|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
Non-B, Non-C Hepatitis as a cause of Advanced Chronic
Liver Disease requiring medical admission at
a rural centre in Pakistan
Muhammad Ali1, Syed Zafar Abbas2,
Farhat Sultana3,
Waseem Akhtar4, Steve Shaw5, Syed Qamar Abbas6
ABSTRACT
Objectives: To study the frequency and mortality of hepatitis B and C negative chronic liver disease (CLD) at a rural tertiary centre in Pakistan.
Methodology: Data was collected retrospectively from the case notes of all the 176 patients consecutively admitted with advanced CLD in our medical ward during one year period. Patients, who were seropositive for hepatitis B and / or C, were separated from those who were negative for them, and the data was analysed.
Results: Thirty five patients (20%) were negative for both viral markers. They were more likely to die during the admission than those who were seropositive (11% VS 25% - p = 0.029).
Conclusions: A significant proportion of patients with CLD are negative for viral markers. These patients are at higher risk of mortality, and need testing for other causes of CLD as some of them may benefit from curative treatments available.
KEYWORDS: Viral Hepatitis, Chronic Liver Disease, Medical admission, Mortality.
Pak J Med Sci April - June 2008 (Part-I) Vol. 24 No. 2 278-282
1. Muhammad Ali, FCPS, MRCP,
Consultant Physician
2. Syed Zafar Abbas, FRCP, FEBG, FACP,
Consultant Gastroenterologist
3. Farhat Sultana, MBBS,
House Doctor
4. Waseem Akhtar,
Department of Medicine,
Muhammad Medical College Hospital,
Mirpurkhas, Pakistan
5. Steve Shaw, PhD,
Senior Lecturer in Statistics
School of Mathematics and Statistics,
University of Plymouth, Plymouth, UK
6. Syed Qamar Abbas, MA, MBBS;
Associate Specialist, Palliative Care Medicine
St. Clare Hospice, Hastingwood, Essex, UK
Correspondence
Dr. Muhammad Ali
Consultant Physician,
Muhammad Medical College Hospital,
Hyderabad Road, Mirpurkhas
Sindh - Pakistan.
E-mail:
dr_muhammad_ali@hotmail.com;
dr_mohammad_ali@yahoo.com
* Received for publication: December 17, 2007
* Revision Received: March 12, 2008
* Revision Accepted: March 15, 2008
INTRODUCTION
Chronic Liver Disease (CLD) has become a major public health problem. In Europe and USA excessive consumption of alcohol, and in Asian countries HBV and HCV are responsible for 75% of cases of CLD.
1 In Pakistan it is mainly due to viral infection especially due to hepatitis B virus (HBV) and hepatitis C virus (HCV), although other causes like alcohol and some metabolic diseases are also identified.2 The spread of these viruses is perpetuated by the reuse of disposable syringes by some general practitioners and quakes especially in the rural areas,3,4 which is responsible for 69% of all cases in our region (unpublished data). In Pakistan the prevalence of anti HCV antibodies is estimated to be approximately 6%, and that of hepatitis B s antigen to be around 3%.5,6 Chronic hepatitis B and/or C may lead to CLD and its consequences namely portal hypertension, hepatic insufficiency and hepatocellular carcinoma.7 Although CLD is commonly caused by viral hepatitis in Pakistan, it may have some other relatively less common and potentially treatable aetiology, including autoimmune liver disease, primary billiary cirrhosis, Wilson’s disease and haemochromatosis. At our centre, 17% of all patients tested had evidence of exposure to HCV (unpublished data). However patients with CLD, who do not have evidence of exposure to either of the two viruses, have not yet been studied in this region. The purpose of this study was to find out the proportion of patients who had CLD but were negative for both hepatitis B and C viral markers, and to compare the demographic features and mortality of this group of CLD, with those with a viral aetiology.PATIENTS AND METHODS
The records of all 176 patients who were admitted in the medical ward of our hospital during one year period between August 2005 and July 2006 with CLD, were studied. The diagnosis of CLD was based on clinical, laboratory and ultrasound scan findings. The clinical features included stigmata of cirrhosis, e.g palmar erythema, dupuytran’s contracture, spider naevi, gynaecomastia, loss of body hair, spleemomegaly, caput medusae, ascites, jaundice haematemesis and /or melaena, hepatic encephalopathy. Laboratory findings included abnormal LFTs, reversed AST: ALT ratio, low platelets, prolonged prothrombin time, low serum albumin, raised serum ascitic albumin gradient (SAAG). Ultrasound scan features suggestive of cirrhosis included shrunken liver, fine nodular margins of liver, altered echotexture, coarse parenchyma, splenomegaly, ascites, distended portal or splenic veins. Any patients that was admitted with CLD satisfying above diagnosis criteria was included in the study and no such patient was excluded.
All patients had advanced CLD with features requiring admission. To save the unnecessary expenses to the patients, viral hepatitis markers (HBs antigen and anti HCV) had in our centre for those admitted patients who either did not have these tests done prior to admission (n=10), or to confirm the results of those tested before admission and reported seronegative (n=33). Chi square tests were done to test significance. A p- value of less then 0.05 was considered significant. Odds ratio (OR) with 95% confidence interval (95%CI) were calculated for findings with significant p values.
Approval was taken from hospital’s Research Ethics Committee to undertake this study.
RESULTS
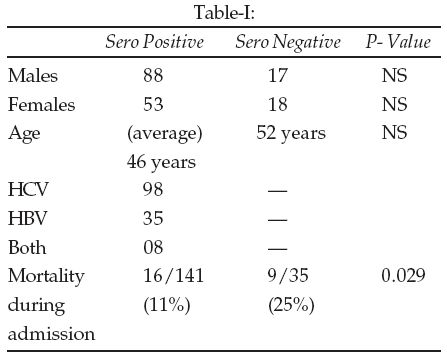
All 176 patients who were admitted with CLD during the study period, were divided into two groups - those who were seropositive for hepatitis B and / or C, and those who were seronegative. There were in total 71 females (40%) and105 males (60%). Out of the total, 35 (20%) patients were found to be seronegative and the remaining 141 (80%) were positive for either or both of the viruses. The average age in the seronegative group was 52 years whereas it was 46 years in the viral marker positive group. There were 18 females (52%) and 17 males (48%) in the seronegative group, and 53 females (38%) and 88 males (62%) in the other group (p = 0.14). Out of the total cases, 98 patients (70%) had CLD due to HCV alone, 35(25%) were positive for HBV and 8 (6%) patients were positive for both. The remaining 35 were negative for both the markers. The indications for admission of these patients were as follows - 40 for non-specific febrile illnesses, 35 for bleeding varices, 31 for hepatic encephalopathy, 25 for hepatorenal syndrome, 20 for profound ascites and 25 for other complications. Twenty five of the totals of 176 patients (14%) died during the course of admission. Among them 16/141 (11%) deaths occurred in the seropositive group and 9/35 (25%) in the seronegative group (p = 0.029; OR = 0.37, 95% CI = 0.15 - 0.93) (Table-I).
DISCUSSION
The main cause of chronic hepatitis and CLD in Pakistan is said to be HBV and HCV2and this study has also confirmed this. Various studies in Pakistan estimate the prevalence of exposure to HBV to be between 2.28 and 3.3% and HCV to be at 6 %,5-9 although our own unpublished data suggests these figures to be as high as 17% for HCV in our region. In this study vast majority of patients had HCV (56%) as a cause of CLD which is in accordance with previous studies as well.1,10-13 HBV incidence has decreased in the recent past. It appears to be because of increased awareness in the general public and due to the hepatitis B vaccination.14 Dual infection by both B and C were seen in 6% of cases. In another study in Pakistan combined infection was seen in 8% of cases.13 Overall there were more men with CLD than women (60% vs. 40%). Other studies have also shown CLD to be more prevalent in males.13-17 This is probably because males are more exposed to common risk factors. Although a greater proportion of women were seronegative than men (51 vs. 48%) as compared to the same for seropositive group (37 vs. 62%), this was not statistically significant (p = 0.14). The average age of seropositive patients in our study was 46 years which is comparable with studies done previously in Pakistan18 and in South East Asia.19The reasons for admission were mostly decompensated cirrhosis and its known complications. Bleeding varices, hepatic encephalopathy, hepatorenal syndrome and ascites accounted for 63% of all the admissions. The remaining 37% were admitted because either they developed a febrile illness and got extremely unwell or they developed non CLD related illnesses. The mortality during admission was unsurprisingly high at 14.2%
Although chronic Hepatitis B and C still account for majority of the patients with CLD, other relatively rare causes should not be overlooked. These include the consumption of hepatotoxic drugs like anti tuberculosis drugs,
20 alcohol, Wilson s disease,21 autoimmune hepatitis,22 primary billiary cirrhosis, haemochromatosis and other rare metabolic illnesses.23 In our study non B non C CLD was found in around 20% of admitted cases. In another study in Pakistan, the incidence of non-B, non-C CLD was estimated at 6% but that study was relatively small, and was done on only 55 patients.24There appears to be a difference in the mortality rates of those patients with CLD who have a viral aetiology and those who are seronegative. In a study done in Northern Pakistan, out of a total of 33 deaths caused by CLD, only 9% had a non-viral aetiology. However, like our study, they were not further investigated. The rest of the patients had HCV and/or HBV.
25 In our study, out of a total of 25 CLD patients who died, 16 (64%) had a viral aetiology and 9 (36%) did not. This is significantly higher than the above mentioned study. However the study mentioned above did not elaborate on the number of the patients admitted in either group and hence the results cannot be compared further. In our study, a total of 176 patients were admitted with CLD – 141 in viral aeiology positive group and 35 in the seronegative group. There was a significant difference in the mortality rate among the two groups in our study. A total of 25 patients died - 16/141 patients in seropositive group and 9/35 in seronegative patients – p = 0.029; OR = 0.37 – 95%CI = 0.15 – 0.93. Hence there is evidence for higher risk of death in seronegative patients.Mortality in patients with cirrhosis caused by HCV and HBV, and also non-viral factors is also significant. For example, mortality in cirrhotic patients with Autoimmune hepatitis is higher than general population. One recent study calculate the standardized mortality ratio of 2.5 (1.62 – 3.40) for this disease.
26 This shows the importance of investigating seronegative patients further, preferably in the earlier stage of their illnesses. Various factors are potentially restricting in this regard. Firstly the lack of education among patients and also a low level of awareness among their primary physicians. There is a dire need of raising awareness of investigating such patients among the general practitioners in particular as some of the diseases causing such problems are potentially curable or controllable. Appropriate treatment started at earlier stages of disease can prevent a significant number of unnecessary and young age morbidity and mortality. This will also have financial implications as many of such deaths occurred at economically productive age. Secondly, there is a huge problem of financial restrain. Pakistan is poor country where 17% of people live their lives under the poverty lines defined as household earning of less then $1 per day .In addition 73.6% of the population earns less then $2 per day.27 Our centre is situated in a rural area of Pakistan, where the problem of poverty is even bigger. The investigations needed for patients requiring tests beyond basic HBV and HCV are expensive and out of reach for a vast majority of our population .Hence the state and private organizations must work together to help such patients.This is first study of its kind done in rural Pakistan Population. It has raised a very important issue of investigating patients with CLD with negative viral markers further which may save many lives. However, this study is limited in that patients with negative basic viral markers could not be investigated further because of financial reasons. This would have helped us to classify them further into exact cause of non-viral liver disease. For the same reason detailed viral studies could also not be done such as hepatitis B e antigen, antibodies and core antibodies.
Recommendations: This study highlights the importance of screening for those relatively rare causes of CLD in patients who do not test positive on viral markers studies.
As such investigations are expensive and out of the reach for a majority of our patients, government and private institutions must join hands to help such patients, which may help avoiding unnecessary mortality.
CONCLUSIONS
Although chronic viral hepatitis is responsible for causing CLD in a majority of our patients, there are other potential causes which are as yet not fully investigated. Such patients are at higher risk of mortality, but may be amenable to curative treatments.
REFERENCES
1. Podolsky DK, Isselbacher KJ. Cirrhosis and alcoholic liver disease. In Fauci AS, Braunwald E, Isselbacher KJ, William JD, Martin JD, Kasper DL. (ed.): Harrison’s Principles of Internal Medicine, 14th ed. New York; McGraw Hill 1998;2:1704-20.
2. Zuberi FF, Zuberi BF, Khan MA, Khan MH. Frequency of rectal varices in patients with Cirrhosis. J Coll Physician Surg Pak 2004;2;94-7.
3. Shaikh MA, Shaikh WM, Solangi GA, Abro H. Frequency and transmission mode of HCV virus in northern Sind. J Coll Physic Surg Pak 2003;13(12);691-3.
4. Khokhar W, Gill ML. Serological profile of incidentally detected asymptomatic hepatitis B positive subjects. J Coll Physic Surg Pak 2004;14(4):208-10.
5. Hamid S, Umar M, Alam A, Siddiqui A, Qureshi H, Butt J and Members of the Consensus Panel. PSG Consensus Statement on Management of Hepatitis C Virus Infection 2003. J Pak Med Assoc 2004;54(3):146-9.
6. Abbas Z, Jafri W, Shah SHA, Khokhar N, Zuberi SJ and Members of the Consensus Panel. PSG Consensus Statement on Management of Hepatitis B Virus Infection – 2003. J Pak Med Assoc 2004;54(3):150-8.
7. Alter MJ. Epidemiology of Hepatitis C virus infection. World J Gastroenterol 2007;7:13(17):2436-41.
8. Khattak MF, Salamt N, Bhatti FA, Qureshi TZ. Seroprevelance of hepatitis B, C and HIV in blood donors in Northern Pakistan. J Pak Med Assoc 2002;52;398-402.
9. Kakepoto GN, Bhally HS, Khaliq G, Kayani N, Burney IA, Siddiqui T, et al. Epidemiology of blood borne viruses: a study of healthy blood donors in Southern. Pakistan. Southeast Asian J Trop Med Public Health 1996;27(4);703-6.
10. Armstrong GL, Alter MJ, McQuillan GM. The past incidence of HCV infection. Hepatology 2000;31(7):77-82.
11. Brown RS, Gaglio PJ, Scope of worldwide Hepatitis C problem. Liver transplantation 2003;9(suppl 3); S10-13.
12. Bhatti FA, Shaheen N, Tariq W, Amin M, Saleem M. Epidemiology of Hepatitis C in blood donors in Northern Pakistan. Pak Armed Forces Med J 1996;46(2);91-2.
13. Hussain I, Nasrullah M, Shah AA. Prevalence of Hepatitis B and C Viral infections in Cirrhosis of Liver in Pakistan. Pak J Gastroenterol 1998;12(1-2):7-11.
14. Mast EE, Margolis HS, Fiore AE. A comprehensive immunization strategy to eliminate hepatitis B virus infection in USA. Recommendation of the advisory committee on immunization practices (ACIP) Part 1: immunization of infant, chldreen, and adolescents. MMWR Morb Mortal Wkly Rep. 2005;54(RR16);1-23.
15. Mohsen AH and Trent Treat HCV study group. The epidemiology of Hepatitis C in a UK health regional population of 5.12 million. Gut 2001;48;707-13.
16. Tong MJ, El Farra NS, Riekes AR, Co RL. Clinical outcome after transfusion associated hepatitis C. N Eng J Med 1995;332:1463-6.
17. Sherlock S, Foz RA, Niazi SP, Scheuer PJ. Chronic liver disease and liver cancer with hepatitis associated antigen in serum. Lancet 1970;1;1243.
18. Iqbal S, Ruknuddin.Liver cirrhosis in North West Frontier province of Pakistan. J Coll Physician Surg Pak 2002;12:289-91.
19. Christopher JM, Stephen AL. Epidemiology of hepatitis C in the East. Semin Liver Dis 1995;15:15-20.
20. Bhadauria S, Singh G, Sinha N, Sirivastava S. Isoniazid induces oxidative stress, mitochondrial dysfunction and apoptosis in Hep G2 cells. Cell Mol Biol (Noisy-le grand) 2007;53(1):102-14.
21. Ferenci P, Cztonkowska A, Merle U, Ferenc S, Gromadz Ka G, Yurdaydin C, et al. Wilson s disease. Gastroenterology 2007;132(4):1294-8.
22. Krawitt EL. Autoimmune Hepatitis. N Eng J Med 2006;354:54-66.
23. Fink SA, Schilsky, Michael LB. Inherited metabolic disease of the liver. Curr Opin Gastroenterol 2007;23(3):237-43.
24. Farooqi JI, Khan PM. Viral aetiology of Liver cirrhosis patients in Swat. Pak J Gastroenterol 2002;16(2):39-42.
25. Khokhar N, Niazi SA. Chronic liver disease related mortality pattern in Northern Pakistan. J Coll Physicians Surg Pak 2003;13(9)495-7.
26. Hoeroldt BS, McFarlane E, Campell M. Standardized mortality ratio in autoimmune hepatitis. Gut 2008;57(Suppl I):A1-A172.
27. List of countries by percentage of population living in poverty. Available at: http://en.wikipedia.org/wiki/List_of_countries_by_percentage_of population_living_in_poverty (Accessed 15h December 2007)
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@