weight and height (kg/m˛). BMI was classified according to the IOM’s (Institute of Medicine) criteria; BMI is called underweight when it was equal and below 19.7, overweight between 26 and 29, obese equal and above 29. The values of BMI between 19.8 and 26 are accepted normal ( Institute of Medicine).
7 The underweight groups classified to be severely underweight and mildly underweight based on 18.5 value of BMI. Ponderal index is determined by the cube of birth height (cm) divided by the birth weight (kg).Study Design: Birth weights were classified to three groups; first group was including 2500gr and below babies, second group was between 2500gr / 4000gr and last group was 4000gr and above (macrosomia). Birthweights were compared with BMI groups, parity, pregestational weight and maternal age.
The relationship between maternal BMI groups and infant birthweights and Ponderal indexes were evaluated. Women were divided in four groups according to the number of their children. Fourth group was including grand multiparity (4 and more). Parity was also compared with infant Ponderal indexes and birthweights.
Statistical Analysis: Statistical analysis was done by using independent samples t-test and ANNOVA. Significance was set at 0.05. Post hoc comparisons were performed by the Tukey method. All data were analyzed with use of the SPSS (SPSS for Windows, version 12.0).
RESULTS
A total of 264 women participated in the study as volunteers. The mean age of the mothers was 26.31 ± 4.95 years (16-40), of father was 31.51 ± 7.60 years (18-66). Two hundred thirty of the mothers (87.1%) were between 20-34 years of age. 15 (5.7%) were less than 19 years of age and 19 out of them (7.2%) were older than 35 years of age.
The average of the newborn birthweights was 3303.8 ± 456.8gr, height was 50.5 ± 1.9 cm, head circumference was 34.6 ± 1.7cm and Ponderal Index was also found 25.36 ± 2.65. On the other hand, 91.3% of the baby (n.241) had birthweight in normal ranges. 4.5% (n.12) of newborn were below 2500gr and 4.2% (n.11) were above 4000gr. The average of maternal pregestational weight was found 60.4± 11.6kg, maternal height was 161.8±5.6 cm and gestational weight gaining was 13.8±6.1kg.
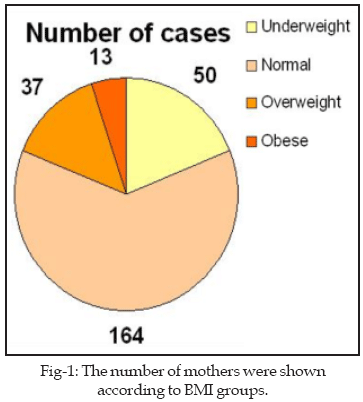
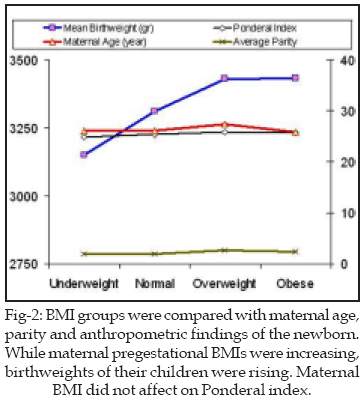
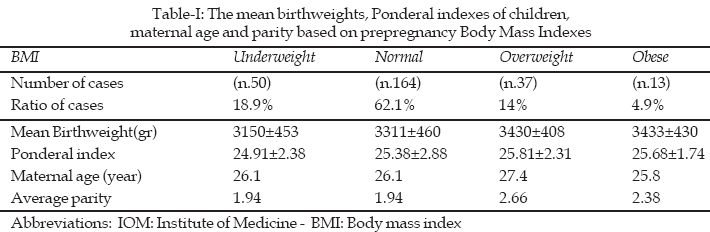
The average of BMI was found 22.95 ± 3.99 kg/m˛. The ratio of mothers according to BMI groups is shown in Fig-1. The mean values of the birthweight and Ponderal index based on prepregnancy BMI are shown in Table-I. When BMI groups were compared with birthweight (p:0.026) and parity (p:0.02), It was determined significant relation statistically. Statistical differences were not determined between maternal pregestational BMI and newborn Ponderal index (p:0.466). Parity was compared with birthweight and ponderal index. Any relations were not determined (p:0.674, p: 0.386). All these relations were shown in Fig-2.
Out of the mothers, ninety nine (37.5%) were primiparae and 165 (62.5%) were multiparae. The number of women with grand multiparity (more than 4) was 26 (9.8%). Eighty six out of the mothers had two children (32.6%), 53 mothers had three children (20%). The average BMI of pirimiparae was 22.28±4.07 and of multiparae was 23.35±3.90. Statistical difference was found significantly between groups (p:0.027). The average age of pirimiparae was found 23,93± 4,11 and was 27,84± 4,84 for multiparae.
DISCUSSION
Nutrition affects human life in every period. Women who have bad nutritional condition will carry risks for their life and siblings. Nutritional behaviour during prepregnancy and pregnancy period can also change the life quality and health of the newborn. It is important to understand the relations between prepregnancy nutrition and fetus growth,. BMI is influenced by ethnicity and genetic but may also serve as a measurement of adiposity and energy balance.
8 As maternal anthropometry differs among ethnic groups, data gathered for each population should be evaluated separately. It is clear that there are some differences about nutiritonal habits and food sources in different regions also. As such we wanted to investigate the results in our population.Low and high levels of maternal BMI could be important on the fetal growth. In our study, BMI values were classified according to the IOM’s criteria and groups were compared with anthropometric findings of the newborn (Institute of Medicine). Mothers with underweight BMI had babies with the lowest birthweight in our population. The average weight of the babies whose mothers had underweight BMI were found 3150gr. In contrast to, the average birthweights in overweight and obese mothers were 3480gr and 3365gr, respectively. Obesity is not a common problem in Turkey. For this reason, the number of obese mothers were low (n.13) in our series. But in this small group, the children of women with BMI above 30 had not birthweight of 4000gr or above as opposite to some previous reports.
8-11 We found that while increasing maternal BMI, birthweights were rising similar to Mitchell and colleague study. 12 But, Ponderal indexes were not changing with maternal pregestational BMI (Fig-2).Some authors have pointed out that severe underweight BMI was an important risk factor for reduced fetal growth.
2 The shorter and thinner women delivered babies with lower birthweight and height. The mean birthweight of newborns of the women with prepregnancy BMI under 19 was significantly low. It was claimed that prepregnancy BMI could predict fetal weight.3,4,13The cut-off values for IOMs criteria was equal and below 19.7kg/m˛ for underweight. The levels under 18.5kg/m˛ was defined thin women by some authors. Since, this cut-off value was the median for underweight group, the values below 18.5 are called severe underweight and above called moderately underweight.
2 It was thought that if we accepted these cut-off values to evaluate our cases, we would have wider point of view. The number of mothers with underweight BMI was found 50 in our study. Out of them, 32 were in the severe underweight group and 18 were moderately underweight group. It was found that the average birthweight and ponderal index of the children of these mothers were 3165gr and 25.11±2.38 in former group, 3127gr and 24.63±2.54 in latter group. We did not see any statistical difference for birthweight and ponderal index (p:0.794, p:0.547). Mitchell and colleagues have claimed that cut-offs of prepregnant BMI under 16 and 17 were spesific but not sensitive indicators for low birthweight.12 However, the number of women with under 17 of BMI was too low to interpret in our study (n.11).In our study, it was shown that while increasing parity, the maternal BMI were also increasing. But after the thirth birth, maternal BMI was not increasing anymore. At the same time, we could not find any relation between parity and newborn anthropometric parameters. The average parity for babies whose weights below 2500gr was also found 2.3. This value was 1.9 for babies with weight of 4000gr or above.
Ponderal index showing the fetal growth can change according to the number of parity. In some previous studies, it was claimed that the children of primiparae mothers had lower birthweight and while increasing parity, both mother BMIs and newborn birthweights were increasing.
5,6 BMI groups were checked in pirimiparae in our population. It was shown that they had lower BMI than multiparae. But, parity did not affect birthweight and Ponderal index, but maternal age could be an important factor for birthweight, Ponderal index and maternal BMI. In our study, the mothers were classified in three groups (19 years of age and below, between 20 and 34, 35 years of age and above) for evaluating the effects of the maternal ages on the birthweight and Ponderal index. It was observed only in 15 mothers under 19 years of age. It also showed that maternal age did not affect on maternal BMIs (p:0.901), newborn birthweights (p:0.688) and Ponderal indexes (p:0.263). At the same time, pregestational weight (p:0.695) and gestational weight gain (p:0.825) did not affect maternal age also. Most of the mothers under 19 years of age had normal BMI. The mean birthweight of their children was found 3350gr. This value was 3385gr for women above 35 years of age.In a study including 1205 multiparae, maternal pregestational weight percentiles were used to evaluate the relationship between maternal and newborn anthropometric measurements. It was claimed that prepregnancy weight was the best predictor of all newborn parameters.
1 Although our study included primiparae and multiparae cases, their results supported our data. The average maternal pregestational weight was almost 57kg for babies with birthweight below 2500gr, 60kg for babies with birthweight between 2500 and 4000gr, 70kg for babies with birthweight above 4000gr. The lower maternal pregestational weights had, the lower newborn birthweights.Although birthweights were rising with maternal pregestational BMI increasing, maternal pregestational weight was also found to be important factor on the newborn birthweight. Maternal pregestational weight affected Ponderal index. Fetal undernutrition may be assumed with low pregestational maternal weight. As such nutritional conditions should be corrected in pregestational life to reduce the possibility of low birth weight newborn.
REFERENCES
1. Neggers Y, Goldenberg RL, Cliver SP, Hoffman HJ, Cutter GR. The relationship between maternal and neonatal anthropometric measurements in term newborns. Obstet Gynecol 1995;85(2):192-6.
2. Ronnenberg A, Wang X, Xing H, Chen C, Chen D, Guang W. Low preconception body mass index is associated with birth outcome in a prospective cohort of Chinese women. J Nutr 2003;133(11):3449-55.
3. Thame M, Wilks RJ, Mcfarlane-Anderson N, Bennett FI, Forrester TE. Relationship between maternal nutritional status and infant’s weight and body proportion at birth. Eur J Clin Nutr 1997;51(3):134-8.
4. Yekta Z, Porali R, Aiatollahi H. The effect of prepregnancy Body Mass Ýndex, gestational weight gain on pregnancy outcomes. BMC Pregnancy Childbirth 2006;6:15:1-8.
5. Juntunen KST, Laara EMJ, Kauppila AJI. Grand grand multiparity and birth weight. Obstet Gynecol 1997;90(4):495-9.
6. Laffineuse L, Goodwin A, Collin M, Mercer B. Impact of change of maternal body mass index between pregnancies on the risk of recurrent term low birth weight. Am J Obstet Gynecol 2005;193(6):171.
7. Institute of Medicine. Committee on nutiriton status during pregnancy and Lactation. Nutrition during pregnancy, National Academy Press; 1990 Washington (DC):81-2.
8. Schieve LA, Cogswell ME, Scanlon KS, Perry G, Fere C, Blackmore-Prince C, et al. Prepregnancy body mass index and pregnancy weight gain: associations with preterm delivery. Obstet Gynecol 2000;96(2):194-200.
9. Caulfield LE, Haris SB, Whalen EA, Sugamori M. Maternal nutritional status, diabetes and risk of macrosomia among Native Canadian women. Early Human Development 1998;50(3):293-303.
10. Ehrenberg HM, Mercer BM, Catalano PM. The influence of obesity and diabetes on the prevalence of macrosomia. Am Obstet Gynecol 2004;191(3):964-8.
11. Sukalich S, Mingione MJ, Glantz JC. Obstetric outcomes in overweight and obese adolescents. Am Obstet Gynecol 2006;195(3):851-5.
12. Mitchell MC, Lerner E. Weight gain and pregnancy outcome in underweight and normal weight women. J Am Diet Assoc 1989;89:634-8.
13. Copper RL, Dubard MB, Goldenberg RL, Oweis AI. The relationship of maternal attitude toward weight gain to weight gain during pregnancy and low birth weight. Obstet Gynecol 1995;85(4):590-5.
14. Szostak-Weigerek D, Szamotulska K, Szponar L. Influence of maternal nutrition on birthweight (abstract). Ginekol Pol 2004;75(9):692-8.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk