|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
The causes of death among patients with
tuberculosis in Khuzestan, Iran
Seyed Mohammad Alavi1, Nejad Salami2
ABSTRACT
Objective: To assess the cause of death in tuberculosis patients.
Methodology: It is a retrospective descriptive study conducted in Khuzestan province in the south west of Iran, from 2002 to March 2006. Medical records of tuberculosis patients over the 5-year period were reviewed and death data were analyzed. Inclusion criteria were documented TB, diagnosed based on National Tuberculosis Program (NTP), extracted data were analyzed in SPSS11.5 system and by descriptive statistics.
Results: One hundred and twenty five deaths (3.15%) with mean age of 48.96+/- 10.03 years were detected. The frequency rate for cigarette smoking, diabetes, chronic renal failure, MDR-TB, imprisonment, HIV infection and injection drug usage were 31.2%,16%, 6.4%,6.4%,22.4%,13.6% and 22.4%, respectively. Eighty four deaths (67.2%) were directly attributed to tuberculosis, among them overwhelming TB disease, haemoptysia, and MDR-TB accounted as the cause of death in 77.4%, 13.1%, 9.5% and 6.4% respectively. Forty one (32.8%) deaths were due to other medical problems, which included AIDS, cardiovascular diseases, bacterial super infection and cancers i.e. 21.9%, 19.5%, 17.1% and 12.2% respectively.
Conclusions: This study showed that overwhelming TB disease, haemoptysis, cardiovascular diseases, bacterial super infection and cancers are the main cause of death. Smoking, imprisonment, injection drug usage and diabetes are frequent risk factors for TB mortality.
KEYWORDS: Cause of death, Tuberculosis mortality, Risk factor.
Source of Funding:
Joundishapour Infectious Diseases and Tropical Medicine Research Center.Pak J Med Sci April - June 2008 (Part-I) Vol. 24 No. 2 217-220
1. Dr. Seyed Mohammad Alavi, MD
Assistant Professor of Medical College,
2. Dr. Nejad Salami, MD
Infectious Disease Ward, Razi Hospital,
1-2: Joundishapour University of Medical Sciences,
Khuzestan Health Center
Joundishapour Infectious Diseases and
Tropical Medicine Research Center,
Ahwaz – Iran.
Correspondence
Dr Seyed Mohammad Alavi,
No: 52, West 11 Avenue,
Kianabad, Ahwaz,
Iran
Email:alavi1329dr@yahoo.com
* Received foe Publication: May 31, 2007
* Revision received: December 6, 2007
* Revision Accepted: December 25, 2007
INTRODUCTION
One third of the world population is infected with M.tuberculosis. Eight million new cases and two million deaths are reported annually worldwide, in which 12% are due to AIDS/HIV.
1 Twenty five percent (25%) of TB deaths in adults in developing countries are preventable.2 TB is one of the 10 leading cause of deaths in developing countries.3 Iran with 17.5% prevalence and 27 per 100 000 population incidence rate is 17Th country in the ranking worldwide.4,5M.tuberculosis after HIV is the most common killer infectious agent in adults worldwide.
1 Mortality rate of TB is high, if untreated, 50% will die, 25% recurs and 25% chronic.2 Although directly observed treatment (DOT) strategy has decreased TB mortality, but, in developing countries, TB is yet the leading cause of preventable deaths.2,4 The causes of death in tuberculosis patients are divided in two groups. The first directly attributed to TB and in the second, the patients die of complicating medical problems unrelated to tuberculosis, such as cardiovascular diseases, diabetes mellitus, cancers, bacterial super infection and severe drug toxicity.6-9 Previous studies have reported that pulmonary failure due to extensive pulmonary involvement and haemoptysis were the main causes of TB death.9The aim of this study was to assess and determine the main causes of death and risk factors of tuberculosis patients in the area of study. Meaning of these risk factors and reducing them will decrease mortality rate from tuberculosis.
METHODOLOGY
In a retrospective study, medical records of all notified tuberculosis cases over the five year period (2002-2006) in Khuzestan province Health Center (south west of Iran) were reviewed and death data were analyzed. Inclusion criteria were documented TB, diagnosed based on National Tuberculosis Program (NTP).
10 Cases with at least two sputum smear positive for acid fast bacillus (SSP-AFB) or, a chest radiography (C-X ray) suggestive of tuberculosis plus one SSP-AFB or, sputum culture positive for M.tuberculosis and one SSP-AFB were defined as smear positive pulmonary tuberculosis (PTB+).Cases with clinical finding suggestive of TB plus three sputum smear negative AFB (3SSN-AFB) after two weeks of antibiotic therapy plus C-X-ray (suggestive TB) were defined as smear negative pulmonary tuberculosis (PTB-). Other diagnostic criteria were cerebro spinal fluid (CSF) analysis for TB meningitis and CT-scan and microbial study for milliary or extra pulmonary tuberculosis (EPTB).
Demographic characteristics, medical history, imprisonment, HIV serology status, drug addiction, underlying diseases, drug side effects and other medical problems during anti TB treatment were taken from their medical files in Razi hospital and KHC. Finally data were analyzed in SPSS11.5 system and by chi square test.
In this study according to NPT, tuberculosis patients are followed up during treatment course (at least 6 months) and 12 months after completion of treatment (month 3, 6 and 12). TB mortality was recorded over six month’s period of treatment.
RESULTS
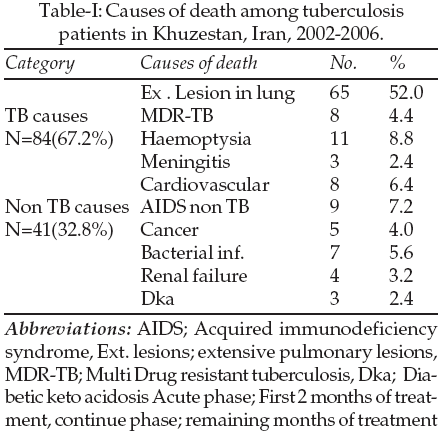
A total of 3960 cases who started anti TB treatment were enrolled in this study, among whom 1521 (38.4%) were female and 2439 (61.6%) were male. One hundred twenty five cases (3.15%) including 44(35.2%) female and 81(64.8%) male with mean age of 48.96 year and SD of10.03 died during treatment. Mortality rate in female and male were 2.8% and 3.3%, respectively. Ninety two (73.6%) died during the first two months of therapy. Eighty four deaths (67.2%) were directly attributed to tuberculosis. Overwhelming TB disease was the cause of death in 65 case (77.4%), among them majority died due to respiratory failure. Eleven cases (13.1%) died of massive haemoptysia. Eight patients (9.5%) died due to multi drug resistant (MDR-TB). Three(3.6%) died of TB meningitis and miliary TB and two (2.4) due to haemothorax. Forty one (32.8%) died due to medical problems unrelated to TB; nine patients (21.9%) from AIDS, eight patients (19.5%) due to cardiovascular diseases, seven patients (17.1%) died as a result of bacterial super infection and sepsis, five patients (12.2%) due to cancers, four (9.8%) due to COPD, four (9.8%) deaths were the result of renal failure, three (7.3%) due to diabetic ketoacidosis and one patients died due to drug induced hepatitis. Other results are shown in Tables-I & II.
DISCUSSION
This study showed that mortality rate of tuberculosis in Khuzestan was 3.15%, (2.8% in females and 3.3% in males). This finding is consistent with previously reported by Kourbatova and et al
11 but higher than reported by Xie.12 TB mortality differs in each country because of TB epidemiological status, TB risk factors and co morbid diseases. This finding also reflects that TB management in Khuzestan like other developing countries is far from developed countries. Despite employing DOTS strategy since 1997 in the area of study,10 mortality rate of TB is yet not acceptable and current TB surveillance must be improved. Frequent risk factors in our study were cigarette smoking, imprisonment, injection drug usage, diabetes, AIDS and chronic renal failure which were consistent with some previous studies.6-9,11-13 In contrast to other studies HIV infection and old age were not frequent risk factors for death in this study. In the present study majority of deaths occurred early in the course of treatment, with 73.6% dying within the first two months of therapy that reflects delayed time between diagnoses and starting of treatment (more than 2 months). These finding suggest that active case finding can reduce TB mortality rate by earlier detection and treatment.

This study also showed that the deaths among TB patients were not only directly related to TB itself but, also were caused due to co morbid conditions, such as cardiovascular, uncontrolled diabetes mellitus, cancers and bacterial super infection. This finding is similar to other studies.6-9, 11-13
In comparison with other reports, non TB cause of death in this study (32.8%) is lower than those conducted in low-incidence developed countries (Kabashi, Japan and Xie, Canada)
8,9,12 with the rate of 58% to 69% but, is consistent with the same –incidence country.6 Kuba et al showed that 31% of tuberculosis patients died directly due to tuberculosis and 69% died from underlying diseases unrelated to TB. Pulmonary failure due to extensive pulmonary involvement, haemoptysis and TB meningitis were the main causes of TB related death and cancers & bacterial pneumonia were the main causes of unrelated to TB.9 Mathew and his colleague reported that TB mortality rate was 9.6% and 75% of tuberculosis patients died of TB while 25% of deaths were unrelated to TB and risk factors for death were: older age, previous anti TB treatment, MDR-TB and alcoholism.6 In the present study we found that fibrotic and cavitary lesions in the lungs predispose patients to superimposed bacterial infection such as severe and life threatening pneumonia and sepsis. This finding is similar to other reports conducted by Kuba, et al and Tocque et al (17.1% vs. 20%).9,13 Early detection and appropriate use of anti microbial drugs can save the life of TB patients. We believe that TB worsen this co morbid disease and place them at increased risk of dying. By adopting a systematic approach to screening and treatment this medical problem will decrease TB mortality rate. Majority of TB related death in this study was due to extended and severe damaged lesions in the lung (diagnosed by lung CT-scan or chest-X-ray) consistent with the works of Kuba,9 Tocque13 and Kourbatova.11 This finding reflects that diagnosis and treatment of TB are made at the end stage phase on account of delay in diagnosis by nearly two months as mentioned previously). Improvement of TB surveillance in Khuzestan and even throughout Iran need to be emphasized. MDR-TB was also associated with death in this study. This was unlikely to be the consequence of delayed diagnosis, but rather, reflects poor prognosis and outcome on second line anti tuberculosis therapy.1,6This study also showed that IDU and AIDS were associated with increased risk of death. High prevalence of drug addiction among Iranian prisoners and the fact that majority of HIV/AIDS in Iran (more than 60%) are due to needle sharing among drug addicts.
14-16 We feel that active surveillance HIV/AIDS in prisons especially in addict holding units is most likely to reduce TB mortality rate.CONCLUSIONS
Despite employing DOTS strategy since 1997 in Khuzestan,
10 there is high mortality rate of TB which is not acceptable. This study showed that overwhelming TB disease, haemoptysis, cardiovascular diseases, bacterial super infection and cancers are the main cause of death. Moreover smoking, imprisonment, injection drug usage and diabetes are frequent risk factors for TB mortality.Recommendation: To decrease TB mortality we recommend that:-
1. Current TB surveillance should be revised.
2. Active case finding for earlier detection and treatment of TB should be employed.
1. Active surveillance HIV/AIDS in prisons especially in addict holding units.
2. Adopting a systematic approach to screening and treatment of co morbid diseases
ACKNOWLEDGEMENTS
We wish to thank CDC staff of Khuzestan Health Center particularly Dr. Tarahhomi for his collaboration. We also thank Infectious Diseases Ward personnel and medical files archivist of Razi hospital for their valuable cooperation.
Conflicts of interest: This study was approved and funded by Infectious Disease and Tropical Medicine Research Center of Joundishapour University of Medical Sciences and there is no conflict of interest.
REFERENCES
1. Mandell GL, Bennett JE, Dolin R. Principles and practice of infectious diseases.6th ed. Elsevier Churchill Livingstone, Philadelphia 2005;2852-3.
2. World Health Organization. TB/HIV: A Clinical Manual,2004.
3. World Health Organization. The ten leading causes of deaths by broad income group 2005 Projections Fact sheet N° 310 / February 2007.
4. World Health Organization; Global Tuberculosis Control: WHO Report 2000. WHO, Geneva: WHO/CDS/TB/2000;275.
5. Iranian Center of Control and Prevention of Diseases. Epidemiological situation of tuberculosis in Iran, Ministry of health, 2002.
6. Mathew TA, Ovsyanikova TN, Shin SS, Gelmanova I, Balbuena DA, Atwood S, et al. Causes of death during tuberculosis treatment in Tomsk Oblast, Russia Int J Tuberc Lung Dis 2006;10(8):857-63.
7. Davis CE Jr, Carpenter JL, McAllister CK, Matthews J, Bush BA, Ognibene AJ. Tuberculosis. Cause of death in antibiotic era. Chest 1985;88(5):726-9.
8. Kobashi Y, Matsushima T, Okimoto N, Hara Y Clinical evaluation of the cause of death in patients with active pulmonary tuberculosis Kekkaku. 2002;77(12):771-5.
9. Kuba M, Nakasone K, Miyagi S, Kyan K, Shinzato T, Kohagura N, et al. Clinical evaluation on causes of death in patients with active pulmonary tuberculosis Kekkaku. 1996;71(4):293-301.
10. Mirhaghani L, Nasehi M. National Tuberculosis Program in Iran, Ministry of health, Nashre Seda 2002;15-20.
11. Kourbatova EV, Borodulin BE, Borodulina EA, del Rio C, Blumberg HM, Leonard MK Jr. Risk factors for mortality among adult patients with newly diagnosed tuberculosis in Samara, Russia. Int J Tuberc Lung Dis 2006;10(11):1224-30.
12. Xie HJ, Enarson DA, Chao CW, Allen EA, Grzybowski S. Deaths in tuberculosis patients in British Columbia, 1980-1984. Tuber Lung Dis 1992;73(2):77-82.
13. Tocque K, Convrey RP, Bellis MA, Beeching NJ, Davies PD. Elevated mortality following diagnosis with a treatable disease: Tuberculosis Int J Tuberc Lung Dis 2005;9(7):797-802.
14. Razzaghi EM, Movaghar AR, Green TC, Khoshnood K. A qualitative study of injecting drug users in Tehran, Iran. Harm Reduct J 2006;18:3:12.
15. Vazirian M, Nassirimanesh B, Zamani S, Ono-Kihara M, Kihara M, Ravari SM, et al. Needle and syringe sharing practices of injecting drug users participating in an outreach HIV prevention program in Tehran, Iran: a cross-sectional study. Harm Reduct J 2005;7:2:19.
16. Gezairy HA. WHO eastern Mediterranean region report. Geneca: WHO, 2000.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk