|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
CASE REPORT |
||||
|
- |
||||
|
Volume 24 |
July - September 2008 |
Number 4 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
CASE REPORT |
||||
|
- |
||||
|
Volume 24 |
July - September 2008 |
Number 4 |
||
|
|
||||
|
|
||||
Neurobrucellosis: Report of A case
with CVA manifestation
Behzad Mohsenpour1, Payam Khomand2, Ebrahim Ghaderi3
Summary
Although neurological symptoms in brucellosis are frequent, central nervous system (CNS) involvement is uncommon. A 42-year-old man was admitted with an episode of faint without loss of consciousness, right hemi paresis, diplopia and headache lasting for four days. The neurological examination revealed left hemi paresis. Limitation of gazing in left eye in lateral view was seen (partial paresis of 6th cranial nerve). The results of laboratory examinations show positive Wright and Coombs Wright in blood and C.S.F. In the brain CT scan hydrocephaly and in magnetic resonance imaging (MRI) some brain atrophy, few high signal foci in the deep with mater had been detected. Treatment included concurrent administration of three drugs: doxycycline, rifampicin and co-trimoxazole. This patient fully recovered.
We suggest that Neurobrucellosis (NB) should always be sought in young patients with ischemic stroke, especially if they do not have any additional risk factors for stroke and live in an endemic area for brucellosis, even if they do not have other systemic signs of brucellosis.
KEYWORDS: Brucellosis, Ischemic stroke.
Pak J Med Sci July - September 2008 Vol. 24 No. 4 614-617
How to cite this article:
Mohsenpour B, Khomand P, Ghaderi E. Neurobrucellosis: Report of one case with CVA manifestation. Pak J Med Sci 2008;24(4):614-7.
1. Behzad Mohsenpour, M.D & MPH,
Infectious Diseases Specialist,
Tohid Hospital,
Sanandaj, Iran.
2. Payam Khomand, MD
Neurologist, Neurology Department,
Tohid Hospital,
Sanandaj, Iran.
3. Ebrahim Ghaderi, MD
General Practitioner,
Communicable Diseases Expert
of Disease Control And Prevention Group of
Kurdistan Province�s Health Centre,
Sanandaj, Iran.
Correspondence
Behzad Mohsenpour,
Address: Abidar Ave,
Kurdistan Province�s Health Centre,
Sanandaj, Iran.
Email: behzadmohsenpour@yahoo.com
* Received for Publication: January 25, 2008
* Accepted: June 4, 2008
INTRODUCTION
Brucellosis, a zoonosis disease that affects animals as the primary host (e.g. camels, sheep and goats) and humans as the secondary host,
1 is still a common health problem in some Middle Eastern & Mediterranean countries.1-4 Nervous system involvement occurs approximately in 2�10% of the patients infected with brucella.1-7 Neurobrucellosis (NB) may develop at any stage in the evolution of the disease and may involve several areas of the central and peripheral nervous system. Therefore, NB has widely variable manifestations, including meningoencephalitis, myelitis, radiculitis, neuritis, spinal cord compression and demyelinative or vascular diseases of the central nervous system (CNS), or any combination of these disorders.4-8The most typical presentation of CNS involvement in brucellosis is chronic meningoencephalitis with mononuclear pleocytosis, decreased glucose and increased protein concentrations in the cerebrospinal fluid (CSF).
7 Uncommon clinical presentations of NB such as migraine, Parkinsonism, optic neuritis, chronic intracranial hypertension and epilepsy have been reported.4,8-11 Brucellar meningitis may also behave as an exclusively neurological disease mimicking vascular accidents that are frequently paroxysmal and recurrent.1,2,4 Here we report one case with brucellosis as an exceptional cause of C.V.A.CASE REPORT
A 42-year-old man was admitted with an episode of faint without loss of consciousness, right hemi paresis, diplopia and headache for the last four days. The patient had also shoulder and neck pain and anorexia from last two months. He had no history of hypertension, diabetes and others chronic diseases. This patient was farmer.
In general physical examination fever (38.7�C) was detected. Blood pressure was 110/70mmHg and pulse 86/min. Examination of heart and lungs were normal. The neurological examination revealed right hemi paresis and upward plantar reflex on the left side. Limitation of gazing in left eye in lateral view was seen (partial paresis of 6
th and 7th left side cranial nerves). The patient was evaluated for stroke in young adults.
Results of laboratory examination is shown in Table-I. In blood sample leucocytosis (85% neut), positive Wright and Coombs Wright was seen. C.S.F was Wright positive. The platelet count, BUN, Cr, Cholesterol, T.G, Uric Acid, Na, K, PTT, PT, U/A, vasculitis tests and echocardiography were normal.

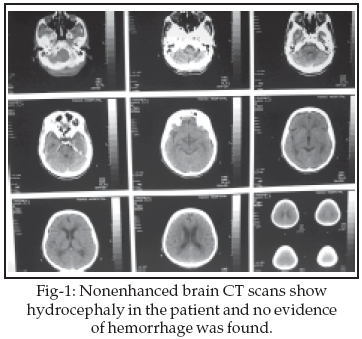
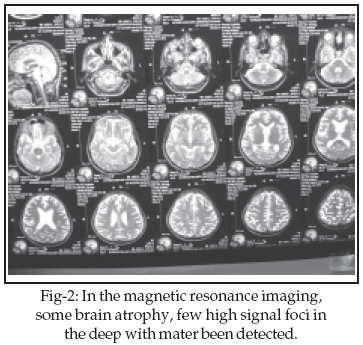
In the primary brain CT no lesion was seen but some days later hydrocephaly has been detected. In brain magnetic resonance imaging (MRI), some brain atrophy and few high signal foci in the deep white matters of both brain hemisphere was reported. There was not any S.O.L in the supra and infra tentorial structures.
DISCUSSION
Brucellosis, although almost eradicated in many parts of the world, still remains widespread and endemic in the developing countries.
3,4,7 Neurological involvement during the course of brucellosis occurs in about 2�10% of the cases.5,6,13 Clinical diagnosis of NB can be very difficult because of various presentations. Several clinical forms of brucellosis affecting the CNS have been reported including meningitis, meningoencephalitis, myelitis, myelopathy and demyelinative or vascular diseases of the CNS.2-5,7Our patient presented with an episode of neurological deficit that was compatible with right hemi paresis and dysfunction of 6
th and 7th left side cranial nerves. The endemic occurrence of brucellosis in Kurdistan, positive serology in serum and CSF for brucellosis, exclusion of other vascular diseases and causes of ischemic cerebral symptoms, and good response to treatment with antibiotics led to the diagnosis of NB. A similar clinical presentation of NB was also reported by other authors and defined as transient brief attacks or intermittent cerebral vascular insufficiency.3,4,7,14Bingol reported four case with transient ischemic attacks (TIA) or ischemic stroke as the predominant manifestation of neurobrucellosis. In one patient transient brief attacks followed by a ruptured basilar artery aneurysm and in another one accompanied by xanthochromia.
4 But as in ours, most of the patients with ischemic cerebral symptoms in Bingol reporte and other report have normal cerebral angiograms.4,13Al-Deeb has reported a man who presented with dysarthria and left hemiplegia of acute onset and his CT showed a frontoparietal infarct, but cerebral DSA was normal. The authors proposed that normal appearance of cerebral vessels in DSA was consistent with vasculitis of deep penetrating arteries.
7 Three types of imaging abnormalities can be seen in neurobrucellosis: inflammation, white matter changes, and vascular insult. Inflammation may cause granulomatous formation or enhancement of the meninges, perivascular space, or lumbar nerve roots.1As a manifestation of basal meningeal infection, involvement of one or more cranial nerves has been noted in more than 50% of the cases.
13 The vestibulocochlear nerve has been described as the most frequently involved cranial nerve in NB. Its involvement is usually combined with other neurological dysfunctions.3,4,15 Neurobrucellosis may develop at the onset of the illness, during convalescence or months to years after recovery from the acute systemic infection.4The pathogenesis of TIA and ischemic stroke in brucellosis still remains uncertain. It has been proposed that TIA in brucellosis may be related to infectious vasculitis, cerebral vasospasm or cardioembolism.
7,14 Various degrees of vascular inflammation ranging from acute to chronic with the possibility of necrosis and aneurysmal formation has been described in CNS brucellosis.4The final diagnosis of NB was made on the basis of the serological tests or culture for brucella in CSF. Other criteria supporting our diagnosis were: a history of consumption of unpasteurized milk or milk products, systemic complaints of brucellosis, such as headache, malaise, weight loss, anorexia, dorsal pain and nausea-vomiting, progressive bilateral sensorineural hearing loss without any other cause, C.V.A not associated with other well-known risk factors of ischemic stroke, lymphocytic pleocytosis in CSF with increased level of protein, and decreased level of glucose.
In chronic NB, increased IgG index and/or oligoclonal banding pattern in CSF electrophoresis can be detected as in many other chronic inflammatory processes of the CNS.
4,16 Normal levels of IgM in serum and CSF also indicated that the infection was in the chronic stage.Trimethoprim/sulfamethoxazole, rifampicin and doxycycline which have good intracellular and CNS penetration and which are synergistic are the most commonly used antibiotics to treat brucellosis. Prolonged treatment (at least 6 months) with a combination of these three antibiotics was used in our patients successfully.
As Bingol
8 concluded, recognition of ischemic stroke because of brucellosis and its differentiation from other vascular diseases are not easy, particularly in elderly patients with stroke risk factors such as hypertension, diabetes, atrial fibrillation, etc. We suggest that NB should always be sought in young patients with ischemic stroke, especially if they do not have any additional risk factors for stroke and live in an endemic area for brucellosis, even if they do not have other systemic signs of brucellosis.REFERENCES
1. Al-Sous MW, Bohlega S, Al-Kawi MZ, Alwatban J, McLean DR. Neurobrucellosis: Clinical and Neuroimaging Correlation. Am J Neuroradiol 2004;25(3):395-401.
2. Adeva-Bartolome MT, Montes-Martinez I, Castellanos-Pinedo F, Zurdo-Hernandez JM, De Castro-Garcia FJ. Neurobrucellosis: four case reports. Rev Neurol 2005;15:41(11):664-6.
3. Lee M, Fung K. A case of human brucellosis in Hong Kong. Hong Kong Med J 2005;11(5):403-6.
4. Bingol A, Togay-Isikay C. Neurobrucellosis as an exceptional cause of transient ischemic attacks. Eur J Neurol 2006;13(5):544-8.
5. Shakir RA, Al-Din ASN, Araj GF, Lulu AR, Mousa AR, Saadah MA. Clinical categories of neurobrucellosis. A report on 19 cases. Brain 1987;110(1):213-23.
6. Bahemuka M, Shemena AR, Panayiotopoulus CP, Al-Aska AK, Obeid T, Daif AK. Neurological syndromes of brucellosis. J Neurol Neurosurg Psychiatry 1988;51(8):1017-21.
7. Al Deeb SM, Yaqub BA, Sharif HS, Phadke JG. Neurobrucellosis clinical characteristics, diagnosis and outcome. Neurology 1989;39(4):498-501.
8. Bingol A, Yucemen N, Meco O. Medically treated intraspinal _Brucella_ granuloma. Surgical Neurology 1999;52(6):570-6.
9. Diaz Espejo CE, Villalobos Chaves F, Sureda Ramis B. Chronic intracranial hypertension secondary to neurobrucellosis. J Neurol 1987;234(1):59-61.
10. Abd Elrazak M. Brucella optic neuritis. Arch Intern Med 1991;151(4):776-8.
11. Yilmaz M, Ozaras R, Ozturk R, Mert A, Tabak F, Aktuglu Y. Epileptic seizure: an atypical presentation in an adolescent boy with neurobrucellosis. Scand J Infect Dis 2002;34(8):623-5.
12. Al-Orainey IO, Laajam MA, Al-Aska AK, Rajapakse CN. Brucella meningitis. J Infect 1987;14(2):141-5.
13. Pascual J, Combarros O, Polo JM, Barciano J. Localized CNS brucellosis: Report of 7 cases. Acta Neurologica 1988;78(4):2829.
14. McLean DR, Russell N, Khan MY. Neurobrucellosis: clinical and therapeutic features. Clin Infect Dis 1992;15(4):582-90.
15. Thomas R, Kameswaran M, Murugan V, Okafor BC. Sensorineural hearing loss in neurobrucellosis. J Laryngol Otol 1993;107(11):1034-6.
16. Sanchez-Sousa A, Torres C, Campello MG, Garcia C, Parras F, Cercenado E, et al. Serological diagnosis of neurobrucellosis. J Clin Pathol 1990;43(1):79-81.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk