|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
Short Communication |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
The epidemiologic profile of pancreatic cancer
and management outcome in Lagos, Nigeria
Onyekwere CA1, Ojukwu JC2
ABSTRACT
Objectives: Pancreatic cancer is a common gastrointestinal malignancy worldwide with incidence almost equal to mortality. The aim was to study the pattern, management and outcome of pancreatic cancer in Lagos, Nigeria from 2005-2007.
Methodology: All histologically – proven cases of pancreatic cancer seen in two hospitals (University teaching and a private facility) in Lagos, Nigeria during the study period were recruited noting their bio data, clinical presentation, treatment and outcome.
Results: The patients age range was 40-86 years.with a mean (SD) of 64 years (10.9) and M: F ratio of 15:12. The common clinical features were weight loss, jaundice and epigastric pain in a few. Abdominal ultrasonography was useful in the diagnosis but histological confirmation was at laparoscopy during which palliative shunt was done for relief of distressing pruritic symptoms. One patient had celiac axis block for distressing pain. The histological types were adenocarcinoma (96%) and anaplastic tumour (4%). All came in advanced stage where palliation was the only option. The mean survival period was 6 months while the 1-year survival is 4%.
Conclusion: The outcome of pancreatic cancer is still very poor and efforts at improving early diagnosis remain the only hope.
KEY WORDS: Pancreatic Cancer, Epidemiology, Nigeria.
Pak J Med Sci April - June 2008 (Part-I) Vol. 24 No. 2 340-343
1. Onyekwere CA, MBBS, FMCP
Dept. of Medicine,
Lagos state University Teaching Hospital Ikeja,
Lagos - Nigeria.
2. Ojukwu JC, MD, FRCS
Advanced Videoscopic and
Laparoscopic Surgical Centre (AVLSC).
Lekki Phase One,
Victoria Island,
Lagos – Nigeria.
Correspondence
Onyekwere C.A
P.O BOX 203 Satelitte Town,
Lagos – Nigeria.
Email: ifymobi@yahoo.com
* Received for Publication: October 3, 2007
* Accepted: January 15, 2008
INTRODUCTION
Pancreatic cancer is the second most common gastrointestinal cancer after colorectal cancer (CRC) and the fourth commonest cancer in males after lung cancer, prostrate cancer and CRC in the western countries. In females it is ranked 5th after lung cancer, breast cancer, cervical/ovarian cancer and CRC. Mortality from pancreatic cancer is almost identical to incidence with median survival of about six months.
1Its incidence is said to be higher in blacks, male gender and older age. It is associated with smoking, diet high in fat and protein with little carbohydrate and exposure to certain pesticides and chemicals related to gasoline. It is said to be familial in up to 10% and may be associated with type 2 diabetes mellitus and chronic pancreatitis.
2 The pathological varieties described include ductal cell adenocarcinoma (90%), Islet cell carcinomas (5%) and cyst adenocarcinoma.3The clinical manifestation is determined by tumour site; cancers of the body and tail cause epigastric pain, anorexia and weight loss. They are often disseminated to other sites like regional nodes, peritoneum causing ascites, liver and the lungs at the time of diagnosis. Cancers of the head cause jaundice at an earlier stage, which may be associated with pruritus. Multifocal tumours are common. New onset diabetes mellitus have been described in 10-20% of them.
4Pre-operative diagnosis and staging have traditionally relied on; transabdominal ultrasonograhy and computed tomography (CT) scan with guided fine needle aspiration. endoscopic retrograde cholangiogram with brushings (ERCP), Endoscopic ultrasound with fine needle aspiration (EUS-FNA) and laparoscopic surgical biopsy.
5 A staging laparoscopy is minimally invasive and delineates inoperability; a palliative bypass could conveniently be performed at the same time. Tumor markers are usually unhelpful but serial rise in CA 19-9 indicates aggressively.Treatment of pancreatic cancer remains challenging and mostly palliative.
6 Pancreatic resection along with duodenectomy (pancreatoduodenectomy) (Whipples procedure) combined with adjuvant chemotherapy offers the best chance of survival but should only be considered if patient is fit, tumour size <3cm with no metastasis. Operative mortality is up to 5% even in expert hands with substantial post-operative morbidity.7 Unfortunately many patients do not meet these criteria as up to 80% have unresectable tumour with metastasis at diagnosis. The available options6,8,9 for these advanced pancreatic cancer includes:-Use of chemotherapeutic agents: 5 fluorouracil or Capacetabine with 1year survival of 2%, Gemcitabine alone one year survival 18%, and Erlotinib with Gemcitabine one year survival of 24%.
- Palliation of jaundice by
* ERCP stent insertion by experienced endoscopists though with risk of bleeding, infection and blockage.
* Percutanuous drainage alone or in combination with ERCP with similar risk.
* Open surgical or more recently laparosopic cholecystojejunostomy or choledochoje- junostomy with a loop or roux-en-y for billiary diversion and rarely gastrojejunostomy for gastric outlet obstruction.
- Palliation of pain using opiate analgesic or laparoscopic celiac block.
- Improvement in quality of life with cholestyramine to reduce itching from obstructive jaundice.
Reports of the pattern of pancreatic cancer exist from the Western countries, Asia, Far East and South America
10-13 with hardly any from Nigeria. A recent report14 however indicates that it is the fourth commonest gastrointestinal malignancy in Lagos, Nigeria. This report sets out to describe the pattern of pancreatic cancer in Lagos, Nigeria as seen by a review of 27 cases. The aim of this study was documentation of the pattern of pancreatic cancer in Lagos Nigeria as seen by a review of 27 cases.METHODOLOGY
All patients that presented to the Gastroenterology unit, Dept of Medicine of Lasuth and the AVLSC Medical Centre Lekki Phase One, Victoria Island Lagos with features of pancreatic cancer and were subsequently confirmed histologically from January 2005 to September 2007 were included into the study.( specify cut off dates for the study) Their clinical records was reviewed and the following data extracted from them; bio data, clinical presentation, risk factor if any, biochemical profile and tumour marker CA 19-9. The findings on imaging (abdominal USS/CT) as well as during laparoscopy with staging will be noted. The histological types and treatment (radical surgery, palliatic surgery and chemotherapy) as well as outcome and survival will be documented.
RESULTS
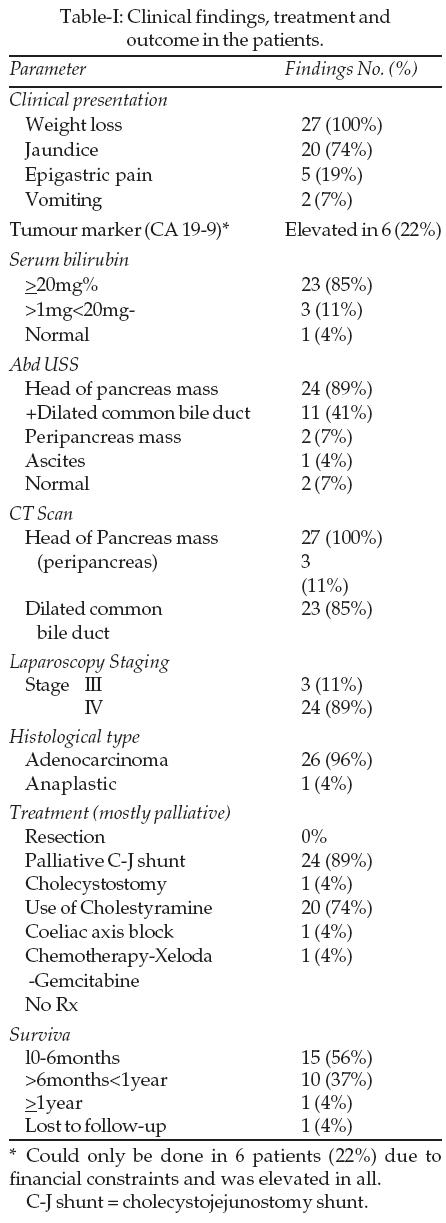
Our review shows a total of twenty-seven patients of age range 40-86 years with a mean (SD) of 64.1 years (10.9) and M: F ratio of 15:12 seen over a three year period (2004-2007). The commonest clinical features were jaundice (21) and weight loss (27). Two patients had epigastric pain while six were already known to be diabetic. The biochemical and imaging findings as well as treatment offered is as shown in Table-I. The one year survival is 4% while the mean survival (SD) is 6.5 (5.06) months.
DISCUSSION
Our patient size of 27 within a 3-year period may appear rather low considering previous reports
1,14 indicating cancer of pancreas as the second commonest gastrointestinal malignancy. The possible explanation for this may be the referral pattern as most of the patients were referred because of distressing pruritic symptoms. Only one patient was referred because of severe epigastric pain. The other reason is the fact that only those with histological confirmation were included. Most patients have a coagulopathy and are not fit for surgical procedures, the other diagnostic options including minimally invasive laparoscopy as in this study or ERCP is yet to be widely available in Lagos and Nigeria at large. The older age and male preponderance as well as association with diabetes mellitus (22%) seen in this review are in keeping with previous reports.2Serum bilirubin and abdominal ultrasonography were found to be useful in the diagnosis and should be done on every patient presenting with jaundice, epigastric pain and weight loss since they are non invasive, readily available and inexpensive. However the most valuable tool for pre-operative diagnosis was abdominal CT. Tissue diagnosis was only possible following laparosopy during which staging and shunt procedures were done for those requiring palliation of their obstructive hepatopathy.
All patients in this study presented in advanced or late stages (III and IV) with palliation being the only option. Improvement in quality of life was achieved modestly with cholestyramine and palliative minimally invasive laparoscopic cholecystojejunostomy. The few who opted for chemotherapy had minimal improvement in one year survival. Our one-year survival (4%) is similar to that from other studies.
6,9CONCLUSION
Early diagnosis remains the key to treatment with abdominal ultrasonography and CT scan being most readily available in this environment. Minimally invasive diagnostic laparoscopy confirms the stage; enables tissue diagnosis and palliative billiary bypass can also be performed at the same procedure. A celiac block if necessary with phenol could also be performed. The prohibitive cost and side effects of Gemcitabine and Erlotinib are also an important factor.
REFERENCES
1. Kloppel G, Hruban RH, Longnecker DS, Adler G. Ductal Adenocarcinoma of the pancreas. World Health Organization classification of tumours: pathology and genetics of tumours of the digestive system. IARC Press 2000.
2. Kemery G. Pancreatic cancer. Epidemiology and pathology. Practical Gastroenterology 2006;30(4):22-32.
3. Capelle C, Solcia E, Kloppel G, Hruban RH. Serous cystic neoplasms of the pancreas. World Health Organization classification of tumours. Pathology and genetics of tumours of the digestive system. IARC Press Lyon 2000.
4. Steer M. Clinical manifestation, diagnosis and surgical staging of exocrine pancreatic cancer. Up To Date. 2005.
5. Victor K, Chen MD, Miguel R, Arguedas MD. A cost minimization analysis of alternative strategies in diagnosing pancreatic cancer. Amer J Gastroenterology 2004;99(11):2223-34.
6. Van Laethem, Marechal R. Emerging drugs for the treatment of pancreatic cancer. Expert Opin Emerg Drugs 2007;12(2):301-11.
7. Fernandez-del CC, Jimenez RE, Steer M. Surgery in the treatment of pancreatic cancer. Up To Date. 2005.
8. Fletcher DR, Jones RM. Laparoscopic cholecystjejunostomy as palliation for obstructive jaundice in inoperable carcinoma of pancreas. Surgical Endoscopy 1992;6(3)147-9.
9. Peter S K, Francois G EL K, Michael LG. Metastatic Pancreatic cancer: emerging strategies in Chemotherapy and palliative care. The Oncologist 2003;8(1):18-34.
10. Svrcek M, Lesurtel M, Lewin M, Afchain P, Fabre M, Scoazec JY, etal. Acinar cell carcinoma of the pancreas with predominant intraductal growth; report of a case. Gastroent Clin Biol 2007;31(5):543-6.
11. Kitagami H, Kondo S, Hirano S, Kawakami H. Acinar cell carcinoma of the pancreas; clinical analysis of 115 patients from pancreatic cancer registry of Japan Pancreas society. Pancreas 2007;35(1):42-6.
12. Yua D, Yu W, Ren XB, Pan WD, Zhang L. Characterization and accuracy of serous cystadenomas and mucinous neoplasms of the Pancreas with multi-slice helical computed tomography. Zhongguo Yi Xue Ke Xue Yuan Xue Bao 2007;29(2):232-7.
13. Souza JJ, Michado MC, Cunha JE, Jukemura J. Analysis of pancreatic Adenocarcinoma tumour staging and resection according to previous body mass index and diabetes duration. Pancreatology 2007;7(2-3):187-93.
14. Abdulkareem F. Pattern of malignant gastrointestinal tumours in Lagos and Shagamu, South-west Nigeria. West Africa Postgrad Med J (Accepted for Publication October 2007).
