|
|
||||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||||
|
ISSN 1681-715X |
||||||
|
||||||
|
- |
||||||
|
ORIGINAL ARTICLE |
||||||
|
- |
||||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||||
|
|
||||||
|
||||||
|
|
||||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||||
|
ISSN 1681-715X |
||||||
|
||||||
|
- |
||||||
|
ORIGINAL ARTICLE |
||||||
|
- |
||||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||||
|
|
||||||
|
||||||
Colostomy in children: Indications and
common problems in Benin City, Nigeria
Osifo OD1, Osaigbovo EO2, Obeta EC3
ABSTRACT
Objective: To evaluate the indications for colostomy and highlight associated problems as well as its contribution to the successful treatment of children.
Methodology: This is a retrospective study of the indications, complications, parents/caregivers acceptance and outcome of colostomy in children over a ten-year period at the University of Benin Teaching Hospital, Benin City, Nigeria.
Results: There were 46 children aged two days and 15 years (mean 3 months ± 2.1) with male/female ratio 2.8:1. Congenital anomaly was the major indication and accounted for 40 (87%) with associated higher morbidity and mortality and an observed significant statistical difference compared with the acquired indications (P<0.0001). Anorectal anomaly accounting for 22 (48%) and Hirschsprung’s disease 18 (39%) were the congenital indications. Morbidity and mortality were mostly associated with children that had anorectal anomaly (P=0.0021). Acquired indications were mainly rectovaginal fistulae, perineal and left colonic injury which accounted for 6 (13%). Skin excoriation 39 (85%), colostomy prolapse 15 (33%) and persistent odour 21 (46%) resulted in poor acceptance by 10 (22%) parents/caregivers. Adequate preoperative counselling, skin protective paste and regular washing of colostomy site alleviated the complications. Wound infection and overwhelming sepsis were difficult to control in 14 (31%) with resultant six (13%) mortalities.
Conclusion: Colostomy still has much to offer in emerging paediatric surgery units. Adequate preoperative counselling of parents/caregivers, good stoma care and early stoma closure gave good results in our setting.
KEYWORDS: Colostomy, Children, Common Problems.
Pak J Med Sci April - June 2008 (Part-I) Vol. 24 No. 2 199-203
1. Osifo OD,
2. Osaigbovo EO,
3. Obeta EC
1-3: Paediatric Surgery Unit,
Department of Surgery,
University of Benin Teaching Hospital,
Benin City,
Nigeria.
Correspondence:
Osifo O.D,
Paediatric Surgery Unit,
Department of Surgery,
University of Benin Teaching Hospital (UBTH),
Benin City,
Nigeria.
E-mail: Leadekso@yahoo.com
* Received for Publication: November 13, 2007
* Revision Received: February 8, 2008
* Revision Accepted: February 12, 2008
INTRODUCTION
The construction of intestinal stoma (temporary or permanent) is an established procedure in surgery.
1 Colostomy is a commonly constructed intestinal stoma in children and majority are done during neonatal period with attendant high anesthetic and surgical complications.2,3 This is because indications in children are mainly congenital anomaly and this results in most stoma being constructed as emergency life saving procedure in neonates and children that may be clinically unstable.4,5In many centers in Nigeria, attention is shifting from the use of temporary colostomy to a single stage repair of anorectal anomaly and Hirschsrung’s disease because of the complications associated with stoma in children. As a result of lack of facilities and manpower needed to carry out extensive neonatal surgery and place unstable patients under long period of general anesthesia, many centres in this sub region still create colostomy as a routine procedure, until the children are fit to stand long hours of surgery.
6-9 This makes stoma associated problems rampant in many emerging paediatric surgical centres in this sub region.The aim of this ten-year retrospective study is to analyze the indications and problems associated with colostomy in a tertiary hospital in order to improve results, particularly among clinicians working in resource poor regions.
METHODOLOGY
University of Benin Teaching Hospital is a tertiary hospital located in the South-south Geopolitical Zone in Nigeria. Cases are referred from hospitals within the subregion and other health institutions including unorthodox healthcare providers. In the period, January 1997 to December 2006, 51 children had colostomy at the Centre. Adequate records were available for 46 patients and these have been retrospectively reviewed for age at colostomy formation, sex, indications for colostomy, types of colostomy, duration patients had the colostomy, complications recorded and outcome of treatment. The patients (n=5) whose case files were not available for analysis were excluded from the study.
The data obtained were analyzed using SPSS and presented as count, frequency and percentage. Categorical data were analyzed using Chi-square test, and where necessary p-values less than 0.05 and greater than 0.05 were regarded as significant and non-significant respectively.
RESULTS
During the study period, 46 children aged two days and 15 years (mean 3 months ± 2.1) had colostomy and they were 34 males and 12 females with male/female ratio 2.8:1. Congenital anomaly was the main indication and accounted for 40 (87%) patients, while acquired anomaly accounted for 6 (13%) patients. An extremely significant statistical difference was observed when complications and mortality were compared among the two groups (P<0.0001). Of the congenital anomaly, anorectal malformation accounted for 22 (48%) patients and Hirschsrung’s disease 18 (39%) patients, were the only indications. Morbidity and mortality were higher among anorectal anomaly than Hirschsrung’s disease with an observed significant statistical difference (P=0.0021). There were four patients with intracardiac, two Down’s syndrome and one malrotation associated with anorectal anomaly, while Hirschsrung’s disease was isolated anomaly.
Children who had anorectal anomaly were younger and they presented between two days and three months (mean 1.5 months ± 0.45) compared with those who had Hirschsprung’s disease that presented between one month and 15 years (mean 4.8 months ± 3.25). This was due to delayed diagnosis because Hirschsrung’s disease patients had normally situated anus and there was no absolute constipation in many. The duration patients had the colostomy was also shorter for anorectal anomaly, one and 12 months (mean 9.1 months ± 2.12) than Hirschsrung’s disease three months and 8 years (1.3 years ± 3.12) because the bowel in Hirschsrung’s disease were grossly dilated which made early pull through difficult and some defaulted from follow-up and represented in surgical outpatients’ clinic eight years after colostomy was created.
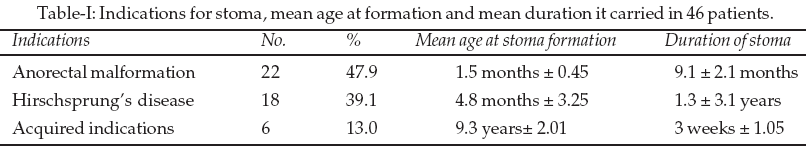
Among the acquired indications, rectovaginal fistulae sequel to obstructed labour in a 13-year-old and 15-year-old girls accounted for two (4.4%) and that complicating retroviral infection accounted for one (2.2%), perineal injury in two (4.4%) and left colonic injury one (2.2%). Also, those that had colostomy for acquired indications were older, aged 5 and 15 years (9.3 years± 2.01), and also had the colostomy for a shorter period, two and six weeks (3 weeks ± 1.05). All the children had temporary colostomy. Twenty-eight (60.9%) had transverse loop, four (8.7%) transverse double barrel, two (4.4%) transverse Devine, one (2.2%) sigmoid loop, two (4.4%) sigmoid double barrel, six (13.1%) sigmoid Devine, two (4.4%) Hartmann’s and one (2.2%) had caecostomy.
Because transverse loop colostomy is one of the fastest to create, it was mainly used in this study. This is because most of the patients presented late in haemodynamic instability and could not withstand long period under general anaesthesia. The construction of transverse loop colostomy was fast and hence minimized prolong exposure to general anaesthesia. Hirschsprung’s disease patients who presented in stable clinical state were given leveling colostomy which was usually a divided sigmoid colostomy. All the types of colostomy functioned satisfactorily in this review and they had similar complications. In all, skin excoriation was recorded in 39 (84.8%) patients and this was managed with skin protective paste such as zinc oxide cream or petroleum jelly when zinc oxide cream was not available. The skin lesions ranged from minor hyperaemia (in 12 patients) to deep excoriation (in 7 patients) which necessitated earlier closure. They all, however, healed when the colostomy was closed. The colostomy prolapsed in 15 (32.6%) patients. This was very disturbing because all the parents/caregivers were worried despite adequate counselling. The prolapse, persistent odour 21 (45.7%), and deep skin excoriations made 10 (21.7%) parents/caregivers accept the colostomy poorly. This led to four patients defaulting during follow-up but all represented on seeing children who had colostomy that did well after closure.
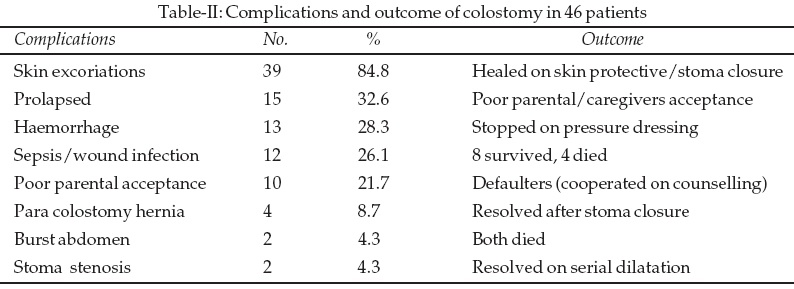
Stoma edge bleeding was recorded post operatively in 13 (28.3%) patients, whereas pressure dressing controlled 11 cases, two were problematic because the children had bleeding diathesis which was co-managed successfully with paediatricians. Wound infection and neonatal sepsis with paralytic ileus were recorded in 12 (26.1%) patients and it accounted for the morbidity and mortality recorded. As a result, four of the patients died from overwhelming sepsis and two died after developing burst abdomen due to the protracted ileus and wound infection, with a total mortality of six (13.1%) recorded during the period. After wound infection had healed among those that survived, two (4.4%) patients developed stoma stenosis which responded to serial dilatation with anal dilators. The para colostomy hernia recorded in four (8.7%) patients had no sequel and all resolved after closure of the colostomy.
DISCUSSION
The creation of colostomy is a common procedure performed in children, especially in this subregion.
2,3 Male preponderance with male/female ratio 2.8:1 recorded in this study tally with earlier reports.2-4 Congenital anomaly was a major indication for colostomy in children compared with acquired pathology and this is in conformity with literatures.1-7 Colostomy created in children for congenital indications had more associated morbidity and mortality with an observed extremely significant statistical difference compared with the acquired group (P<0.0001).5,8 All the children in this study had temporary colostomy. This is because the indications were correctable lesions which allowed closure of the colostomy after definitive surgery.1,4,6,11 Wound infection and overwhelming sepsis were the main causes of morbidity and mortality in this review and reports from previous studies.1,11 Sepsis culminating in multiple organ failure was responsible for the 6 (13%) mortality in this study which was similar to earlier studies in this subregion.2-4,9-11Anorectal anomaly accounted for more indications for colostomy in this study. This is at variance with earlier reports
2,4 in this subregion that reported Hirschsrung’s disease as a more common indication. Also, children with anorectal anomaly presented at a younger age than those who had Hirschsrung’s disease because of absent or abnormally situated anus and absolute constipation recorded. The absolute intestinal obstruction in many babies with anorectal anomaly necessitated colostomy being created for children that were haemodynamically unstable with resultant higher morbidity and mortality (P=0.0021).6-11 This was compounded by associated cardiac anomaly recorded among only babies with anorectal anomaly which constituted a high anaesthetic risk. The absence of a normal anus, however, made them keep appointment, came earlier for definitive repair and had earlier closure of colostomy.2-4,10,11Skin excoriations continued to pose a major challenge to colostomy creation and accounted for 39 (84.8%) children having this complication in this study.
1-3 This has been attributed to the constant maceration of the skin, allergic reaction to gut contents, fungal infection of the macerated skin as well as enzymatic digestion of the macerated skin and exposed subcutaneous tissues.1,2 Stoma bags are not readily available and even when available their use in children was very difficult in most rural communities with poor hygiene. Although skin protective cream was enough to prevent deep excoriation in many patients, a large proportion had deep excoriations which necessitated earlier closure. This was because of the difficulty in controlling deep excoriation after it had established.6-8 The non availability of stoma bags and difficulty with its use in children, particularly among rural dwellers made skin excoriation inevitable complication.10,11 The underprivileged mothers were taught to use napkins and clean the site regularly with water and this gave good results.2,4,11Methods
aimed at reducing colostomy prolapse which was the second most common complication in this study have been described in the literatures.1-12 Controlling the prolapse was very difficult and no method adopted was satisfactory as was also reported by other workers.11-13 The prolapse, persistent odour and deep skin excoriations made 10 (21.7%) parents/ caregivers accept the colostomy poorly. This is similar to earlier reports3,10,11 in this subregion but at variance with reports from more enlightened society.6-8,12 Even though this led to 4 patients defaulting during follow-up they represented in stable clinical state on seeing children who had colostomy but did well after it was closed. Further cooperation was obtained by demonstrating to parents, other children who once had colostomy and did well after closure during counselling sessions as was earlier reported.3Post operative haemorrhage from colostomy site was controlled by pressure dressing and this was not severe enough to require blood transfusion except in two cases that had bleeding diatheses as also reported previously.
1,2 On the other hand, colostomy closure has also been reported to be associated with complications, although none was recorded in this study.5,6,13,14 The timing of colostomy closure was influenced by financial constraint, skin excoriation, prolapse, parents/caregivers compliance and clinical state of the patients.5,13-15 Generally, those who had colostomy for acquired indications were closed earlier, followed by anorectal anomaly and Hirschsprung’s disease. All the patients had intraperitoneal closure with good results, although reports16,17 by those who use extraperitoneal and laparoscopic closure are also encouraging.In conclusion, the morbidity and mortality recorded in this study were due mainly to underlying pathologies complicated by sepsis and not colostomy related; hence colostomy was a common procedure performed in children during the period. The lack of facilities and manpower needed to perform definitive procedures which required exposure to long period of general anaesthesia in unstable children, made colostomy play important role in the management of these children. Adequate preoperative counselling of parents/caregivers, good stoma care and early stoma closure gave encouraging results. Colostomy still has much to offer in emerging paediatric surgery units in resource poor regions.
REFERENCES
1. Gauderer MWL. Stomas of the small and large intestine. In: O’Neill JA, Rowe MI, Grosfeld JI, Fonkalsrud EW, Coran GA eds: Pediatric Surgery 5th Edition Philadelphia: Mosby Year Book Inc 1998;2:1349-58.
2. Uba AF, Chirdan LB. Colostomy complication in children. Ann Afr Med 2003;2:9-12.
3. Ameh EA, Mshelbwala PM, Sabiu L, Chirdan LB. Colostomy in children an evaluation of acceptance among mothers and caregivers in a developing country. S Afr J Surg 2006;44:138-9.
4. Adotey JM. Colostomy- the Port Harcourt experience. West Afr J Med 1998;17:179-83.
5. Wong RW, Rappaport WD, Witzke DB, Putnam CW, Hunter GC. Factors influencing the safety of colostomy closure in the elderly. J Surg Res 1994;57:289-92.
6. Chandramouli B, Srinivasan K, Jagdish S, Ananth- akrishnan N. Morbidity and mortality of colostomy and its closure in children. J Pediatr Surg 2004;39:596-9.
7. Mollit DL, Malangoni MA, Ballantine TV, Grosfeld JL. Colostomy complications in children. An analysis of 146 cases. Arch Surg 1980;115:455-8.
8. Cigdem MK, Onen A, Duran H, Ozturk H, Otcu S. The mechanical complications of colostomy in infants and children: analysis of 473 cases of a single centre. Pediatr Surg Int 2006;22:671-6.
9. Al-Salem AH, Grant C, Khawaja S. Colostomy complications in infants and children. Int Surg 1992;77:164-6.
10. Nmadu PT. Complications of colostomy closure in Zaria, Nigeria: A report of 70 cases. Cent Afr J Med 1990;36:287-91.
11. Nmadu PT. Colostomy: indications, complications and management: the Zaria experience. Trop Doct 1992;22:128-9.
12. James TKL. Proximal end transverse colostomy in children: a method to avoid colostomy prolapse in Hirschsprung’s disease. Dis Colon Rectum 1983;26:221-2.
13. Garber HI, Morris DM, Eisenstat TE, Coker DD, Annous MO. Factors influencing the morbidity of colostomy closure. Dis Colon Rectum 1982;25:464-70.
14. Pachter HL, Hoballah JJ, Corcoran TA, Hofstetter SR. The morbidity and financial impact of colostomy closure in trauma patients. J Trauma 1990;30:1510-13.
15. Sola JE, Bender JS, Buchman TG. Morbidity and timing of colostomy closure in trauma patients. Injury 1993;24:438-40.
16. Das S. Extraperitoneal closure of colostomy in children. J Indian Med Assoc 1991;89:253-5.
17. Rosen MJ, Cobb WS, Kercher KW, Sing RF, Heniford BT. Laparoscopic restoration of intestinal continuity after Hartmann’s procedure. Am J Surg 2005;189:670-4.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk