|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
Intracervical PGE2 gel for cervical
ripening and induction of Labour
Fazia Raza1, Saeeda Majeed2
ABSTRACT
Objective: The objectives of the study were to evaluate the efficacy of interacervical gel as a cervical ripening agent in the unfavourable cervix. The changes in the Bishops score, onset of labour and its progress were secondary outcome measures.
Methodology: Fifty patients were enrolled in this prospective study conducted in Gynae "A" unit of Khyber Teaching Hospital, Peshawar from January to December 2004. Patients with singleton living fetus, cephalic presentation, gestational age of >36 weeks completed were included. Half milligram (0.5mg) of prostaglandin E2 gel intracervical was used for intracervical application. The application was repeated after 6-12 hours if the Bishop score remained unfavourable i-e <5.
Results: The indications were postdates pregnancy (50%), PIH (18%), Diabetes Mellitus (18%) and Rh isoimmnization (6%). The success rate in terms of vaginal delivery was 82%. The lower segment caesarean section rate was 18%. The commonest indication for caesarean section was failure to progress. The complications side effects were minimal & the neonatal outcome was good.
Conclusion: This study showed that intracervical application of prostaglandin E2 gel is effective, safe acceptable method for ripening of cervix in women with unfavourable cervix.
KEY WORDS: Intracervical prostaglandin E2, unfavorable cervix, Bishop score, induction of labour.
Pak J Med Sci April - June 2008 (Part-I) Vol. 24 No. 2 241-245
1. Fazia Raza,
Gynocologist,
Ploy Clinic Hospital ESSI Kohat Road,
Peshawar - Pakistan.
2. Saeeda Majeed,
Incharge Gynae Department,
Rehman Medical Institute,
Hayatabad, Peshawar - Pakistan.
Correspondence:
Fazia Raza,
E-mail: faziaraza@yahoo.com
* Received for Publication: September 20, 2007
* Revision Received: January 23, 2008
* Revision Accepted: January 27, 2008
INTRODUCTION
The rate of inducing labour varies widely in different institutions depending on choices of obstetricians and indication for Induction,
1 post dates pregnancy being a common indication, including social reasons.2 The process of induction of labor should only be considered when vaginal delivery is felt to be the appropriate route of delivery. Induction of labour is a challenge to the clinician, mother and the fetus and must be selected and supervised carefully.1At term a series of several complex events are modulated by neuroendocrine pathways, humoral transmission, steroids and local hormones. During the transition to the onset of labor the cervix becomes soft, short and cervical resistance decreases. This process is called as "cervical ripening".
3-5 Cervical ripening is an essential prerequisite for induction and is employed when the cervix is unfavorable before initiation of uterine activity. The degree of cervical ripening or favorability is assessed with Bishops scoring system, which has now being modified (Table-I). It provides the basis for cervical assessment for induction of labor. A favorable cervix is with a modified Bishop score of more than 8 and unfavorable cervix with a Bishop score of <4.2When the cervix is unfavorable the principle method of induction of labour is with the help of prostaglandins which are available in the form of intercervical, vaginal gel and tablets and oral tablets and injections.
1Prostaglandins E
2 intracervical gel contains 0.5mg of dinoprostone & when applied locally it induces collagen breakdown, dispersion and fluid absorption by stromal tissue and effective cervical ripening for induction of labour.6,7 In some cases early uterine activity may start as well.A number of reports have appeared in the international literature favoring the intracervical route, claiming advantage of increased incidence of successful initial inductions, fewer side effects, simple administration and minimal discomfort to the patients. Some studies have been conducted in Pakistan but they have not yet been published.
METHODOLOGY
A prospective study of one year duration from January to December 2004 was carried out in Gynae "A", Khyber Teaching Hospital, Peshawar in which 50 patients were included. Patients with gestational age>36 weeks, singleton living fetus with cephalic presentation, specific indication for induction, Bishop score 1-4 intact membranes, reactive cardiotocography were included. Patients with previous uterine scar, cephlopelvic disproportion, Grandmultiparity, intrauterine fetal death, antipartum hemorrhage, Asthma, Gross oligohydramnios were excluded. Patients who fulfilled the inclusion criteria, were admitted & evaluated for maternal and fetal well being.
A non-stress test was carried out. The patients with reactive non stress test were included in the study. Written informed consent was taken and Bishop score was noted down. In patients where the date of last menstrual period was not known the gestational age was estimated by an early or late ultrasound.
Using sterile technique a prefilled syringe containing 0.5mg of dinoprostone was instilled endocervically. Following the administration the patient remained in the supine position for at least 15-30 minutes to minimize leakage from the cervical canal.
The Bishop score was recorded initially and after six hours. The cervix was graded as a favorable cervix when the Bishop score was equal to or greater than five points. These patients either went into spontaneous labour or the labour was augmented by oxytocin infusion after 6-12 hours of last dose of prepidil.
If the Bishop score remained less than 5 after 6-12 hours, reapplication was done. A minimum of two doses were used. When the score remained below 5 after 6 hours of second application it was taken as failure. All the patients were monitored clinically under close supervision. The patients vital parameters, fetal heart sound and uterine contractions were recorded every half an hour. The Bishop score was recoded at intervals. Progress of labour was charted on a partogram.
Data collection was done with the help of proforma and it was analyzed with computer based software SPSS 10.0 version.
The different statistical tests used for data analysis were percentage, proportion mean and standard deviation. The difference between different variables was analyzed using Chi-square test and T-test where appropriate. The main outcome measures were:
i. Changes in Bishop score
ii. Route of delivery
iii. Application delivery internal
Gestational age in primigravida patients was 30-38 weeks in (20%), 38-40 weeks in 32 % and 40-42 weeks (48%). Gestational age in multigravida was 36-38 weeks in (10%) 38-40 weeks in 38% and 40-42 weeks in 52%.
RESULTS
Dinoprostone or PGE2 gel was applied endocervically in 50 patients and Results were analyzed on age, parity, indications for induction, success rate of induction, outcome of induction and maternal and fetal complications. Out of 50 patients 31 were primigravida and 19 were multigravida. The mean age in PG was 26 years and in MG was 27 years 38% of primigravida were in the age group of 20-25 years and 42.10% of multigravida were in the age group of 26-30 years. 48.38% of the primary gravida and 52.63% of multigravidas presented between the gestational age group of 40 to 42 weeks.

The commonest indications for induction of labour were postdated pregnancy (50%) followed by PIH (18%) and Diabetes (18%). The other indications were IUGR, Rh-Incompatibility and BOH. (Table-II)
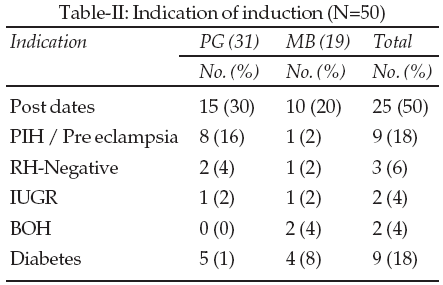
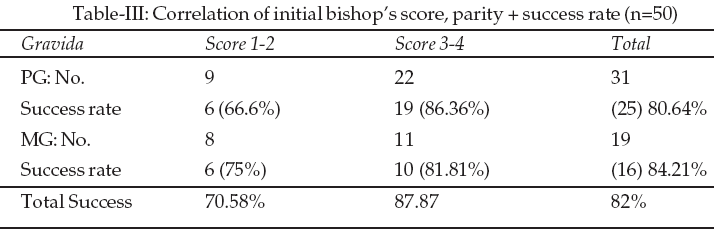
The initial Bishops score (Table-III) at the time of PGE2 gel introduction had a significant influence on the success of induction. The success rate was 70.58% when the score was low (1 or 2) and as high as 87.87% when the score was three or four. The overall success rate in the study was 82%.
The mean Bishops score was 2.6, which increased to 5.5 after 6 hrs and to 9.5 after 12 hrs, it means a gradual but progressive change in Bishop’s score occurred in successful cases. Reapplication was required in 7 cases. Amongst the subjects requiring reapplication, the rate of progress was slower. The failure rate was high in those requiring reapplication. Vaginal delivery occurred in 82% cases out of which three cases (6%) had forcep’s delivery and two had vaccum delivery. The incidence of LSCS was 18%. The indications for caesarean section was failed inductions, fetal distress and nonprogress of labor. The commonest being failure to progress (8%). The incidence of failed inductions was 4%.
The induction delivery interval was shortened, 20 cases (48.5%) delivered within 12 hours out of which 6 were primigravida and 14 were Multigravida. The mean induction delivery interval was 14 hours and S.D 5.59. (Table-IV)
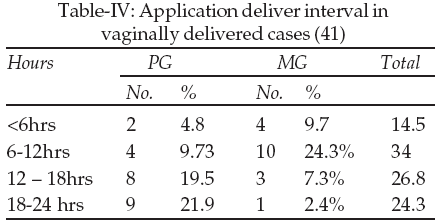
The commonest complication occurring after PGE2 installation was Diarrhea and vomiting in 10% of cases, fever in 4%, maternal hyper stimulation occurred in 4% of cases where as PPH occurred in 2% of cases. There were no life threatening complications.
There was no case of neonatal mortality. Mean birth weight was 2.7kg. The mean Apgar score was 8 at one minute and 9 at five minutes. Only two cases had Apgar score below 7 at 5 minutes. The incidence of neonatal jaundice and meconium aspiration was 10% and 2% respectively. Other fetal complications included birth asphyxia in two (4%) respiratory distress syndrome in one patient (2%). There was no case of septicemia.
DISCUSSION
Modern obstetrics aims at improving the safety of the mother and the fetus during antenatal period as well as parturition. The aim of induction of labour is to perform safe vaginal delivery. Spontaneous labour and vaginal delivery is preceded by a cascade of synchronized events, which leads to ripening of cervix.
1 Calder et al has reported that ripening of cervix governs the ease and success of induction of labour.5 Prince et al8 has oberved that if ripening of cervix fails to occur, then delivery and labour may be prolonged and many a times it may be unsuccessful. Induction of labour in a patient with an unripe cervix is professional folley without ripening the cervix first.From 15% to 20% of all pregnancies require induction of labour.
1 Cervical ripening before induction is essential and Prostaglandins (PGs) are thought to play a significant role in the process of cervical ripening and initiation of labor.2,3 Fetal membranes and decidua produce PGE2 during pregnancy and labor.1-4 Release of this hormone leads to changes in the biochemistry of the cervix and also stimulates the production of PGF2a. In turn, PGF2a sensitizes the myometrium to oxytocin.5 Exogenous administration of PGE2 (dinoprostone) is known to mimic this natural process and lead to cervical ripening or labor.3,4,6Endo cervical application of prostaglandin E2 gel has become increasingly popular following studies in Sweden. However PGE1 is also a suitable preparation for softening and effacement of cervix. The overall success rate in terms of vaginal delivery was 82% in our study. Kierse at al
9 in his meta analysis had shown that intracervical prostglandins E2 in the form of gel compared with no treatment effectively increase Bishop’s score and the incidences of successful initial inductions. In these trials the success rate was from 72%. The success rate of our study is comparable to study done by Rafiq-ul-Islam et al10 84% and Warke et al 81%.11 The incidence of failed induction in our study was 4% which is comparable to a study done by prince et al8 with incidence of 6% but in contrast to study done by Warke et al11 with a failure rate of 1.33%.Various studies have shown the beneficial effects of intra cervical PGE2 gel in improving Bishop score, the improvement ranging from 3 to 7 points.
7,8,12 The success of induction of labour was found to be directly proportional to the Bishop score at instillation. The mean Bishop’s score was 10.7 which is comparable to the study done by Noah et al7 1987. The overall mean induction delivery time was 16.43 hours. Various studies have shown considerable variation as far as induction delivery time is concerned ranging from 9 hours Noah et al7 to 17.9 hours, Thiery et al13 to 20.2 hrs in a study done by Jackson Gm 1994.14 The parity of the patients considered also influenced the duration of labour. PGE2 gel has shown to shorten the induction delivery interval in many studies and thus will result in less fetal and maternal morbidity and mortality.The commonest indication for induction of labor in this study was Postdates pregnancy (50%, PIH (18%), and Diabetes (18%), which was comparable with the study done by Turner JE.
15 In this study, post dates, PIH and rupture of membranes were the major indications accounting for 70% of inductions. It is also comparable with the results of Sayeeda Batool Mazhaar et al16, but in contrast to the study done by Michelle et al.17 in which the most common indication for induction was Oligohydramnios followed by postdates & PIH.Present data from worldwide prospective investigations strongly suggest that local PGE
2 therapy has few maternal side effects, and favorable neonatal outcomes. In our study the side effects were minimal and neonatal out come was good.CONCLUSIONS
*
The study showed that intracervical application of prostaglandin E2 is an effective, safe and acceptable method for induction of labour in women with unfavorable cervix and indications for induction.* Dinoprostone gel application resulted in improved Bishop score, facilitates the process of induction, increased number of successful inductions, shortened application delivery interval and decreased cesareans section rate.
* Fewer patients required labor induction with oxytocin.
* All these effects were achieved with out increasing maternal and neonatal morbidity. Hence PGE2 gel can be recommended as a useful and potent method of induction of labor with unfavorable cervix.
ACKNOWLEDGMENT
I am thankful to Mr. Gohar Said for typing and helping the manuscript.
REFERENCES
1. Grant JM. Induction of Labour. In. James D.K, Steer P.J, Weiner C.P, Gonik B.High Risk Pregnancy: management Options. 1999;2nd ed.1079-1101.
2. Induction of Labour. Evidence based clinical guideline No 9.2001.
3. American College of Obstetricians and Gynaecologists. Induction of Labour. Washington DC: ACOG; 1999. Practice Bulletin no 10.
4. Uldbjerg N, Ekman G, Malmstrom A. Ripening of the human uterine cervix related to changes in collagen, glycosaminoglycans and collagenolytic activity. Am J Obstet Gynecol 1983;147:662-6.
5. Calder AA. Pharmacological management of the unripe cervix in the human. In: Naftolin F, stubblefied PG, edition. Dilatation if uterine cervix. New x –ray: Ravin Press; 1980;317-33.
6. Cruz AS, Pinto JM, Valerioo. PGE2 gel for enhancement of priming and induction of labour at term inpatients with unfavorable cervix. Europe J Obstet Gynaeco Reprod Biol 1985;20:331-6.
7. Noah ML, Decoster JM, Fraser W. Preinduction cervical softening with endocervical PGE2 gel. A multicenter trial. Acta Obstet Gynecol scand 1987;66:3-7.
8. Prins RP, Bolton RN, Mark C. Cervical ripening with intravaginal prostaglandin E2 gel. Obstet Gynecol 1984;63:697-702.
9. Keirse MJ. Prostaglandins in preinduction cervical ripening. Metaanalysis of worldwide clinical experience. J Reprod Med 1993;38 (1):89-100.
10. Rafiq-ul-Islam, Sritanu Bhattacharryya, Bejoylarshmi Goswami. Intracervical PGE2 gel for cervical Ripening and induction of labour. J Obstet Gynecol Ind 2001;51(6):83-6.
11. Warke HS. Saraogi RM, Sanjwalla SM Prostaglandin E2 gel in ripening of cervix in induction of labour. J Postgrad Med 1999;45(1)05-9.
12. Trofather KF, Boners D, GAU DA, preinduction cervical ripening with prostaglandin E2 gel. Am J Obstet Gynecol 1985;153:268-71.
13. Thiery M, Decoster JM. Parewijck W. Noah ML et al. Enavcervical prostaglandin E2 gel for preinduction cervical sotening. Clin Obstet Gynecol 1984;27:429-39.
14. Jackson GM, Sharp HT, Varner MW. Cervical Ripening before induction of labour: a randomized trial of prostaglandin E2 gel versus low dose oxytocin. AMJ Obstet Gynecol 1994;171(4): 1092-6.
15. Turna JE. Burke MS. Poreeco RP. Weiss MA. Prostaglandin E2 in tylose gel for cervical ripening before induction of labour. J Reprod Med 1987;32(11):815-21.
16. Sayeda Batool Mazhar, Saba Sarwar, Ghazala Mahmod. Induction of labour, A Randomized trial comparing prostaglandin E2 pessary, intracervical foly catheter and extra a amniotic saline infusion. J Surg 2000;19-20:12-8.
17. Perry MY, Leaphart W. Randomized trial of intra cervical vs. posterior fornix dinoprostone for induction of labour. Obstet Gynae 2004;103:13-7.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk