|
||||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||||
|
ISSN 1681-715X |
||||||
|
||||||
|
- |
||||||
|
ORIGINAL ARTICLE |
||||||
|
- |
||||||
|
Volume 22 |
October - December 2006 |
Number 4 |
||||
|
|
||||||
|
||||||
|
||||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||||
|
ISSN 1681-715X |
||||||
|
||||||
|
- |
||||||
|
ORIGINAL ARTICLE |
||||||
|
- |
||||||
|
Volume 22 |
October - December 2006 |
Number 4 |
||||
|
|
||||||
|
||||||
Carpal Tunnel Release via Mini-Open Wrist Crease Incision:
Procedure and Results of Four Years Clinical Experience
Sudqi A. Hamed1, Falah Z. Harfoushi2
ABSTRACT
Objective: To evaluate prospectively the safety and effectiveness of a mini-open technique for carpal tunnel release using a 1- 1.5 centimeter wrist skin crease incision.
Methods: Clinical experience with the technique consists of 98 patients and 124 hands over a period of four years, from October 1999 - October 2003. All cases were done as out patient and under local anesthesia. Details of the technique, patient satisfaction and outcomes are presented.
Results: The mean duration of the operation was 12 minutes. The technique was highly satisfactory cosmetically for all patients especially who previously experienced the open standard palmar incision in the other hand. Ninety-four percent of the patients were completely satisfied with the procedure regarding their symptoms. Five cases developed minor superficial wound infection. No major nerve or vascular injury had occurred. Postoperative outcome measures and patient satisfactions (pain, return to normal activities and work, scar and pillar tenderness) were comparable with published series of endoscopic carpal tunnel release.
Conclusion: This technique is simple, safe, cosmetically satisfactory and cost effective. It can be used by experienced hand surgeons especially in countries where endoscopic release is expensive and not widely available.
KEY WORDS: Carpal tunnel surgery, Mini-open release, Safety, Complications, Satisfaction.
Pak J Med Sci October - December 2006 Vol. 22 No. 4 367-372
1. Sudqi A. Hamed, MD
2. Falah Z. Harfoushi, MD
1-2: J.B.G.S (Jordanian
Board in General Surgery),
J.B.O.S (Jordanian Board in Orthopedic Surgery),
Royal Rehabilitation Centre,
King Hussein Medical Centre,
Amman – Jordan.
Correspondence:
Dr. Sudqi A. Hamed,
P.O. Box: 10082, Code: 13181,
Zarqa – Jordan.
E-Mail:
sudqi_hamed2005@yahoo.com
* Received for Publication: April 29, 2006
* Accepted: June 30, 2006
INTRODUCTION
Since the first carpal tunnel release (CTR) for median nerve compression at the wrist was performed by Learmonth
1 in 1930, the operation has undergone many changes. Today, traditional open carpal tunnel release (OCTR) is the gold standard for the surgical treatment of carpal tunnel syndrome. It provides direct vision of the ligament, guarantees complete section and allows treatment of additional pathologies in the carpal tunnel.2,3 Its main drawbacks are tender scar, pillar pain, long healing period, flexor tendon bowstringing, adherence of tendons, reflex sympathetic dystrophy and cosmetic complaints, all related to the incision.4,5In an effort to decrease these complications, endoscopic carpal tunnel release (ECTR) was developed in 1989 to leave the skin intact over the flexor retinaculum.
6,7 According to these studies, ECTR results in a notably more rapid return to work and daily activities, less scar tenderness, less pillar pain and better cosmesis. The disadvantages of ECTR includes: costly equipment required, which renders a simple procedure cumbersome; costly surgery; prolonged operative setup time. Also, there is a steep learning curve for this technically demanding procedure, and practice in cadavers has been recommended for surgeons before clinical use.8 Most importantly, there have been many reported complications in association with the procedure, including neuropraxia, transection of the median nerve or its branches, ulnar nerve injury, superficial palmar arch injury.3,9,11,12 In addition, incomplete division of the transverse carpal ligament has been noted in cadaveric studies and clinical series.3,7-12Since 1991, various authors tried to combine the simplicity and safety of OCTR with the reduced tissue trauma and postoperative morbidity of ECTR by using a short incision open techniques (wrist crease mini-open incision,
13-17 short longitudinal incision in the palm18-21 double incision mini-opentechnique.22 With these approaches, the flexor retinaculum is divided with a conventional knife, scissors or specially developed instruments.In this study, we report our results and experience with a wrist crease mini-open incision (WCM-OI) using conventional scissors for carpal tunnel release.
PATIENTS AND METHODS
Surgical technique: In this study we performed all the operations through a transverse incision at the distal crease of the wrist & following the same steps as described by many authors.
13-17 All the procedures were performed by the same surgeon (S.H.) in an outpatient setting under local infiltration anesthesia without using a tourniquet. The wrist was placed in moderate extension over a rolled towel. A short transverse incision, about 1-1.5cm in length, was performed at the distal crease of the wrist ulnar to the palmaris longus tendon (PL) Fig-1.
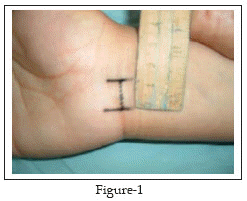
The PL is isolated and retracted radially Fig-2. The antebrachial fascia lying deep to PL is exposed where it is continuous with the proximal edge of the transverse carpal ligament distally. The anatomic plane between PL and palmar fascia superficially and the antebrachial fascia and the carpal ligament deeply is opened with blunt dissection, using a pea nut gauze. A 5mm transverse incision is made with a scalpel on the proximal edge of the carpal ligament, taking care not to damage the median nerve, thus allowing access to the carpal canal. A blunt Freer elevator or the closed scissors is inserted under the ligament and advanced proximally to establish an extrabursal path where the proximal part of the carpal ligament and the distal portion of the antebrachial fascia are then incised with the blunt scissors under direct vision Fig-3. Now the proximal edge of the carpal ligament is seen end on Fig-4; thus one is able to visualize superficial and immediately deep to the carpal ligament. The blunt Freer elevator or the scissors is inserted under the ligament and advanced distally to establish an extrabursal path. The proximal edge of the transverse carpal ligament is divided under direct vision. And by retracting the palmar skin and fascia volarly, thus providing improved visibility of the distal portion of the carpal ligament, the distal part is transected with a blunt and straight conventional scissors. The transection proceeds snip by snip and carefully with the scissors directed in the longitudinal axis of the fourth ray. Upon completing the release, a snap is felt.
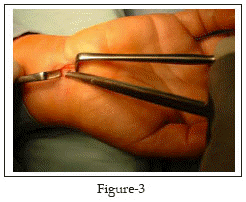
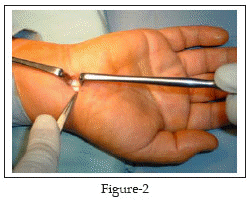
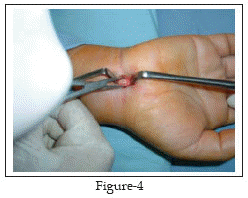
Finally, we check the completeness of the release by introducing the tip of the closed straight scissors or the blunt Freer elevator distally, beyond the distal edge of the retinaculum, and withdrawing it slowly while the tip is directed volarly. If the release is incomplete, the surgeon will feel a step; otherwise, withdrawal should be smooth. At this stage, the median nerve will be seen clearly through out the tunnel Fig-5.
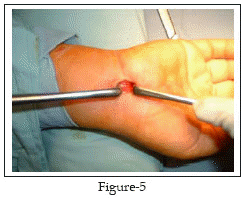
At the end, the skin incision is closed with monofilament non-absorbable sutures Fig-6 and dressed. The patient is advised to start gentle active finger movement immediately, to keep the hand elevated for the first 24 hours, to take some pain killer for the next 48 hours and to come back after ten days to check the wound and to remove stitches.
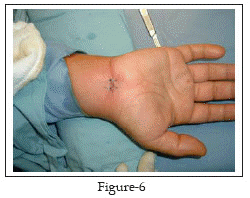
From October 1999 to October 2003 we performed 124 carpal tunnel releases on 98 patients, using the WCM-OI. The diagnosis of carpal tunnel syndrome was clinical and then it was confirmed by electrodiagnostic studies, which were performed on all patients. Only patients with idiopathic carpal tunnel syndrome were included in the study, while patients with secondary causes were excluded and treated by OCTR. All patients had failed prior conservative treatment for at least four weeks before the procedure. Demographic data of our patients are shown in Table-I.

Surgical results and outcomes were evaluated by using the Boston Carpal Tunnel questionnaire (BCT), which is a patient – oriented, self- administered, standardized instrument that has shown reproducibility and validity.23,24 It consists of two scales. The symptom severity scale includes 11 items concerning severity, frequency and duration of symptoms. The functional status scale includes 8 items concerning difficulties in performing 8 daily activities. The symptom severity and functional status scores are the mean scores of all items in each scale ranging from 1 (no) to 5 (most sever) symptom or disability. The patients were asked to report the time when she or he could do the activities of daily living (washing, eating, writing, etc.) with the operated hand. During follow- up period scar tenderness, radial and ulnar pillar tenderness were assessed according to the method used by Lee et al.21 where the patients rated the tenderness at their incision, radial pillar and ulnar pillar on a scale of 1 (no tenderness) to 4 (sever tenderness). Any complications were recorded. At the last clinic appointment patients were asked to grade their cosmetic results as poor, fair, good or excellent; and we assessed the over all patient satisfaction by asking the patients to select a number on a scale graded from 0-100.
RESULTS
The mean duration of the operation was 12 minutes (9-16 minutes). No single major complication, wound or neurovascular, was recorded in any of the patients. Minor complications were observed including: four superficial wound infections cured over five days of oral antibiotics and dressing; two wound hematomas resolved over the next month without sequel; subjective numbness in long finger, resolved over three months, in one patient; parasthesia in ulnar nerve distribution in one patient, resolved over three months; mild reflex sympathetic dystrophy developed in one hand managed conservatively over three months.The preoperative and postoperative scores for the symptom severity and functional status scales of the Boston Carpal Tunnel questionnaire are shown in Table-II. Both scales showed large improvement from before surgery compared with 3 weeks, 6 weeks and 12 weeks after surgery. The median time to activities of daily living was 6 days. Scar and pillar tenderness were assessed at six weeks and twelve weeks postoperatively and are shown in Table-III.
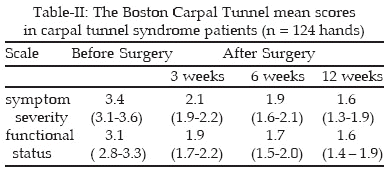
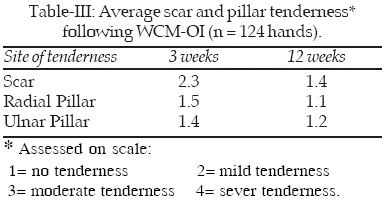
After a mean of 4.2 months follow-up evaluation, all patients were satisfied with their cosmetic results (96 % reported good- excellent results). The average subjective over all satisfaction with the procedure, assessed by asking each patient to select a mark on a scale graded from zero to hundred, was 92%.
DISCUSSION
As the optimal modality for carpal tunnel release has been debated in recent years, various open techniques using small incisions have been described.
13-22 In 1991, Carter 13 published the first surgical experience in treating carpal tunnel syndrome using a transverse wrist incision and a special carpal tunnel knife. He reported no complications in 100 cases with patient over all satisfaction of 94%.In 1994, Bromley
19 used a short single palmar incision, and Wilson22 used double palmar incisions for carpal tunnel release and they cut the flexor retinaculum with a conventional scissors. They reported excellent results without any major complications.In 1995, Abouzahr et al.
17 released the flexor retinaculum in cadavers with a transverse wrist incision and injured the superficial palmar arch in one of 28 hands. He concluded that the technique is simple, effective, employs inexpensive instruments, and has a low complication rate.Hallock et al.
18 did a prospective comparison of 71 hands which underwent open release using a minimal incision with 66 hands who had ECTR. They found no statistical differences between the two techniques regarding scar length, rate of complications, and length of time before resuming routine activities. Lee et al16 performed CTR for 275 hands through WCM-OI, using a special knife. They had no operative complications and they found the procedure simple and of low cost.In 1998, Lee and Stickland
21 published their experience of CTR via a limited palmar incision in two centers. They did anatomic dissection in 28 cadaveric specimens following the procedure and found complete decompression of the carpal tunnel, preservation of the palmar cutaneous branch and thenar motor branch of the median nerve, ulnar artery and nerve and superficial palmar arch. Their clinical experience with the technique on 694 hands showed that 92.2% of patients derived complete or near complete symptomatic relief with two complications (0.29%). They found that scar and pillar tenderness, grip, and key pinch are comparable with those in published series of ECTR.Our results show that large improvement in symptoms and function occurred in the first three weeks after surgery, and further improvement continued up to three months postoperatively Table-II. These improvements are comparable with those after OCTR
27,28 and after ECTR.6,7The Average operating time in our series was 12 minutes (range 9-16 minutes). It is almost similar to the operating times reported by other authors used the same small incision technique
16,21. This is significant when compared with the data from Brown et al.9 who did a prospective, randomized assessment study of OCTR and ECTR and found that the operating room was fifty-seven minutes for the OCTR and sixty-seven minutes for the ECTR. Hallock et al.18 in a prospective comparative study, found that the actual surgery time for the minimally invasive open method was 11.7+3.0 minutes and 21.6+5.9 minutes when using the endoscope. However, recently Chow29 presented his thirteen years experience with ECTR on 2402 hands and reported an average operating time of 8 minutes. He explained it on the basis of his long experience.The reduced postoperative scar and pillar pain and tenderness were considered the primary advantages of ECTR when compared with the OCTR.
7,9,10,12 The results in our patients Table-III, were remarkably similar to those of Lee et al.21 Following limited open incision, and those obtained after ECTR.7,9,10,12 Decrease scar pillar pain and tenderness following endoscopic and mini-open incisions can be explained by the reduced trauma to the skin, subcutaneous tissue, palmar aponeurosis and by preserving the fascial convergence between thenar and hypothenar musculatures.21 On the contrary, the OCTR divides all these structures to obtain access to the transverse carpal ligament. The absence or mild scar and pillar pain and tenderness facilitate the earlier return to daily activities as seen in our patients.It is apparent from recent reports that complications following CTR are unfortunately more than what reported in the literature.
5,12 In 1995, Palmer12 made a survey among members of the American Society for Surgery of the Hand to assess and compare major surgically treated complications of ECTR and OCTR over a five year period. The survey revealed treatment of 283 complications following OCTR, including laceration of median nerve, palmar cutaneous branch, digital nerve, superficial palmar arch and tendon laceration. The survey also revealed 455 complications following ECTR. Although the author did not report the incidence of these complications, we can guess that the incidence is low for the OCTR as a common procedure but is high for the non-popular ECTR. Chow25 believed that the major reason for this high complication rate is the lack of experience, as the learning curve for the ECTR is long.Reviewing the results of authors who used the mini- open, semi-blind approaches revealed major complication rates of 0% - 0.3%.
13-22 Our series showed similar results. The way to have a safe semi-blind open procedure that we used in the present study is to push the scissors gently towards the longitudinal axis of the fourth ray while the tip of the scissors directed volarly and to stop immediately when the ligament resistance suddenly decreases. The incision is also ulnar to the tendon of palmaris longus, which avoids the palmar cutaneous branch of the median nerve. These mini-open approaches are easy to master and have a short learning curve, which contribute to their low morbidity and post-operative complications.Postoperative cosmetic appearance of the palm is an important issue related to skin incision. Our results showed clearly that the WCM-OI we used is highly satisfactory and comparable to endoscopic approach. The over all patient satisfaction with the procedure was also excellent at the final follow-up visit. We believe that a longer follow-up period is needed to assess the long term results of this approach regarding the possibility of recurrence of the disease, which was not done in our study or in the previous studies which used these mini- open approaches.
In conclusion, based on our study and on the results of previous studies, the mini-open technique is simple, easy to master, safe and cost effective. The outcomes which are comparable to ECTR and superior, in certain aspects, to OCTR justify its use by experienced hand surgeons especially in countries where endoscopic release is expensive and not widely available.
REFERENCES
1. Learmonth JR. The principle of decompression in the treatment of certain diseases of peripheral nerves. Surg Clin North Am 1933; 13: 905.
2. Szabo RM. Entrapment and compression neuropathies. In: Green DP (Ed.). Greens Operative Hand Surgery 1999; 2: 1404-7.
3. Akelman E, Weiss AC. Carpal tunnel syndrome: Etiology and endoscopic treatment. Orthop Clin North Am 1995; 26 (4): 769-78.
4. Semple JC, Cargill AO. Carpal tunnel syndrome: Results of surgical decompression. Lancet 1969; 3: 918-9.
5. MacDonald RI, Lichtman JJ, Hanlon JN. Complications of surgical release for carpal tunnel syndrome. J Hand Surg 1978; 3: 70–6.
6. Okutsu I, Ninomiya S, Takatori Y. Endoscopic management of carpal tunnel syndrome. Arthroscopy 1989; 5: 11-8.
7. AgeeJM, McCarroll HR, Tortosa RD. Endoscopic release of the carpal tunnel: A randomized prospective multicentre study. J Hand Surg 1992; 17A: 987-95.
8. Rowland EB, Kleinert JM, Endoscopic carpal-tunnel release in cadavera: An investigation of the results of twelve surgeons with this training model. J Bone Joint Surg 1994; 76A: 266–8.
9. Brown RA, Gelberman RH, Seiler JG. Carpal tunnel release: A prospective, randomized assessment of open and endoscopic methods. J Bone Joint Surg 1993; 75A: 1265–75.
10. AgeeJM, Peimer CA, Pyrek JD. Endoscopic carpal tunnel release: a prospective study of complications and surgical experience. J Hand Surg 1995; 20A: 165-71.
11. Varitimidis SE, Herndon JH, Sotereanos DG. Failed endoscopic carpal tunnel release: operative findings and results of open revision surgery. J Hand Surg 1999; 24B: 465- 7.
12. Palmer AK,Toivonen DA. Complications of endoscopic and open carpal tunnel release. J Hand Surg 1999; 24A : pp. 561–5.
13. Carter SL. A new instrument a carpal tunnel knife. J Hand Surg 1991; 16A: 178–9.
14. Klein RD, Kotsis SV, Chung KC. Open carpal tunnel release using a 1-centimeter incision technique and outcomes for 104 patients. Plast Reconstr Surg 2003; 111:1616-22.
15. Cellocco P, Rossia C, Bizzarria F. Mini-Open Blind Procedure Versus Limited Open Technique for Carpal Tunnel Release: A30-Month Follow-Up Study. J Hand Surg 2005; 30A:493-9.
16. Lee H, Jackson TA. Carpal tunnel release through a limited skin incision under direct visiualization using a new instrument, the carposcope. Plast Reconstr Surg 1996; 98: 313-9.
17. Abouzahr MK, Patsis MC, Chiu DT. Carpal tunnel release using limited direct vision. Plast Reconstr Surg 1995; 95: 534–8.
18. Hallock GG, Lutz DA. Prospective comparison of minimal incision "open" and two-portal endoscopic carpal tunnel release. Plast Reconstr Surg 1995; 941-6.
19. Bromley GS. Minimal-incision open carpal tunnel decompression.J Hand Surg 1994; 19A: 119–20.
20. Serra JM, Benito JR, MonnerJ. Carpal tunnel release with short incision. Plast Reconstr Surg 1997; 99: 129–35.
21. Lee WB, Strickland JW. Safe carpal tunnel release via a limited palmar incision. Plast Reconstr Surg 1998; 101: 418–24.
22. Wilson KM. Double incision open technique for carpal tunnel release: an alternative to open release. J Hand Surg 1994; 19A: 907-12.
23. Levine DW, Simmons BP, Koris MJ et al. A self-administered questionnaire for the assessment of severity of symptoms & functional status in carpal tunnel syndrome. J Bone Joint Surg 1993; 75A: 1585–92.
24. Atroshi I, Gummesson C, Johnsson R. Symptoms, disability and quality of life in patients with carpal tunnel syndrome. J Hand Surg 1999; 24A: 398-404.
25. Chow JC, Hantes ME, IL MV. Endoscopic carpal tunnel release: thirteen years experience with the Chow technique. J Hand Surg 2002; 27A: 1011-18.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk