|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
Short Communication |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
Short Communication |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
Comparison of pre and post surgical caudal
block in reducing stress responses in children
M. Seyedhejazi1
ABSTRACT
Objective: Surgical stress stimulates the release of catecholamine and cortisol. Both of which have anti-insulin action resulting in an increase of plasma glucose concentration. The most common regional block in pediatric age group is caudal epidural analgesia.
The aim of this study was to compare the stress response following pre and post surgical caudal block.
Methodology: After approval by our local ethics committee and written parental consent 70 children between two and seven years of age scheduled for elective lower abdominal procedures were enrolled in this study. Anesthesia was induced with fentanyl 1µg/kg, midazolam 0.03mg/kg, propofol 3mg/kg, LMA was inserted, maintenance was with halothane 1-1.5%, N2O 3 lit/min, O2 3 lit/min. Halothane concentration was decreased to 0.6% in children who received pre surgical caudal block (20 minutes after block). Children in group-A received pre surgical caudal block with 0.25% bupivacain 1ml/kg, those in group B received post surgical caudal block with same dosage and concentration.
Results: Demographic data were similar. Plasma glucose concentration were decreased during the course of this study in Group A, (P=0.045). However, in Group B the plasma glucose level increase 15 min after beginning of surgery (P=0.001). The hemodynamic changes with in group A was less than group B (P<0.05).
Conclusions: In children, pre but not post surgical caudal block attenuates the stress response associated with lower abdominal surgery.
KEY WORDS: Caudal block, Blood sugar, Stress response, Pediatric.
Pak J Med Sci April - June 2008 (Part-I) Vol. 24 No. 2 344-347
1. Dr. M. Seyedhejazi,
Assistant Professor,
Department of Anesthesiology,
Tabriz University of Medical Sciences,
Tabriz – Iran.
Correspondence
Dr. M. Seyedhejazi,
E-mail: seidhejazie@yahoo.com
* Received for Publication: December 10, 2007
* Accepted: January 31, 2008
INTRODUCTION
During the past two decades, pediatric pain has received considerable attention, and reliable age-related pain scales have been developed to evaluate the severity of pain and the efficacy of its treatment. Surgery generates a neuroendocrine stress response in neonates, infants and children, resulting in undesirable alterations of the metabolic state and immune function. Epidural anesthesia diminishes or even suppresses this stress response and is well tolerated in children.
1Because young children lack the ability to communicate their analgesic needs and are unable to use a patient-controlled analgesia device, regional anesthesia techniques are preferred for relief of postoperative pain. These techniques can also be used instead of general anesthesia when preexisting anatomic or physiologic alterations increase the risk of general anesthesia.
2The most popular regional anesthesia technique in pediatric patient is the caudal epidural block, which is relatively easy to perform.
1-3 It can be performed prior to surgery to be used in combination with general anesthesia, performed after surgery to be used for postoperative analgesia, or used instead of general anesthesia for low abdominal and lower extremity procedures.2,4Previous reports have demonstrated that blood levels of epinephrine (E) and norepinephrine (NE) were decreased by caudal epidural analgesia, using local anesthetics alone, caused by afferent neural blockade.
5 Surgical stress stimulates the release of cathecholamines and cortisol both of which have anti-insulin action resulting in an increase of plasma glucose concentrations.6The present prospective, randomized study was designed to determine if preoperative caudal epidural block, compared with postoperative caudal epidural block, decreases stress response after lower abdominal surgery in children.
METHODOLOGY
After approval by our local ethics committee and written parental consent, 70 pediatric patients, ASA physical status one between two and seven years of age, all undergoing elective herniorrhaphy, hydrocele, undessended testis, circumcision, were randomly (with randomly computed blocks) assigned to two groups. Group A= preoperative caudal block and Group B= post operative caudal block.
Patients were excluded from the study if they had: a failed block, hemoglobin of less than 11g%, episodes of intraoperative hypothermia (less than 350c), hypoxia (Spo2 of less than 95%), Hypercarbia (Co2 more than 50mmHg) or hypothermia (with or without shivering) in the recovery room.
Anesthesia was induced with fentanyl 1µg/kg, midazolam 0.03mg/kg, propofol 3mg/kg, laryngeal mask airway was inserted. All children were breathing a fresh gas flow through a mapleson D-circuit. Manual assisted ventilation was performed to keep end-tidal CO2 between 35-45mmHg. Maintenance of anesthesia was with halothane 1-1.5%, N2O 3 lit/min, O2 3lit/min. Halothane concentration was decreased to 0.6% in children who received pre surgical caudal block (20 minutes after block).
In the Group A after the child was asleep, and before surgery, the child was placed in the left lateral position and a 23 or 21 gauge needle inserted in to the caudal space through the sacrococcygeal membrane, by using an aseptic and non touch technique. When the aspiration test was negative 1ml/kg of bupivacaine 0.25% was injected. 15 – 20 minutes after caudal analgesia the surgical incision was done. Group B patients received post surgical caudal block (just after surgery and under general anesthesia) with the same method.
In both groups’ blood samples with drawn at, G0: Two days before surgery G1: Baseline (immediately after anesthesia induction) G2: 15 minutes after surgical incision G3: 20 minutes after completion of surgery. Blood samples with drawn from separate IV line that was closed with heparin lock.
Heart rate(HR), non invasive systolic and diastolic blood pressure, Spo2, Etco2, were measured before anesthesia, after anesthesia induction, after caudal analgesia (group A) and then every five minutes in both groups.
Patients were fasted for a minimum of six hours from solid food and milk and two hours from clear fluid. All children were adequately hydrated by using ringer solution at a rate of 10ml/kg in the first hour using an infusion pump.
Statistical analysis for a comparison between the four phases (G0, G1, G2 and G3) of the study in each group was performed by using the analysis of variance test for repeated measurement. The unpaired student’s t-test was used when each phase (G0, G1, G2 and G3) was compared between the two groups. The equality of variances was performed by using the levene’s test. Statistical significance is assumed when the P. value were < 0.05.
RESULTS
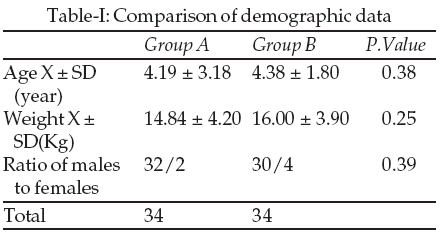
Seventy children undergoing lower abdominal surgery were enrolled in this study and randomly assigned to two groups. There were no significant differences in the demographic data so two groups were comparable (Table-I). Two children were excluded from the study because of block failure (aspiration test was positive in one cases, the other one had subcutaneous injection by incorrect needle placement). The type of surgery was 69.5% inguinal hernia, 8.8% undessended testis and remaining were circumcision.
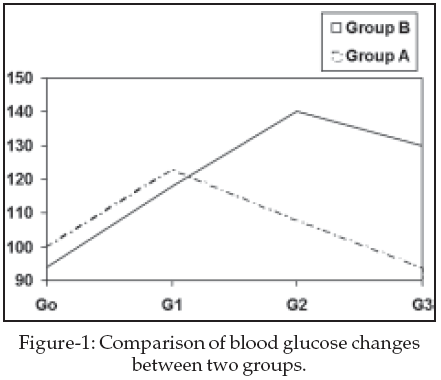
None of the patients had signs of hypoglycemia before induction of anesthesia. Plasma glucose concentration were decreased during the course of this study in Group A, (P=0.045). However, in Group B the plasma glucose level increase 15 minutes after surgical incision (P=0.001). But it decrease 20 minutes after completion of surgery (P=0.001). The mean plasma glucose concentration in Group A was lower than in Group B during and after surgery (P=0.003) (Fig-1).
The increase in systolic blood pressure and diastolic blood pressure weren’t significant with in Group A (P=0.47, P=0.19). The increase in systolic blood pressure was significant (P=0.03) but the changes of diastolic blood pressure wasn’t significant (P=0.12) with in Group B. According to P. value there were significant differences between two groups in the mean of systolic blood pressure (P=0.001) and diastolic blood pressure (P=0.02).
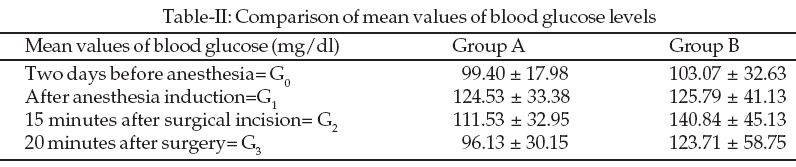
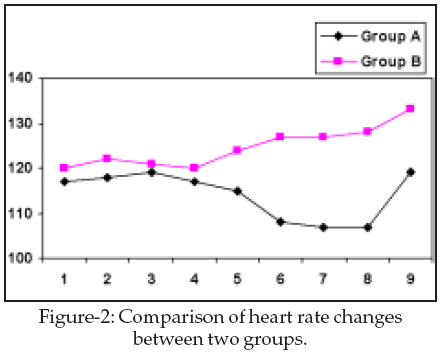
The increase in heart rate wasn’t significant within Group A (P=0.63), but it was significant in Group B (P=0.001). There were significant differences between two groups in the mean of heart rate P=0.001(Fig-2).
DISCUSSION
Our results showed that the increase in plasma glucose concentration due to surgical stress was prevented by preoperative caudal epidural analgesia. Plasma glucose levels were low during and after surgery performed with caudal analgesia, though they were high in the Group B.
Reduction of the stress response is highly dependent on the surgical site and the analgesic technique used. Caudal epidural analgesia / anesthesia inhibit the stress response, particularly during surgery in the lower part of the body in a pediatric population.
7,8 It has been demonstrated that the addition of caudal block to general anesthesia significantly reduces the neurohormonal response in children undergoing ilioinguinal herniorrhaphy.5 One study assessed the effects of caudal block on plasma cortisol, prolactin, insulin and glucose concentration during and after surgery. It indicated that caudal anesthesia suppresses the metabolic and endocrine responses to stress associated with lower abdominal surgery in children.9The surgical stress increase catecholamine and cortisol that both has anti insulin action that lead to hyperglycemia. So it is suspected that surgical incision causes increased in the blood glucose.
5 In our study in Group B, after surgical incision blood glucose increase significantly but in Group A the G2 decreased compared with G1(P=0.045). The caudal blocks before surgery decrease hemodynamic changes during surgery.7 In this study the systolic, diastolic blood pressure and heart rate changes within Group A weren’t significant(P<0.05).Panels and Hasnaui in 750 lower abdominal surgeries with caudal analgesia reported that successful block is common in children below seven years of age and they had only seven cases of block failure.
6 In this study we had two block failure that were excluded from study. In our study for Group A patients we decreased halothane concentration 20 minutes after surgical incision (the homodynamic remain stable) that showed successful block in all of patients except two.Khali SN and coworkers compared pre surgical caudal block with intravenous narcotics and post surgical caudal block and pointed out that pre surgical caudal analgesia attenuates the stress response of anesthesia and surgery and decrease postoperative narcotic use while narcotics prolong PACU and discharge times. Other study results show that in children undergoing inguinal hernia repair, pain control with a preoperative caudal block as compared to intra operative intravenous fentanyl significantly reduces the incidence of emergence agitation and pain scores following sevoflurane anesthesia.
10Pain is the main determinant of the early catecholamine response to surgery in the lower extremity,
9 however, pain measurement in children is difficult and unreliable. Each of the methods of rating pain has its limitations, particularly in the nonverbal children.10 Stress response hormone levels can therefore be used as an objective method to assess the analgesic efficacy of local anesthetics injected into the extradural space before infra umbilical or lower extremity surgery in both adult and pediatric populations.3REFERENCES
1. Miller RD, Fleisher LA, Johns RA, Savarese JJ, Weiener-Kronish JP, Young WL. Miller’s Anesthesia, USA, Elsevier, 2005;1732-4.
2. Litman RS. Pediatric Anesthesia the Requisites in Anesthesiology, USA, Mosby, 2004;160-5.
3. Tobias JD. Therapeutic application of regional anesthesia. Paediatr Anaesth 2002;12:272-7.
4. Zaglaniczny K, Aker J. Clinical Guide to Pediatric Anesthesia. USA. Saunders Company,1999;359-412.
5. Gaitini LA, Somri M, Vaida SJ, Yanovski B, Mogilner G, Sabo E, et al. Dose the addition of fentanyl to bupivacaine in caudal epidural block have an effect on the plasma level of catecholamines in children? Anesth Analg 2000;90:1029-33.
6. Russell SCS, Doyle E. Recent advaces: Paediatric anaesthsesia. BMJ 1997;314:201.
7. Motoyama EK, Davis PJ. SMITH’s Anesthesia for infants and children. Seventh Edition. USA, Mosby, 2006;468-74.
8. Tuncer S, Yosunkaya A, Ruhily R. Effect of caudal block on stress responses in children. Pediatr Int 2004;46:53-9.
9. Khalil SN, Hanna E, Farag A, Govindaraj R, Vije H, Kee S. Pre surgical caudal block attenuates stress response in children. Middle East J Anesthesiol 2005;18(2):391-400.
10. Aouad MT, Kanazi GE, Siddik-sayyid SM, Gerges FJ, Rizk LB, Baraka AS. Preoperative caudal block prevents emergence of agitation in children following sevoflurane anesthesia. Acta Anaesthesiol Scand 2005;49(3):300-4.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk