|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
July - September 2009 |
Number 4 |
||
|
|
||||
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
July - September 2009 |
Number 4 |
||
|
|
||||
|
||||
Early prediction of severity and outcome
of acute severe pancreatitis
Syed Sagheer Hussian Shah1, M. Ali Ansari2, Shazia Ali3
ABSTRACT
Objective: To establish the value of APACHE II scoring system, C-reactive Protein (CRP) level and C.T Severity Index (CTSI) in predicting the severity of acute pancreatitis.
Methodology: A prospective study was done in the Department of General Surgery, Jinnah Postgraduate Medical Centre, Karachi, over a period of one year i.e. from January to December 2007. Fifty patients of acute pancreatitis were taken and their outcome and severity was assessed by using APACHE II score, CRP level and CTSI.
Results: At the end of the study results showed that thirty eight (76%) patients were young females, most of which had gall stone pancreatitis, twenty-one patients (42%) had severe acute pancreatitis, twenty two (44%) patients had length of hospital stay of two or more than two weeks, in 21 patients (42%) patients APACHE II score was more than 8, in 21 patients (42%) CRP level was more than 120mg/l, CTSI showed that eighteen (36%) had three points and three (6%) had four points. Three patients (6%) expired within 72 hours of admission due to advanced age, uncontrolled sepsis and co-morbids.
Conclusion: The severity markers used in this study showed significant importance in prediction of severity of acute pancreatitis. Particularly Apache II scoring system and CTSI.
KEY WORDS:
APACHE II score, CT Severity Index (CTSI), C-reactive Protein (CRP).Pak J Med Sci July - September 2009 Vol. 25 No. 4 619-623
How to cite this article:
Shah SSH, Ansari MA, Ali S. Early prediction of severity and outcome of acute severe pancreatitis. Pak J Med Sci 2009;25(4): 619-623.
1. Dr. Syed Sagheer Hussian Shah, FCPS,
Associate Professor of Surgery,
Surgical Unit- III,
2. Dr. M. Ali Ansari, FCPS
Trainee general Surgery,
3. Dr. Shazia Ali, FCPS,
Trainee General Surgery,
2,3: Surgical Unit- II,
1-3: Jinnah Postgraduate Medical Centre,
Karachi - Pakistan.
Correspondence
Syed Sagheer Hussain Shah, FCPS
Associate Professor of Surgery,
Dept. of General Surgery,
Surgical Unit- II
Jinnah Postgraduate Medical Centre,
Karachi – Pakistan.
Email:
syedsagheer_shah@yahoo.com
* Received for Publication: February 9, 2009
* Revision Received: June 11, 2009
* Revision Accepted: June 21, 2009
INTRODUCTION
A large number of the patients with acute pancreatitis develop severe disease which is life threatening with a high mortality rate. Early identification of patients at risk of developing a severe attack of acute pancreatitis (AP) is of great importance because rapid therapeutic interventions improve outcome. In most cases, acute pancreatitis is a mild self limiting disease without complications, but acute necrotizing pancreatitis, which occurs in 20% of the attacks, is a life threatening disease with high morbidity and mortality. Improved outcome in the severe form of AP is based on early identification of disease severity and subsequent management of high risk patients in intensive care units with early endoscopic retrograde cholangiopancreatography (ERCP) in gallstone induced disease, early enteral feeding, and prophylactic antibiotics.
1-4One good reason for early assessment of severity in acute pancreatitis is that this could discount the majority of cases that are mild and have a self limiting course and do not require any treatment other than general support and parenteral fluid for a few days. In the past few years there have been some progress in the treatment of acute severe pancreatitis. Among the emerging new modalities are cytokine inhibitors and different anti-inflammatory regimes. Furthermore, there are randomized studies showing that patients with severe acute pancreatitis benefit from early prophylactic treatment with potent antibiotics.
5,6 It is also suggested that the patients with acute severe gall stones induced pancreatitis should undergo endoscopic sphincterotomy as early as possible (within 24 to 48 hours of admission).7 It can not be ruled out that treatment with protease inhibitors could re-emerge as a treatment option. It has been shown to be of value in a meta-analysis,8 provided that the therapy can be started early enough, and also as a prophylactic treatment to prevent ERCP induced acute pancreatitis.9 All these possible treatments must be instituted at a very early stage in the disease, as the chances for success diminishes rapidly with time. Moreover, these therapies are expensive and not without complications, and most importantly, the vast majority of patients with acute pancreatitis will not benefit, as their pancreatitis is mild and self limiting. Therefore, there is even greater need for simple markers for severity, which can provide reliable information.The objective of conducting this study was to apply the established parameters for assessment of acute severe pancreatitis in our population and compare the results with studies done in other parts of world.
METHODOLOGY
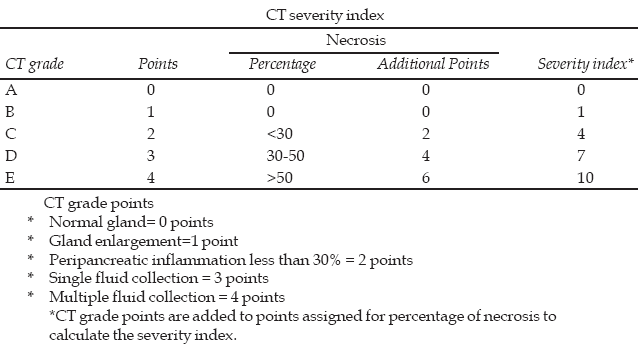
The medical record of patients with a confirmed diagnosis of acute pancreatitis that were admitted in the department of general surgery, JPMC between Jan to Dec 2007 was reviewed. Fifty patients admitted for the management of acute pancreatitis and its complications were included in the study. Their demographic data, duration of symptoms at presentation, cause of acute pancreatitis, the APACHE II score (in first 24 and 48 hours), CRP level, C.T scan abdomen findings (pancreatic necrosis, acute pancreatic pseudocyst or pancreatic abscess) organ failure (if any) interventional procedures (if done) outcome and length of hospital stay were recorded in the structured proforma. Cutoff value for APACHE II score was 9 & for CRP level 120mg/dl. The CTSI is scored as:
An arbitrary cutoff of five hospital days was used to exclude patients with mild episodes of acute pancreatitis. In addition, patients remaining in the hospital for elective cholecystectomy after resolution of acute pancreatitis were excluded.
RESULTS
Out of fifty patients, 38 (76%) were females and 12 (24%) males, with a ratio of 3:1. Age range was 18 to 70 years with a mean of 42± years, fourteen (28%) subjects were less than 35 years, twenty five (50%) in the age bracket of 35-50 years and sixteen (32%) more than 50 years. All the patients presented with acute abdominal pain, in forty five (90%) the commonest site of pain was epigastrium and in five (10%) it was in epigastrium and right hypochondrium. It was severe in nature and radiated to the back in most of the patients.
The duration of pain on admission ranged from 4 to 24 hours, in seventeen patients (34%) it was less than 12 hours. The complaint of nausea and vomiting was reported by all fifty (100%) patients, twenty five (50%) presented with fever (low to high grade). On general physical examination tachycardia of more than 120b/min was present in 40 patients (80%) and tacypnea of, more than 35 b/min was found in twenty eight patients. Baseline investigations and abdominal ultrasound was performed in all patients.
APACHE II score was calculated within 24 hours of admission in all patients, twenty nine (58%) had a score of less than 7 and in twenty one (42%) it was more than 8. CRP levels came checked after 48 hours and in twenty one (42%) patients (who had an apache score of more than 8) it was more than 120mg/dl, which is indicative of severe inflammation, as reported in previous studies.
10 Intravenous contrast enhanced abdominal CT scan was performed to assess the status of pancreas and to calculate CTSI in these patients. The CTSI was calculated from the extent of pancreatic inflammation, necrosis and the presence or absence of fluid collections. In the present study twenty nine (58%) patients had CTSI of two points, eighteen (36%) had three points and three (6%) had four points.Endoscopic retrograde cholangiopancreato-graphy (ERCP) was performed in 15 (30%) patients with clinical and laboratory evidence of jaundice or ultrasonographic or CT scan evidence of CBD stones. No stone was detected in the CBD in five patients, in remaining ten patients, endoscopic sphincterotomy was performed for removal of CBD stones after which jaundice relieved and patients improved gradually.
Cholelithiasis was the most common etiological factor, which was present in thirty-five (70%) patients, three patients had history of alcohol consumption, in rest twelve patients etiology remained undiagnosed (idiopathic) at the time of discharge (30%) no cause was detected. Forty two (84%) patients settled on conservative treatment, eight (16%) patients underwent surgical intervention in the form of laparotomy, washout and drain placement. Twenty-one (42%) patients with severe acute pancreatitis required ICU support. Three (6%) patients expired within 72 hours of admission due to uncontrolled sepsis and co-morbids. Twenty two (44%) patients had length of hospital stay of more than two weeks and twenty eight (56%) patients stayed for less than two weeks; mean stay at hospital was two weeks.
DISCUSSION
Improved outcome in severe AP is based on early identification of disease severity. In the study of Brivet et al,
1 patients admitted to the intensive care unit after a delay of >24 hours had a fourfold risk of dying. Accurate predictors of severity in the early phase of the disease are needed to direct appropriate measures for immediate treatment and subsequent disease are needed to direct appropriate measures for immediate treatment and subsequent management of these high risk patients in clinics specialized in the treatment of patients with severe AP. On the contrary, patients accurately identified to have mild disease may be fairly safely treated on low-cost wards, which is important because of limited health care resources.The APACHE II score was devised as a prognostic scoring system in critically ill patients requiting ICU care.
11 The APACHE II score provides an immediate physiologic assessment of individual patients, in conjunction with there age and co morbidity. Researchers12-14 have preferred the APACHE II score to other prognostic scoring system for severe pancreatitis, such as Ranson criteria, because the APACHE II score can be determined at hospital admission. For example, in a study of 290 attacks of acute pancreatitis, only 59 (20%) of which were classified as severe, Larvin and McMahon13 found the APACHE II score to be accurate at identifying patients with severe acute pancreatitis, organ failure, and death, thus proving the importance of its measurement at hospital admission. During the past two decades, the outcome of severe acute pancreatitis has significiantly improved and the overall mortality has significantly decreased to less than 15% in patients with severe pancreatitis. A small sub group accounts for most of the deaths, and this includes patients who develop the fulminant course (3 deaths in our study) and patients who require multiple debridements associated with prolonged ICU care and hospitalization and high mortality.To our knowledge, the role of the prognostic systems has not been previously defined in identifying the subgroup with a poor outcome in a predetermined population of the patients with severe pancreatitis. With this intent, in the present study, we examined the relationship between the APACHE II score and an adverse outcome in a group of patients with severe pancreatitis. Twenty one patients (42%) in this study had severe disease; they were admitted to the ICU and evidence of organ failure (>1 organ) developed in nine patients (18%). The APACHE II scores accurately predicted the presence of severe pancreatitis, organ failure, and death. Furthermore, patients dying of acute pancreatitis had significant deterioration in their APACHE II scores within first 24 hours of admission compared with survivors. Deteriorating APACHE II scores at 48 hours after admission were found in 5 of 9 patients who died. Our results suggest a role for the APACHE II score in risk stratification in patients with severe pancreatitis. Furthermore, deteriorating APACHE II scores in 48 hours after admission may be an ominous signs that may predict late deaths from severe acute pancreatitis. In yet another study the authors have highlighted why APACHE II scoring system can serve as a better prognostic tool in our set up.
15Another marker for assessment of severity in this study was C-reactive protein (CRP) level. CRP is an acute phase reactant that is synthesized by the hepatocytes. This synthesis is induced by the release of interleukin one and six. Thus the CRP peak in serum is usually not maximal until about day three after the onset of pain, and is always later than the peak of these interleukins. CRP is the most popular single test severity marker used today. The only problem is that CRP is a rather late severity marker (day 2-4) as compared to the other markers. Cut-off levels have been discussed in literature, and levels between 120 and 210/L have generally been agreed upon as distinguishing between the mild and the severe disease.
16,17 Levels above 120mg/L after one week also distinguish severity well.16,18 In the present study the same cut off values are used and CRP levels ranges from 120-210 in our patients, 21 patients (42%) had more than 120mg/L, in rest patients it was not significantly raised. The third marker of severity in our study was the CTSI. A recent study by Simchuck et al19 has shown the prognostic value of the CTSI in patients with severe acute pancreatitis. In patients with a CTSI greater than five, there were a 8-fold higher risk of death and a 10-fold higher chance of the need for necrosectomy. In yet another study the authors have highlighted why APACHE II scoring system can serve as a better prognostic tool in our set up.15CONCLUSION
In our study, while highly significant associations were found with three measures of outcome and the overall predictive accuracy was high. Clearly improved risk stratification is necessary for patients with severe acute pancreatitis. Future research directed vat CT-based morphological criteria, pathophysiological scoring systems, or a combination of both may identify the subgroup of sick patients with an adverse outcome in those with severe acute pancreatitis and may provide an opportunity for targeted therapy to improve care for these patients.
REFERENCES
1. Brivet FG, Emilie D, Galanaud P. Pro- and anti-inflammatory cytokines during acute severe pancreatitis: an early and sustained response, although unpredictable of death. Parisian Study Group on Acute Pancreatitis. Crit Care Med 1999;27:749-755.
2. Schmid SW, Uhl W, Friess H, Malfertheiner P, Buchler MW. The role of infection in acute pancreatitis. Gut 1999;45:311-6.
3. Sharma VK, Howden CW. Meta analysis of randomized controlled trials of endoscopic retrograde cholangiopancreatography and endoscopic sphincterotomy for the treatment of acute biliary pancreatits. Am J Gastroenterol 1999;94:3211-4.
4. Windsor AC, Kanwar S, Li AG, Barnes E, Gutherine JA, Spark JI, et al. Compared with parenteral nutrition, enteral feeding attenuates the acute phase response and improves disease severity in acute pancreatitis. Gut 1998;42:431-5.
5. Pederzoli P, Bassi C, Vesentini S, Compedelli A. A randomized multicenter clinical trial of antibiotic prophylaxis of septic complications in acute necrotizing pancreatitis with imipenam. Surg Gynecol Obstet 1993;176:480-3.
6. Sainio V, Kemppainen E, Puolakkainen P, Taavitsainen M, Kivisaari L, Valtonen V, et al. Early antibiotic treatment in acute necrotizing pancreatitis. Lancet 1995;346:663-7.
7. Neoptolemos JP, Carr-Locke DL, London NJ, Bailey IA, James D, Fossard DP. Controlled trial of urgent endoscopic retrograde cholangiopancreatography and endoscopic sphincterotomy versus conservative treatment for acute pancreatitis due to gallstones. Lancet 1988;2:979-83.
8. Messori A, Rampazzo R, Scroccaro G, Olivato R, Bassi C, Falconi M, et al. Effectiveness of gabexate mesilate in acute pancreatitis. A metaanalysis. Dig Dis Sci 1995;40:734-8.
9. Cavallini G, Tittobello A, Frulloni L, Masci E, Mariani A, Di Francesco V. Gabexate for the prevention of pancreatic damage related to endoscopic retrograde cholangiopancreatography. N Eng J Med 1996;335:961-3.
10. Triester SL, Kowdley KV. Prognostic factors in acute pancreatitis. J Clin Gastroenterol 2002;34:167-76.
11. Knuas WA, Draper EA, Wagner DP, Zimmerman JE. APACHE II; a severity of disease classification system. Crit Care Med 1985;13:818-29.
12. Wilson C, Heath DI, Imrie CW. Prediction of outcome in acute pancreatitis: a comparative study of APACHE II, clinical assessment and multiple factor scoring systems. Br J Surg 1990; 77:1260-4.
13. Larvin M, McMahon MJ. APACHE II score for assessment and monitoring of acute pancreatitis. Lancet 1989;2:201-5.
14. Dominguez-Munoz JE, Carballo F, Garcia MJ, de Diego JM, Campos R, Yangüela J, et al. Evaluation of the clinical usefulness of APACHE-II and SAPS systems in initial prognostic classification of acute pancreatitis: a multicenter study. Pancreas 1993;8:682-6.
15. Zakri RH, Khaliq T, Inam A, Asghar T. Prognostication of acute severe pancreatitis: which one of Ranson’s and the APACHE II scoring system can serve as better prognostic tool in our set up? Annals Pak Ins Med Sci 2006;2(4):256-259.
16. Wilson C, Heads A, Shenkin A, Imrie CW. C-reactive protein, antiproteases and complement factors as objective markers of severity in acute pancreatitis. Br J Surg 1989;76:177-81.
17. Appelros S, Petersson U, Toh S, Johnson C, Borgstrom A. Activation peptide of carboxypeptidase B and anionic trypsinogen as early predictors of severity of acute pancreatitis. Br J Surg 2001;88:216-21.
18. Beutler B, Cerami A, Cachectin: more than a tumor necrosis factor. N Eng J Med 1987;316:379-85.
19. Simchuk EJ, Traverso LW, Nukui Y, Kozarek RA. Computed tomography severity index is a predictor of outcomes for severe pancreatitis. Am J Surg 2000;179:352-5.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@