|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
CASE REPORT |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
CASE REPORT |
||||
|
- |
||||
|
Volume 24 |
April - June 2008 (Part-I) |
Number 2 |
||
|
|
||||
|
|
||||
Dealing with markedly elevated false positive
d-dimer by sequential testing with two d-dimer assays
Khawaja Afzal Ammar1, Molly Shapiro2
ABSTRACT
False positive D-dimers are common & lead to an expensive confirmatory work-up. The approach of a highly sensitive assay for screening followed by a highly specific assay for confirmation, commonly used in diagnosing AIDS and Lyme disease, have not been applied to D-dimer testing. We describe a case of a 32-year old female with pleuritic chest pain and a D-dimer of >2000�g/l. Although negative chest CT and leg ultrasound for thromboembolism were performed, persistent pleuritic chest pain mandated further work-up. We used a confirmatory D-dimer assay with much higher specificity to declare the first test false positive. Such a negative confirmatory test can save further follow-up, work-up, and anxiety on both the parts of patient and physician, and should be considered in diagnostic algorithms of venous thromboembolism.
KEY WORDS:
False positive D-dimer, Venous thromboembolism.Abbreviations and Acronyms:
AIDS = Acquired Immune Deficiency Syndrome,CT = Computerized Tomography, DVT = Deep Venous Thrombosis,ECG = Electrocardiogram,
ELISA = Enzyme Linked ImmunoSorbent Assay, GI = GastroIntestinal, LA = Latex Agglutination ,
PE = Pulmonary Embolism, US = Ultrasound
Pak J Med Sci April - June 2008 (Part-I) Vol. 24 No. 2 321-323
1. Khawaja Afzal Ammar, MD
2. Molly Shapiro, RN, MSN-MBA, PhD
Division of Cardiology,
Department of Internal Medicine,
Mayo Clinic Rochester, MN
Department of Internal Medicine,
Olmsted Medical Center, Rochester, MN, USA.
Correspondence
Khawaja Afzal Ammar, MD,
Assistant Professor of Medicine,
C/o Tammy Burns, Gonda 5-468,
Division of Cardiovascular Diseases, Mayo Clinic,
200 First Street SW, Rochester, MN 55905.
Email: ammar.khawaja@mayo.edu
* Received for Publication: November 13, 2007
* Accepted: March 6, 2008
INTRODUCTION
In clinical practice, D-dimer may be the first diagnostic screening test in a protocol for symptomatic outpatients with suspected thromboembolism.
1 D-dimer assay sensitivity and negative predictive value is dependent on the discriminate level, assay method, kit and instrument. D-dimer levels are not only elevated in venous thromboembolic diseases, but also in other life threatening conditions including occult malignancy as well as non life threatening conditions including recent surgery, infection, hemorrhage, trauma, liver disease, pregnancy and anemia.2,3 If results are associated with low specificities, additional diagnostic testing is recommended.4 When combined with other non-invasive diagnostic tests, a the clinical utility of D-dimer lies in negative predictive value of greater than 90%.5The various D-dimer assays in use offer different mixes of sensitivity and specificity. Advantages of ELISA are higher sensitivities but disadvantages to clinical utility are expense and length of processing time.
3 The advantages of latex agglutination (LA) assays are rapid results and low cost but disadvantages are false negatives, subjective results, and reagent variability. Red blood cell agglutination assays have shown to be quick and affordable but sensitivity range variability makes them less accurate.6 While the major clinical utility of D-dimer is its high negative predictive value, a markedly positive D-dimer test, creates a clinical obligation to continue the workup beyond the usual paradigm of ruling out venous thromboembolism. The following case illustrates this issue.We obtained permission from the Institutional Review Board of Olmsted Medical Center.
CASE REPORT
A 32-year old non-smoking female presented with pleuritic chest pain and dyspnea that started after traveling in a car for two hours. The only abnormal laboratory finding was D-dimer >2000�g/l when normal is <301�g/ml. Routine hematological indices and other laboratory tests were normal.
The patient was actively menstruating while having been on birth control pills for 9 months. Vital signs were normal except a temperature of 100 degrees Fahrenheit. The physical exam was normal except for the hint of a systolic click. The patient was adopted with an unknown family history. Her chest x-ray was negative and ECG showed a longstanding left axis deviation. Complete blood counts, troponin, chemistries were normal. US for DVT was negative to lower extremities bilaterally. Spiral CT showed no pulmonary emboli. Due to markedly elevated D-dimer in a fairly suspicious clinical setting, she was hospitalized for further monitoring and evaluation. Echocardiogram showed trivial mitral valve regurgitation. UGI x-ray was normal. Repeated D-dimer assays were >2000. The patient remained clinically stable, was discharged, and followed as an outpatient. Her chest pain resolved but her D-dimer stayed above 2000. False positivity was considered. A confirmatory STAGO-LIA� quantitative was ordered and was negative. Serial Pacific Hemostasis� D-dimers were twice negative which corroborated the clinical diagnosis and patient course. The last three negatives were considered true results. She was followed for 18 months without sequelae.
DISCUSSION
This case illustrates the negative impact of a markedly positive D-dimer test on evaluation of a patient with pleuritic chest pain. A high D-dimer in the right clinical setting merits chest CT and bilateral leg US. If the D-dimer is alarmingly high, then the specificity of quantitative assays reaches >90%.
6 In this case with marked elevation of D-dimer of >2000 (implying>90% specificity) and pleuritic chest pain, a physician is obligated to pursue further work-up to determine cause of elevation, even after the ultrasound and CT are negative for venous thromboembolism. There are strong psychological and legal imperatives to prove false positivity in such clinical scenarios. Analogies would include screening HIV infection with ELISA but if positive, confirming it with a more specific test, i.e. Western blot. Another similar clinical paradigm would be a middle aged male with classic anginal chest pain whose stress ECG is normal. Such patients will be further tested with sestamibi or angiogram, in order to explain the angina. We suggest that a sensitive D-dimer assay be used as a screening tool. If results are markedly elevated such, as in this case, protocols should include a confirmatory assay that is more specific.Once false positivity is confirmed, anxiety is alleviated for both patient and physician. Most clinical algorithms would suggest workup with ultrasound and CT scan of chest to rule out venous thromboembolism, if such a severe elevation is seen in a person with some predisposing factors for DVT as a prolonged car ride by our patient who also was on oral contraceptives. Once venous thromboembolism is ruled out, the urgency to diagnose the cause of elevated D-dimer is resolved. While the Emergency Room physician is more concerned with diagnosing diseases that are life threatening in the short term, the general internist who eventually assumes the care of the patient is responsible for ruling out diseases that are life or limb threatening in the long term. The current algorithms fail to address this clinical dilemma.
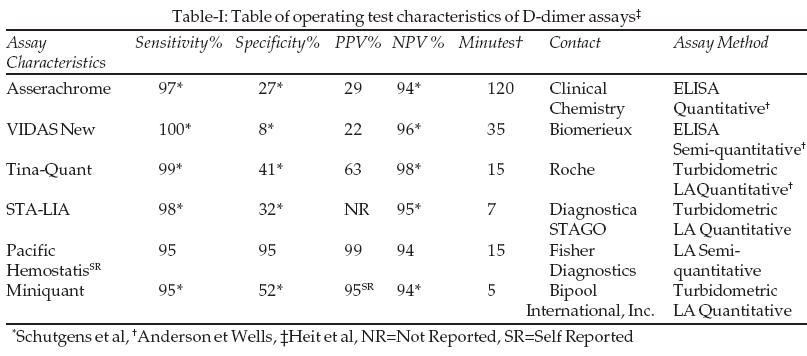
8 Since other causes of D-dimer elevation include malignancy, instead of launching an exhaustive workup for malignancy, doing a more specific D-dimer test to confirm the false positivity of the test, in a non-urgent manner (via a reference laboratory if not available locally, over next day or two), may be more prudent and cost effective.The sensitivity and specificity of different D-dimer tests are listed in the table. In selecting a more specific assay, many methods such as ELISA and whole blood assays are more accurate clinically than LA but they are time consuming and not suitable for emergency use.
4 While the strategy of using a more specific D-dimer assay may address the issue of dealing with a markedly positive D-dimer, to see if it is true positive or false positive, it obviously cannot be used to deal with other limitations of D-dimer like false negativity, which is rare.3,7While current algorithms revolve around optimal strategies of using clinical history, D-dimer and expensive imaging in order to diagnose venous thromboembolism, they do not address the strategy to further evaluate patients with markedly positive D-dimer after venous thromboembolism is excluded.
4,8 This case makes the point that it may be more cost-effective and efficient to follow-up an abnormal sensitive D-dimer assay with another more specific D-dimer assay. If the specific d-dimer assay is negative then further work-up is unnecessary and it also saves both the patient and the physician from further worry. We already follow this logic in clinical practice when testing for AIDS or Lyme disease (ELISA followed by Western Blot) or coronary artery disease in a chest pain patient (a positive ECG stress test is followed by a stress echo, which has higher specificity). Borrowing this concept for D-dimer may confer similar benefits.ACKNOWLEDGEMENT
We like to thank Ms. Uroos Raza, MS for her excellent manuscript preparation and editing skills
REFERENCES
1. Dempfle CE. Use of D-dimer assays in the diagnosis of venous thrombosis. Semin Thromb Hemost 2000;26(6):631-41.
2. Anderson DR, Wells PS. D-dimer for the diagnosis of venous thromboembolism. Curr Opin Hematol 2000;(7):269-301.
3. Frost SD, Brotman DJ, Michota FA. Rational use of D-dimer measurement to exclude acute venous thromboembolic disease. Mayo Clin Proc. 2003;78:1385-91.
4. Schutgens RG, Haas FL. The usefulness of five D-dimer assays in the exclusion of deep vein thrombosis. J Thromb Haemost 2003;1:976-81.
5. Perrier A, Desmarais S. Non-invasive diagnosis of venous thromboembolism in outpatient. Lancet 1999;353:190-5.
6. Kelly J, Rudd A, Lewis RR, Hunt BJ. Plasma D-dimers in the diagnosis of venous thromboembolism. Arch Intern Med 2002;162:747-56.
7. Freyberger G, Trillaud H, Labrouche S. D-dimer strategy in thrombosis exclusion-a gold standard study in 100 patients suspected of deep venous thrombosis or pulmonary embolism: 8 DD methods compared. Thromb Haemost 1998;79:32-7.
8. Wells PS. Integrated strategies for the diagnosis of venous thromboembolism. J Thromb Haemost. 2007;5:Suppl 1:41-50.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk