|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
An audit of 149 consecutive breast
biopsies in Ibadan, Nigeria
Irabor DO1, CA. Okolo2
ABSTRACT
Objective: To study the outcomes of one hundred and forty nine consecutive breast biopsies in both male and female patients in one arm of the general surgery division of the department of surgery, university college hospital Ibadan.
Methodology: A retrospective study of the case files and histopathology reports of 149 patients who had biopsies of the breast from May 1996 to September 2004.
Results: The study showed that below the age of 30 years, there was no malignancy detected in 85 breast biopsies, however as the age increased it was seen that less than one out of four biopsies were malignant when the patients were aged between 31 and 40 years, rising to one out of four biopsies for the 41-50 and 51-60 age-groups. The 61-70 yielded roughly one out of three whilst two out of three breast biopsies were malignant in the 71-80 age-groups.
Conclusions: Majority of breast lumps are benign and women have a probability of one chance in 10 that their biopsies may be malignant. However under 30 years this is unlikely. Above the age of 40 years the chance of malignancy rises to a one in four which will strongly support screening methods for women above 40 years. For record purposes, fibroadenoma is still the most common breast lesion in women under 30 years and invasive ductal carcinoma is the most common histopathological type of breast cancer in Ibadan, Nigeria.
KEY WORDS: Breast lumps, Biopsies, Nigeria.
Pak J Med Sci April - June 2008 (Part-I) Vol. 24 No. 2 257-262
1. Dr. Moazzam Ali Atif,
2. Dr. Hassan Ali,
3. Dr. Tariq Mahmood,
1-3: Department of Medicine,
Jinnah Postgraduate Medical Centre,
Karachi � Pakistan.
1. Dr. Irabor DO,
Senior Lecturer,
Department of Surgery,
College of Medicine,
University of Ibadan,
Ibadan � Nigeria.
2. Dr. CA. Okolo,
Lecturer,
Consultant Pathologist,
College of Medicine,
University of Ibadan,
Ibadan � Nigeria.
Correspondence
Dr. DO. Irabor,
Surgery Department,
University College Hospital Ibadan,
P.M.B. 5116 Ibadan,
Nigeria.
E-MAIL: dirabor@comui.edu.ng
irabordavid@yahoo.com
* Received for Publication: December 31, 2007
* Accepted: January 17, 2008
INTRODUCTION
The presence of a breast lump strikes most educated and enlightened women with apprehension, uncertainty, fear and sometimes depression.
1 Fortunately not all breast lumps are malignant; in fact the majority is not. However not one surgeon can stick his head out to affirm with certainty that, clinically, a breast lump is benign even if the age of the patient and features of the lump do not support malignancy.2,3 The final arbiter is histologic tissue diagnosis which can be achieved from tissue biopsy obtained by different techniques such as needle, core, incisional or excisional biopsies.This study reviews the tissue diagnoses of patients (both male and female) who presented to one of the general surgery units of the University College Hospital Ibadan with complaints of a lump or lumps in one or both breasts. It is hoped that apart from shedding some light on the probability of having a benign or malignant outcome after breast lump excision in Ibadan, Nigeria, the paper may provide useful data for counseling patients, strengthening advocacy for better breast health awareness and supporting purposeful screening measures.
4METHODOLOGY
This is a retrospective study of all the patients who had excision of breast lumps in one surgical unit of the University College Hospital Ibadan, Nigeria between May 1996 and September 2004, a period of eight years and three months. All the patients were initially seen at the surgical outpatients� clinic where they were interviewed, examined and scheduled for excisional or incisional biopsies depending on the sizes of the lumps.
All the biopsies were performed as day case procedures under 0.5% xylocaine where the average volume used in infiltration for each patient did not exceed 10ml except in patients with bilateral disease. The incisions were circumareolar for the most when feasible (for cosmetic reasons) and circumferential when the former was not possible due to site of the lump. No patient had to be converted to general anesthesia. No patients were transfused. The incision was closed with subcuticular stitches using either 3-0 vicryl or 3-0 nylon. The patients went home immediately after operation on oral analgesics. Antibiotics were not prescribed. Those without drains were seen at the outpatient�s clinic 9-days later; those with drains were seen 48-hours after operation to remove the drain then were seen one week after. The subcuticular nylon stitches were gently withdrawn on the 9
th day post-surgery at the outpatient�s clinic. The tissue biopsy specimen were fixed in 10% formalin and sent to the histopathology laboratory. The pathologists did the gross description and cut up of the specimen and the tissue slides were stained using Haematoxylin and Eosin. The slides were read and interpreted by the pathologists who made the histopathology reports available.The histopathology reports were usually available from the pathology department three weeks after surgery, thus after the 1
st post-operative visit to the outpatient clinic most patients were given a 3-week appointment. Decisions about further management were taken at this time.RESULTS
The period of study was 100-months; May 1996-September 2004, and a total of 149 patients were studied; 5 males and 144 females giving a Male/Female ratio of 1:29. The age range was 15 to 72 years.
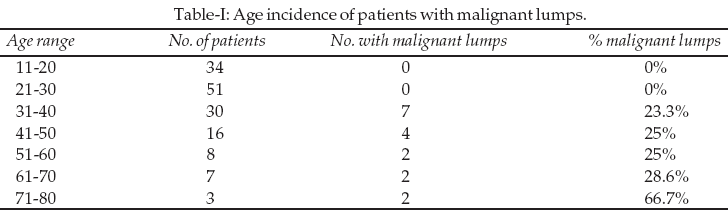
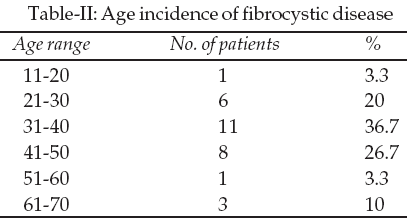
The total number of lumps was 161 (11 patients had bilateral lesions) with the ratio of cancerous to benign lumps of 1:8.5 (17 to 144). It was noticed that the cancerous lumps comprised 10.56% of the total number of biopsies while fibrocystic disease accounted for 18.60% and the majority (52.80%) was fibroadenomata; in all 85 patients in had fibroadenoma, 30 patients had fibrocystic disease while 17 had carcinoma. The percentage of patients with cancerous lumps rose gradually from the 30-40 age group to the 70-80 age group (Table-I). The mean age of patients with carcinoma was 48.8 years; those with fibrocystic disease 39.5 years, fibroadenoma 24.4 years and benign phylloides tumor 18.8 years. Most of the cases of fibrocystic disease occurred in women aged 31 to 50 years (Table-II).
The benign phylloides tumor accounted for 3.1% (5 patients) of the total number of biopsies and the remaining 15% comprised a range of diagnoses like duct ectasia, lactational changes, traumatic fat necrosis, gynecomastia, lipoma, ductal papilloma and acrine acrospiroma, to name some (Table-III).
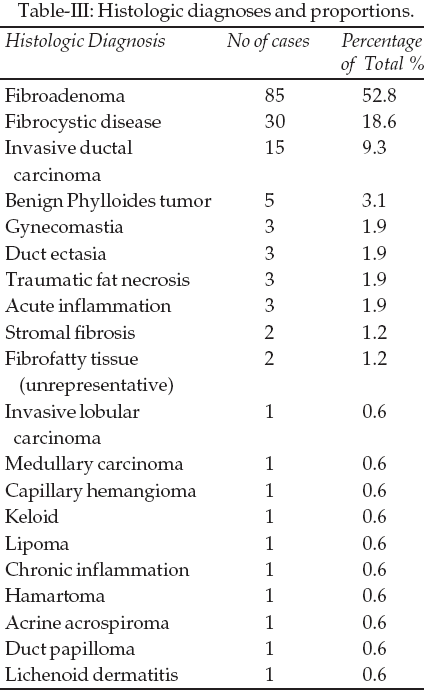
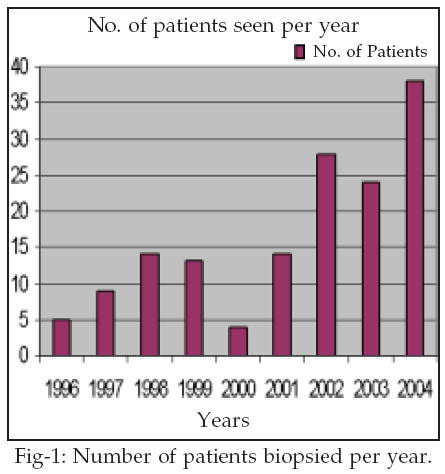
Histopathology of the malignant lumps showed that 15 out of the 17 had Invasive ductal carcinoma (88.2%) with the two remaining patients having Medullary and Invasive lobular carcinomas respectively (5.9% each). Two patients (36 and 50 years) had background fibrocystic disease associated with their carcinoma and two other patients, a 46 year-old female and a 72 year-old male had associated squamous metaplasia. The number of cases presenting for biopsies over these 8 years doubled in the year 2002 and have increased in 2004 (Fig.-1).
Out of the five male patients in this study there were three with gynecomastia; these were two 58- year-old men with unilateral left-sided breast enlargement and one 20 year-old man with a right-sided breast enlargement. One 70 year-old man had fibrocystic disease with epitheliosis of the left breast and the last male in this series was a 72 year-old man with invasive ductal carcinoma with squamous metaplasia of the right breast.
DISCUSSION
Most breast lumps are likely to be benign and roughly one out of ten biopsies turn out to be malignant, but that is only generally speaking.
2,3 When set against the age-range of the patients it was seen that below the age of 30 years, there was no malignancy detected in 85 breast biopsies. As the age increased it became visibly apparent that less than one out of 4 biopsies were malignant when the patients were aged between 31 and 40 years, rising to one out of four biopsies for the 41-50 and 51-60 age-groups. The 61-70 yielded roughly one out of three whilst two out of three breast biopsies were malignant in the 71-80 age-group (Table-I). Breast cancer has been said to be exceedingly rare in females under 30 years and this information agrees with the age-incidence of breast cancer that it rises with the age of the patient.2-5For our patients with benign lumps, histopathology of the benign lumps showed fibroadenoma to be the most common breast lump with 52.8%, followed by fibrocystic disease with 18.6% and benign phylloides tumor 3% which agrees with the fact that the most common breast lump in females under the age of 30 years is fibroadenoma.
1-5 Several studies done in Nigeria, Saudi Arabia, Nepal and India have shown that the most common breast lump in females is the fibroadenoma followed by fibrocystic disease.6-14 In a study of 302 females under the age of 21 years with breast lumps using fine-needle aspiration cytology it was found that no malignancies were present.15 In the absence of a family history it is said that a woman in her 30�s has a one in 250 chance of developing carcinoma of the breast during her next 10 years and this rises to one in 75 in her 40�s for the subsequent 10 years.16 Our patients between the ages of 30-50 had roughly one out of four biopsies being positive for cancer. Fibroadenoma has been shown from histological studies to resemble closely hyperplastic lobules commonly found in normal breasts and the induction of this lesion by hormone replacement therapy and in younger nulliparous women taking the oral contraceptive pill may further underscore the fact that the hyperplastic stimulus is hormonal, probably oestrogenic.17 Most fibroadenomata grow to only about 3cm in diameter and many spontaneously regress.17 A study actually suggests the safety of non-operative management of cytologically-confirmed fibroadenoma; these authors found that 38% of fibroadenomata resolved over five years.18Fibrocystic disease is a disease of the more mature female and in this study majority fell between the age range 31-50 (63.4%)
2,3,5 (Table-II). The mean age of patients with fibrocystic disease in this study was 39.5 years and this is slightly higher when compared with the recent study in Ghana where this age was 31.8 years.2 Fibrocystic disease is an important breast lesion because of its high frequency (second to fibroadenoma in this study) and the ability of some of its subtypes to mimic the clinical and radiographic appearance of carcinoma.19 Hormones also play a role in its development but the exact pathogenesis still remains to be established.20Atypical epithelial hyperplasia is the most important and troublesome component of fibrocystic disease because of its possible relationship with carcinoma.
19,21 As seen in the results of this study, two of the patients with invasive ductal carcinoma also had background fibrocystic changes.The mean age of our patients diagnosed with breast cancer was 48.8 years, close to the Ghanaian study of 50.1 years
2 and the most common histopathological type was invasive ductal carcinoma and this conforms with several reports.3,4,10 We also found a difference in the mean ages of our patients who presented with fibroadenoma and benign phylloides tumor; 24.4 years to 18.8 years respectively. Phylloides tumors are said to be rare fibroepithelial tumors which account for less than 1% of all breast neoplasms.19 This study however yielded 3.1% of the excisions performed. Benign phylloides tumor is referred to as giant fibroadenoma in some studies because clinically they are smooth, rounded multinodular lesions that may be indistinguishable from fibroadenomas.4 They are also indistinguishable from fibroadenomas mammographically.15 The phylloides tumor has been reported to occur at any age, however the median age is said to be generally in the 5th decade of life or at least a decade older than the mean age of patients with fibroadenoma.4,14,15 The converse is what we found in this study as the 4 patients in this study were persistently younger than the mean fibroadenoma age. The problem with phylloides tumor is that the malignant component may also appear innocuous until distal metastases appear; this is why some authors may be wary of advising non-operative management for breast lumps that have features of fibroadenoma.22 It is also important to note that in this study one of the cases (acrine acrospiroma) was not really a primary breast neoplasm but a skin adnexal tumor in the skin of the breast presenting clinically as a breast lump.23 This also applies to the single cases of keloid, capillary hemangioma and lichenoid dermatitis respectively, which are skin lesions (Table-III). However, the fact that they were located on the skin of the breast prompted the patients to seek for surgical consultation. Excision of these lesions and histopathological examination was the only way to assure the patients of the benignity or otherwise of the lesions. One has to keep in mind that Paget�s disease of the breast, which is a premalignant condition, presents as a skin lesion.In a previous study done in this institution in 1994, it was reported that only 39% of the breast biopsies were benign,
14 however it seems that a lot has changed in the sub region since then as this study produced 89.4% benign masses, this is closer to the 75-80% obtained in a sister West African country.4 Stimulation of public awareness to breast cancer in Ibadan Nigeria was championed by a non-governmental organization, BRECAN; the breast cancer association of Nigeria, which was inaugurated in 1997. It is debatable whether the significant increase in the number of patients presenting to the hospital from1998 onwards are due to its activities, however there is no doubt that more women with breast lumps are having surgery in this hospital (Figure-1). We see some male patients rarely; as in this study over a 100-month period only five male patients presented (3.4% of the total).In summary, for counseling purposes this study has reaffirmed that majority of breast lumps are benign; that women may have a probability of one chance in 10 that their biopsies may be malignant; and that under 30years it is unlikely. However, in view of the fact that certain histologic features in breast biopsies such as atypical ductal hyperplasia in benign breast lumps may be linked with malignancy, it is advised that histologic assessment for all breast lumps should be routinely done to evaluate the risk factors for malignancy.
For advocacy purposes we have seen that above the age of 40 years the chance of malignancy rises to one in four, which will strongly support screening methods for women above 40 years. Fibroadenoma is still the most common breast lesion in women under 30 years and invasive ductal carcinoma the most common histopathological type of breast cancer in Ibadan, Nigeria.
ACKNOWLEDGEMENTS
Our gratitude to the secretarial staff, laboratory scientists, resident doctors and consultants of the Pathology Department U.C.H. Ibadan for making results of biopsy specimens available in good time.
REFERENCES
1. Deane K, Degner L. Information needs uncertainty and anxiety in women who had a breast biopsy with benign outcome. Cancer Nursing 1998;21:117-26.
2. Morrow M. The Breast, In Surgery: Scientific Principles and Practice. Greenfield LJ (Ed.) 3rd Edition, Chapter 58, 2001;1334-72.
3. Kerlikowske K, Smith-Bindman R, Britt-Marie L, Grady D. Evaluation of abnormal mammography results and palpable breast abnormalities. Ann Intern Med 2003;139:274-84.
4. Ohene-Yeboah MOK. An audit of excised breast lumps in Ghanaian women. West Afr J Med 2005;24:252-5.
5. Sterns EE. Age-related breast diagnosis. Can J Surg 1992;35:41-5.
6. Adesunkanmi AR, Agbakwuru EA. Benign breast disease at Wesley Guild Hospital, Ilesha, Nigeria. West Afr J Med 2001;20:146-51.
7. Onuigbo W. Breast fibroadenoma in teenage females. Turk J Pediatr 2003;45:326-8.
8. Adeniji KA, Adelusola KA, Odesanmi WO. Benign disease of the breast in Ile-Ife: A 10-year experience and literature review. Centr Afr J Med 1997;43:140-3.
9. Otu AA. Benign breast tumors in an African Population. J Roy Coll Surg Edinb 1990;35:373-5.
10. Kathcy KC, Datubo-Brown DD, Gogo-Abite M, Iweha UU. Benign breast lesions in Nigerian women in Rivers state. East Afr Med J 1990;67:201-4.
11. Chiedozi LC, El-Haq IA, Kollur SM. Breast diseases in the Northern region of Saudi Arabia. Saudi Med J 2003;24:623-7.
12. Khan S, Kapoor AK, Khan IU, Shrestha GB, Singh P. Prospective study of pattern of breast disease at Nepalgunj Medical College (NGMC), Nepal. Kathmandu Uni Med J 2003;1:95-100.
13. Chaudhuri M, Sen S, Sengupta J. Breast lumps: A study of 10 years. J Indian Med Assoc 1995;93:455-7.
14. Ihekwaba FN. Benign breast disease in Nigerian women: a study of 657 patients. J Roy Coll Surg Edinb 1994;39:280-3.
15. Pacinda SJ, Ramzy I. Fine-needle aspiration of breast masses, a review of its role in diagnosis and management in adolescent patients. J Adolescent Health 1998;23:3-6.
16. Sauven P. Guidelines for the management of women at increased familial risk of breast cancer. European J Cancer 2004;40:653-65.
17. Bundred NJ. Aetiological factors in benign breast disease. Br J Surg 1994;81:788-9.
18. Cant PJ, Madden MV, Coleman MG, Dent DM. Non-operative management of breast masses diagnosed as fibroadenoma. Br J Surg 1995;82:792-4.
19. Collins LC, Baer HJ, Tamimi RM, Connolly J, Colditz G, Schnitt S. Magnitude and laterality of breast cancer risks according to histologic type of atypical hyperplasia; results from the nurses health study. Cancer 2007;109:180-7.
20. Angeli A, Bradlow HL, Dogliotti L. Endocrinology of the breast. Basic and clinical aspects. Ann NY Acad Sci 1986;464:640-1.
21. Page DL, Dupont WD. Histopathologic risk factors for breast cancer in women with benign breast disease. Semin Surg Oncol 1988;4:19-22.
22. Parker SJ, Harries SA. Phylloides tumor. Postgrad Med J 2001;77:428-35
23. Winkelman RK, Wolff K. Solid-cystic hidradenoma of the skin. Clinical and histopathologic study. Arch Dermatol 1968;97:651-61.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk