|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
July - September 2009 |
Number 4 |
||
|
|
||||
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
July - September 2009 |
Number 4 |
||
|
|
||||
|
||||
Disseminated intravascular coagulation
in Abruptio Placentae
Yasmeen Khooharo1, Fayaz Ahmed Memon2, Khursheed Jhan Noorani3
ABSTRACT
Objectives: To assess the proportion of Disseminated Intravascular Coagulation (DIC) in abruptio placentae and outcome of such patients with DIC.
Methodology: This Descriptive study was conducted in the Department of Obstetrics and Gynecology (OBG) ward 8, unit -1 at Jinnah post Graduate Medical Centre (JPMC) Karachi from 1st January, 2001 to 31 December 2002. This study was carried out on 100 diagnosed cases of abruptio placentae; and its adverse effects were noted on haemostatic system. Patients who came through the Emergency Department of (OBG) or Main Emergency of JPMC with a history of ante partum hemorrhage was included in this study. Written consent was taken from patients for using information regarding history, clinical Examination and related investigations for the research purpose.
Results: DIC was found in seven out of 100 patients, they were relatively younger and Multiparous. Mean age was 27.5 years while parity ranged between Para 5-11 with mean gestational age of 33.14 weeks. Six (85.7%) patients had severe vaginal bleeding, abdominal pain and uterine tenderness. Coagulation profile and routine laboratory investigations revealed that all patients had raised fibrin degradation products, clotting, and prothrombin and activated thromboplastin time, while decreased serum fibrinogen, platelets and hemoglobin. All cases were immediately managed with fluid replacement and blood transfusion. Six (85.7%) cases were delivered by spontaneous vaginal delivery and only one (14.3%) case by caesarean section. Fetal mortality was high 6 (85.7%) all were fresh still birth while only one (14.3%) baby was alive. There was no maternal death.
Conclusions: The proportion of DIC in abruptio placentae was found to be 7%. Early diagnosis and immediate treatment of abruptio placentae are important factors for successful therapy of DIC. Fetal mortality was directly proportional to amount of blood loss, initial level of maternal hemoglobin and gestational age. No maternal death occurred.
KEY WORDS:
Abruptio placentae, Ante partum hemorrhage, Disseminated intravascular coagulation.Pak J Med Sci July - September 2009 Vol. 25 No. 4 660-664
How to cite this article:
Khooharo Y, Memon FA, Noorani KJ. Disseminated intravascular coagulation in Abruptio Placentae. Pak J Med Sci 2009;25(4):660-664.
1. Dr. Yasmeen Khooharo, FCPS
Assistant Professor,
2. Dr. Fayaz Ahmed Memon, FCPS
Assistant Professor,
Department of Medicine,
1-2: Muhammad Medical College,
Mirpurkhas,
Sindh - Pakistan.
3. Prof. Khursheed Jhan Noorani, FCPS
Dean College of Physician and Surgeons Pakistan
Department of Obstetrics and Gynecology
Correspondence
Dr. Yasmeen Khooharo,
Assistant Professor,
Muhammad Medical College,
Mirpurkhas - Pakistan.
Email: ykhooharo@yahoo.com
* Received for Publication: January 19, 2009
* Revision Received: February 3, 2009
* Revision Accepted: June 5, 2009
INTRODUCTION
Pregnancy is accompanied by changes in the haemostatic system, which converts it into hypercoagulable status from venous thromboembolism to disseminated intravascular coagulation.
1,2 DIC is always a secondary phenomena triggered by specific conditions such as abruptio placentae, amniotic fluid embolism, retained dead fetus, abortion induced with hypertonic fluids and vascular endothelial injury in case of pre-eclampsia, and incompatible blood transfusion.3-5Abruptio placentae is most common cause of DIC. Altered coagulation factors revert back to normal within first few weeks of postpartum.
4 The primary and most important treatment of DIC involves correction of the underlying cause, that is termination of pregnancy.6 DIC occurs in approximately 10% of cases of abruptio placentae.7 Maternal mortality due to coagulopathy and hemorrhage is about 1% in developed countries,8 but in our developing countries, it is high due to wide spread pre-existing anemia, difficulties with transport and restricted medical staff.5 In Pakistan maternal mortality is about 2.5%.9 Fetal loss is much more common than maternal deaths, approximately 15% worldwide.4,5 Over 50% of the perinatal deaths are still births, perinatal mortality is more common in developing countries.6METHODOLOGY
This study was conducted over a period of two years from 1st January, 2001 to 31st December, 2002 at JPMC. The study aimed to find out the proportion of DIC amongst the cases of abruptio placentae, to describe their management and foetomaternal outcome. Hence all the patients presenting with diagnosis of abruptio placentae on clinical findings and ultrasound were included in the study. Total number of patients included in the study with diagnosis of abruptio placentae was 100. These patients presented to emergency department of ward-8, Unit-I or Main casualty of JPMC, Karachi. The Resident Medical Officer (RMO) on duty took detailed history, carried out general physical, systemic, abdominal but not vaginal examination to see the bishop’s score until placenta praevia was ruled out by ultrasound. All the laboratory investigations such as complete blood picture, serum fibrinogen, fibrin degradation products, platelets, prothrombin time, activated partial thromboplastin time and clotting time was carried out. Based on the following criteria, the patients were labeled as cases of DIC.
1. No clot formation.
2. Serum fibrinogen <100mg/dl (normal 250 – 400mg/dl).
3. Fibrin degradation products >10µg/ml (D-dimmer)
4. Platelet count <50,000/cum.m
5. Prothrombin time 3 digit above control (control: 15sec).
6. Activated partial thromboplasin time (APTT).
7. Bleeding time.
8. Clotting time
3Elevated levels of D-dimmer and soluble fibrin are very sensitive for the diagnosis of DIC.
10 Patients in the labor room were managed according to the management protocol for abrubptio placentae as well as DIC. If there is no progress of labor, or delayed progress, fetal distress, or any other obstetrical indication then patients should be delivered by caesarean section. Performa was used for data collection. All the data analysis as well as development of database was done on SPSS version 10.0. Descriptive statistics was used to analyze the data, however, no statistical test was applied for conclusion since the study was descriptive non-interventional.RESULTS
This study is based upon 100 diagnosed patients of abruptio placentae and to assess the proportion of DIC and outcome of such patients. Majority of the patients with DIC had the age range from 26 to 35 years with the mean age of 27.5 years. All the patients were non-booked; however, they were referred and grandmultiparus ranged between Para 5 to 11. Majority of the patients were found in gestational age of 28 to 33 weeks. The mean gestational age was 33.14 weeks.

All the seven patients had severe vaginal bleeding; 4 (57.1%) had bleeding from the mouth, nose and intra-venous line. Abdominal pain was found in 6 (85.7%) cases. All the patients were found anemic and raised pulse rate and low blood pressure were observed. Fetal heart sound was audible in only one (14.3%) patient. Uterine tenderness was observed in all the patients with DIC and uterine contraction was observed in 4 (57.1%) patients.

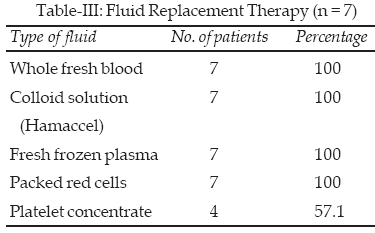
The diagnosis of DIC was based on clinical features and laboratory data (Table-I). Two patient (28.6%) were diagnosed only on laboratory evidence and 5 (71.4%) were diagnosed on clinical features and laboratory data as well (Table-II). All seven cases had low hemoglobin (<11gm/dl) with the average of 4.41gm/dl. Raised fibrin degradation products, clotting, prothrombin, activated partial thromboplastin time and decreased serum fibrinogen and platelets were distinguished laboratory reports. All the seven patients were managed with fluid replacement therapy. Whole fresh blood, colloid solution, fresh frozen plasma, packed red cells was given to all seven patients and four patients received platelet concentrate (Table-III).
Six (85.7%) patients with DIC were delivered by spontaneous vaginal delivery while only one (14.3%) was delivered by cesarean section. Majority of the patients had induction delivery time interval between 0-4 hours with average time of 0-6 hours. A high fetal mortality rate of 85.7% was observed in the patients with DIC and all were fresh still birth and one alive baby was delivered by cesarean section with poor apgar score was admitted in nursery and discharged healthy after treatment. However no maternal mortality was observed in the patients of DIC.
DISCUSSION
Maxon JH (2000) reported that no single laboratory test is available for diagnosis of DIC.
11 However; several certain clinical findings along with laboratory investigations have supported the diagnosis. We also made diagnosis of DIC on the basis of clinical as well as laboratory results.This study estimated that DIC was found in 7% of the cases which is about 3 times higher than the proportion of DIC (2.5%) reported by Ellahi and Khalid at Nishtar Hospital Multan.
12 Sardar M, found that in most severe forms patients presented with bleeding from skin, mucus membrane, incisions, intravenous line and catheter sites as well as massive obstetric haemorrhage.13 These findings were also observed in our study. Four patients (51.1%) had bleeding from mouth, nose, and intravenous line. All patients were anemic with raised pulse, six (85.7%) patients had low and one (14.3%) patient had high blood pressure. Fetal heart sounds were present only in one patient, uterine tenderness was observed in all the patients with DIC and uterine contraction was observed in four (57.1%) patients. All seven DIC patients were observed with the raised fibrin degradation products, prothrombin and activated partial thromboplastin time while low serum fibrinogen, blood platelets, and hemoglobin. Two (28.6%) cases were diagnosed only on laboratory evidence and 5 (71.4%) were diagnosed on clinical as well.Following the immediate management with fluid replacement therapy, delivery of fetus, and placenta as suggested by AL-Nuaim LA, et al.,
14 and Letsky EA,1 significant improvement in all patients was observed. Induction delivery time in majority of patients was attributed to be rapid (0- 4 hours). This is similar to the research findings as reported by Douglas, Buchman, and MacDonald (1955).9Six (85.7%) of cases delivered by spontaneous vaginal delivery were still births. This high perinatal mortality was due to asphyxia and prematurity. Almost the similar finding were recorded in a study by Hellmann and Pritchard on the basis of quite a large sample size of 530 women.
15 The remaining one case (14.3%) was delivered by caesarean section due to fetal distress, this patient developed DIC after caesarean section due to post-partum hemorrhage.Five (71.4%) cases were augmented with syntocinon infusion and amniotomy. One (14.3%) case was delivered without any intervention. A high fetal mortality rate of (85.7%) was observed in our study, all were fresh still birth and one alive baby was delivered by caesarean section with poor Apgar score. This baby was admitted in nursery of our department, it recovered and survived.
In our study however no maternal mortality was observed with DIC. All seven (100%) cases were monitored in the intensive care unit within the department. Patient were closely monitored for post-partum hemorrhage, which is more common due to atoniy of uterus and hemophilic nature of disease.
16 But after the delivery of the fetus and placenta the spontaneous correction of (DIC) was seen.7CONCLUSIONS
DIC is a serious life threatening complication of abruptio placentae for both mother and fetus. Perinatal mortality is still alarmingly high due to asphyxia and prematurity. Following are the major findings of the study:
Early diagnosis and immediate treatment of abruptio placentae are important for successful therapy of DIC. Late arrival, diagnosis, and treatment increase likelihood of morbidity of mother and baby. Early referral and good laboratory facilities improve the maternal morbidity and mortality. Fetal mortality is directly proportional to the level of hemoglobin of the mother, amount of blood loss and prematurity rather than DIC.
The pre-disposing factors to ward off the problem in abruptio placentae, is poverty, ignorance and lack of education among the population. Blood bank services should be made widely available to provide faster service and rapid availability of fresh whole blood, fresh frozen plasma, packed red cell and platelet concentrates. These should be made available even at district and Rural Health Centers. Compulsory training sessions for capacity building of new doctors, nurses may be initiated to follow the common protocols for the management of abruptio placentae so as to reduce the risk of complications such as DIC.
REFERENCES
1. Letsky EA. Disseminated intravascular coagulation. Best Pract Res Clin Obst Gynaecol 2001;15:623-44.
2. Kenneth G, Perry Jr. Abruptio placenta. In: Michel E, Rivilin, Rick W, Martin. Manual of clinical problems in obstetrics and gynecology 5th ed. Lippincott: Fest washing Square: Philadelphia: Williams and Wilkins 1999;21-5.
3. Soomro N, Sanaullah F. Obstetrician’s encounter with disseminated intravascular coagulation (DIC). Med Channel 1998;4:23-7.
4. Cotron RS, Kumar V, Collins T, Robbins SL. Disseminated intravascular coagulation. In: Cotran RS, Kumar V, Collins T, Robbins SL. Pathologic basis of disease 6th ed. WB Saunders: Pennsylvanis 1999;640-3.
5. Osterud B, Bjorklid E. The tissue factor pathway in disseminated intravascular coagulation. Semins Thromb Hemostat 2001;27:605-17.
6. Pritchard JA, Brekken AL. Clinical and laboratory studies on severe abruptio placentae. Am J Obstetric Gynecology 1967;97:681-700.
7. Justin C, Taylor DJ. Bleeding in late pregnancy. In: James DK, Steer PJ, Weiner CP, Gonik B. High risk pregnancy 2nd ed. Philadelphia: WB Saunders 1999;111-28.
8. Department of health (1996) report on confidential enquiries into maternal deaths in the United Kingdom 1991 – 1993 London, HMSO.
9. Douglas RG, Buchman MI, MacDonald FA. Premature separation of the normally implanted placenta. J Obstetric Gynecol Br Emp 1955;62:710-22.
10. Horan JT, Froncis CW. Fibrin degradation products, fibrin monomer and soluble fibrin in disseminated intravascular coagulation. Semin Thromb Hemost 2001;27:57-66.
11. Maxon JH. Management of disseminated intravascular coagulation. Crit Care Nurs Clin North Am 2000;12:341-52.
12. Ellahi N, Khalid T. Abruptio placentae; maternal and fetal outcome. The Professional 2001;8:296-300.
13. Sardar M, Zafar A, Samme A. Disseminated intravascular coagulation in obstetrics. Pak J Obstetric Gynecology 1997;10:13-15.
14. AL-Nuaim LA, Mustafa MS, Abdel Gader AG. Disseminated intravascular coagulation and massive obstetric hemorrhage. Management dilemma. Saudi Med J 2002;23:658-62.
15. Hellman LM, Pritchard JA. Placenta previa and abruptio placentae. In: Hehnan LM, Pritchard JA editors. Williams Obstetrics 14th ed. New York: Appleton Century – Crofts 1971;612.
16. Joseph B. DeLee. Abruptio placenta the principles and practice of Obstetrics 17th ed Philadelphia: WB Saunders 1939;499-511.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@