|
 |
|
Published
by : PROFESSIONAL MEDICAL PUBLICATIONS |
|
ISSN 1681-715X |
|
|
|
|
|
- |
|
ORIGINAL
ARTICLE |
|
- |
|
Volume 25 |
April
- June 2009 (Part-I) |
Number 2 |
|
|
|
Bony complications of chronic sinusitis
M. Masud Ul Haq1, Shahid Hussain2
ABSTRACT
Objectives: To study bony complications of
sinonasal disease and its varied manifestations.
Methodology: In this five year retrospective study,
cases with bony complications from 2003 to 2007 were collected and their
records evaluated. Twenty cases were identified with bony complications.
Results: Maxilla was most common bone affected.
Five patients were diagnosed as having acute osteomyelitis (35%); an equal
number were diagnosed as having chronic osteomyelitis of which one had a
fistula on the cheek and one had fistula due to tuberculosis. Odontogenic
infections and chronic sinusitis each gave rise to two cases with
osteomyelitis of the palate and maxilla. Chronic sinusitis was the main cause
of frontal bone osteomyelitis in two cases, one of which had a discharging
fistula in left frontoethmoid region displacing eye. Fungal sinusitis led to
destruction of lamina papyracea. Acute osteomyelitis responded to antibiotics.
Conclusions: Polymicrobial infection is common,
antibiotics are indicated initially. Surgery is considered when an abscess is
revealed by CT and if it deteriorates clinically. Results suggest that FESS is
effective for diagnosis and treatment of complications but can be combined
with conventional surgery which is effective in management of refractory
sinusitis.
KEY WORDS: Sinusitis, Bony complications, Osteomyelitis,
Antibiotics, FESS, Caldwell-Luc.
Pak J Med Sci April - June 2009
Vol. 25 No. 2 308-312
How to cite this article:
Masud-Ul-Haq M, Hussain S. Bony complications of chronic sinusitis. Pak J
Med Sci 2009;25(2):308-312.
1. M. Masud Ul Haq, FCPS,
Associate Professor of ENT
2. Shahid Hussain, FCPS,
Assistant Professor of ENT
Department of ENT,
Lahore Medical & Dental College,
Ghurki Trust Teaching Hospital,
Jallo More,
Lahore, Pakistan
Correspondence
Dr. M. Masud Ul Haq,
Department of ENT,
Lahore Medical & Dental College,
Ghurki Trust Teaching Hospital,
Jallo More,
Lahore, Pakistan
Email: entpak@yahoo.com
* Received for Publication: July 1, 2008
* Revision Received: July 8, 2008
* Revision Accepted: January 26, 2009
INTRODUCTION
In developing countries, sinusitis is under treated.
Morbidity and mortality has altered over the decade due to newer antibiotics.
To compound the problems, these are prescribed by clinician, also self
prescribed by patients and that too in low therapeutic doses and withdrawn on
slight improvement. Maxillary is the commonest infected sinus. Exciting
factors may be polyps, neoplasia, ostial obstruction, debilitating illnesses.
Unilateral chronic maxillary sinusitis may be associated with foreign body in
the maxillary sinus.
1
Maxillary sinusitis due to dental causes is secondary to periodontal/periapical
infection2
and suppurative facial lesion may be a sign of dental infection.3
Complications arise due to spread through bony, vascular, perineural,
lymphatics and are orbital, intracranial and bony involvement leading to muco/pyococele,
osteomyelitis/osteitis and dental root infections.4
It is rare to see sinus discharging as open fistula on the face in modern
world of antibiotics and surgery.
With improvement in economic and social conditions and use
of antibiotics, we have enjoyed a decline in infections for several decades.
It is now seen that bony complications of sinusitis presentations form a
proportion of new cases, especially with diabetes and resurgence of fungal
disease and some cases of tuberculosis. Therefore, it is important that
clinicians are aware of bony complications and varied manifestations. We
report increased incidence of isolated complications, its strange
presentations and clinical manifestations over a five year period. History,
examination, pus culture sensitivity and radiology were main investigations.
Medical treatment was effective in acute cases. Surgery was opted in chronic
cases.
METHODOLOGY
In this retrospective study, cases with bony complications
from 2003 to 2007 were collected and their records evaluated. Twenty cases
were identified with bony complications at the department of otolaryngology
and head and neck surgery, Lahore Medical and Dental College allied hospitals.
Each patient underwent a detailed clinical examination and a battery of
investigations. Most patients were treated with antimicrobial therapy; others
required surgical intervention followed by extensive medical therapy. In
addition, diabetics were treated with anti-diabetics and one with ATT
respectively.
RESULTS
Maxillary sinus, frontal sinus, ethmoids and sphenoid sinus
were involved, in descending order of frequency; maxilla was the most commonly
affected. Five patients were diagnosed as having acute osteomyelitis (35%); an
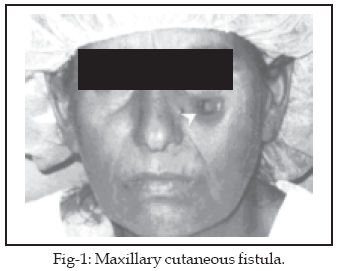
equal number were diagnosed as having chronic osteomyelitis of which one had a
fistula on the cheek (Fig-1) and one had fistula due to tuberculosis
(Fig-2ab).
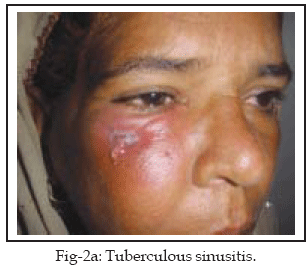
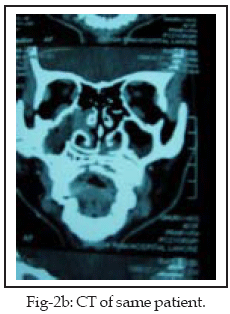
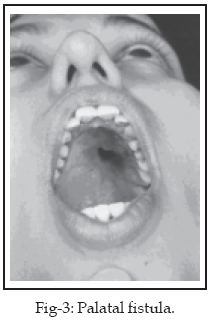
Odontogenic infections and chronic sinusitis each gave rise
to osteomyelitis in two cases (10%) of the patients with osteomyelitis of the
palate and maxilla combined of which one case had a fistula in the hard palate
(Fig-3). Chronic sinusitis was the main cause of frontal bone osteomyelitis in
two cases (10%), one of which had a discharging fistula in left frontal bone
displacing the eye ball.
Fungal sinusitis led to destruction of lamina papyracea and
displacement of eye ball (Fig-4). Acute osteomyelitis leading to orbital
cellulites responded to antibiotics. Corticosteroids were helpful in initial
abortion of acute symptoms especially in fungal diseases. Sequestrectomy was
carried out in all chronic cases but in cases of bony complications more
radical surgery was performed including FESS and conventional reconstruction.

DISCUSSION
Internet search revealed less than 50 articles on bony
complications of sinusitis. In sinusitis; strept-staph, H.influenzae are early
organisms while Pseudomonas aeruginosa, Moraxella catarrhails are late
invaders.
5
Infections due to Pseudomonas aeruginosa are difficult to treat6
and has the ability in sinusitis, at least in the presence of surgical
intervention to involve bone at a distance from the site of primary infection
in the absence of intervening mucosal disease.7
Recent investigations of chronic sinusitis, recalcitrant to traditional
medical and surgical therapy, indicate the gram-negative bacteria are
frequently involved commonly pseudomonas aeruginosa.8
Comparing it with our cases, we had the problem of multiple drug resistant
staph aureus and pseudomonas aeruginosa along with involvement in the form of
removal of sequestrate, mucosa and granulation tissue. Till the infection is
confined to sinuses it is called sinusitis. The spread of infection beyond the
bony walls leads to complications. Maxillary sinusitis results in redness,
swelling of cheek and eye lids, leading to subperiosteal abscess, bony
necrosis/sequestrate and fistula. Endopthalmos and midface depression may
occur in sinusitis. This process may be result of chronic maxillary
hypoventilation with atelectasis of antrum secondary to chronic negative
pressure.9
Chronic maxillary sinusitis can have different clinical
presentations. In our cases it was unusual bony complications, the patients
initially had localized infections and unethical surgical or medical
interventions, all contributed to the development of fistula draining
externally or invading deeply, a rare clinical event in the modern era. CT is
modality of choice for evaluating extent of disease and presence of focal
mucosal thickening should prompt clinical and radiological assessment.
3
Plain radiography and dental advise were undertaken at first instance in our
cases, although CT would have been ideal, but was not possible due to
financial constraints in all cases. Odontogenic infections and chronic
sinusitis each gave rise to osteomyelitis in 3 of 10 cases.
Almost 30% of the patients with osteomyelitis of the
maxilla, chronic sinusitis was the main cause of frontal bone osteomyelitis in
all 20 cases, tuberculosis 10 of 15 cases; 67%.
10
If otolaryngologist maintains a high index of suspicion, an early diagnosis
can be made with simple investigations. Successful outcome depends upon
appropriate chemotherapy and timely surgical intervention when necessary.11
Patients with tuberculosis of head and neck must be investigated to exclude
pulmonary or systemic disease.12
Rare localization of mucocoeles in maxillary sinus can be
explained with width of maxillary ostia, infections of local anatomical
structures should be operated with classic surgery.
13
Mucormycosis is saprophytic
organism which can become pathogenic in specific conditions, particularly in
patients with diabetes mellitus.14
Pott’s puffy tumor is associated with intracranial infection, early diagnosis
can be obtained by CT, treatment is surgery and antibiotics against mixed
pathogens.15
Pott’s puffy tumor has been reported in only 21 pediatric cases in the
literature. A high degree of suspicion with neurosurgical intervention and
appropriate antibiotics result in favorable outcomes.16
We treated our patient with a surgical abscess drainage
followed by prolonged use of antibiotics and achieved complete therapy. The
cellular and humoral elements of the immune system may be disrupted in
diabetic patients resulting in such atypical courses and complications of
infections. Evliyaođlu et al emphasized prompt diagnosis as intracranial
invasion may cause neurologic problems and importance of surgical intervention
tailored for individual lesion.
17
Orbital complications can cause orbital sepsis and cavernous sinus thrombosis,
the "close-lying" connections, as seductive they are, should not divert from
the rule: infrequent causes are infrequent and frequent causes are frequent.18
Ho et al identified pathogens in 39%, two common being Staph and Strept, 13%
had polymicrobial infection, 23 patients underwent sinus, orbital or
intracranial surgery, including all five patients in stage IV, three of six
patients in stage III, 13 of 35 patients in stage II, and two of 34 patients
in stage I.19
Administering corticosteroids as an adjunct to antibiotics
may accelerate the healing process in experimentally induced rhinosinusitis.
20
As regards surgery, Caldwell-Luc reduces oedema and inflammatory cells.21
Patients treated with Caldwell-Luc operation need reoperation in 7.3% cases.
While in FESS group 27% need reoperation.22
The post surgical effects of the removal of the maxillary sinus mucosa shows
marked increase in acute and chronic inflammation, granulation, fibrosis and
ulcerations.23
If there is no autogenous bone material available, the problem is to find a
suitable material for reconstruction, microtitanium mesh can be used for
reconstruction of the walls of maxillary sinus.24
Reconstruction is challenging, even more difficult problem when we compared
this situation to our cases. Some otolaryngologists believe that Caldwell-Luc
procedure should be used for unilateral chronic sinusitis, the results of this
series suggest that endoscopic sinus surgery is an effective procedure for the
diagnosis and treatment of unilateral chronic sinusitis.25
Complication rate was 4.4% in the Caldwell-Luc group and 2.6% in the FESS
group.26
CONCLUSION
Infected mucocoeles, expand to local anatomical structures,
should be operated with classic radical surgery. Fungal infection may have a
poor prognosis. The contribution of frozen section for diagnosis and
management should be adopted. Orbital complications due to sinusitis can cause
orbital sepsis and fistula formation. Polymicrobial infection is common,
broadspectrum antibiotics are indicated initially. Surgery should be
considered not only when an abscess is demonstrated by CT but also if clinical
deterioration occurs with adequate antibiotic treatment. Added steroids as an
adjunct to antibiotics accelerate the healing process. The results suggest
that FESS is an effective procedure for the diagnosis and treatment of bony
complications but can be combined with conventional surgery like Caldwell-Luc
which is effective in the management of refractory sinusitis after failed FESS
or antrostomy. It should remain in our armoury. Revision of the maxillary
sinus yields comparable outcomes to repeat Caldwell-Luc in patients with a
history of past failed surgery. Endoscopic revision is a good alternative for
surgical rehabilitation of bony complications.
REFERENCES
1. Tingsgaard PK, Larsen PL. Chronic unilateral maxillary
sinusitis caused by foreign bodies in the maxillary sinus. Ugeskr Laeger
1997;159:4402-4.
2. Connor SE, Chavda SV, Pahor AL. Computed tomography
evidence of dental restoration as aetiological factor for maxillary sinusitis.
J Laryngol Otol 2000;114:510-3.
3. Moir GC, Morris AM, MeClure IJ. Suppurating facial
lesions may be sign of dental infection JR Coll Surg Edinb 1996;41:416-8.
4. Lund VJ. The complications of sinusitis. In: Kerr A,
editor Scott Brown’s otolaryngology Vol 4. 6th ed. Oxf-ord:
Butterworth–Heinemann. 1997;4/13/1-4/13/1.
5. Farr RW, Ramadan H. Report of Pseudomonas aeruginosa
sinusitis in a patient with AIDS. WV Med J 1993;89:284-5.
6. Perloff JR, Gannon FH, Bolger WE, Montone KT. Bone
involvement in sinusitis: an apparent pathway for spread of disease.
Larygoscope 2000;110:2095-9.
7. Bolger WE, Leonard D, Dick EJ Jr, Stierna P. Gram
negative sinusitis: a bacteriological and histological study in rabbits. Am J
Rhinol 1997;11:15-25.
8. Blackwell KE, Goldbery RA, Calcaterra TC. Atelectasis fo
the maxillary sinus with enophthalmos and midface depression. Ann Otol Rhinol
Laryngol 1993;102:429-32.
9. Kesseler P, Hardt N. the use of micro-titanium mesh for
maxillary sinus wall reconstruction. J Craniomaxillofac Surg 1996;24:317-21.
10. Prasad KC, Prasad SC, Mouli N, Agarwal S. Osteomyelitis
in the head and neck. Acta Otolaryngol 2007;127(2):194-205.
11. Prasad KC, Sreedharan S, Chakravarthy Y, Prasad SC.
Tuberculosis in the head and neck: experience in India. J Laryngol Otol
2007;121(10):979-85.
12. Nalini B, Vinayak S. Tuberculosis in ear, nose, and
throat practice: its presentation and diagnosis. Am J Otolaryngol
2006;27(1):39-45.
13. Perić A, Baletić N, Vukomanović-Durdević B, Jović M,
Kozomara R. Mucocoele of the maxillary sinus. Vojnosanit Pregl
2007;64(5):361-4.
14. Ferchichi L, Chadli-Debbiche A, Koubâa W, Khayat O,
Labbčne N, Ben Gamra O, et al. Rhinocerebral mucormycosis in four diabetics. J
Mal Vasc 2006;31(2):85-7.
15. Mammen-Prasad E, Murillo JL, Titelbaum JA. Infectious
disease rounds: Pott’s puffy tumor with intracranial complications. N J Med
1992;89(7):537-9.
16. Bambakidis NC, Cohen AR. Intracranial complications of
frontal sinusitis in children: Pott’s puffy tumor revisited. Pediatr Neurosurg
2001;35(2):82-9.
17. Evliyaođlu C, Bademci G, Yucel E, Keskil S. Pott’s
puffy tumor of the vertex years after trauma in a diabetic patient: case
report. Neurocirugia Astur 2005;16(1):54-7.
18. Sturm V, Kordic H, Stürmer J, Landau K. Sinusitis and
ocular motility disorders. Klin Monatsbl Augenheilkd 2008;225(5):401-7.
19. Ho CF, Huang YC, Wang CJ, Chiu CH, Lin TY. Clinical
analysis of CT staged orbital cellulitis in children. J Microbiol Immunol
Infect 2007;40(6):518-24.
20. Sütbeyaz Y, Aktan B. Treatment of sinusitis with
steroids combination with antibiotics in experimentally induced rhinosinusitis.
Ann OtoRhinoLaryng 2008;117(5):389-94.
21. Markio – Makela M. Qvarnberg Y. Endoscopic sinus
surgery or Cardwell – Luc operation in the treatment of chronic and recurrent
sinusitis. Acta otolaryngol suppl 1997;529:177-80.
22. Melgarejo-Moreno PJ. Ribera Cortada I, Sarroca- Capell
E. Redical or partial maxillary sinus surgery: a dilemma today? An
experimental study. Rhinology 1996;34:110-13.
23. Bennninger MS, Sebek B. A Levine HL. Mucosal
regeneration of maxillary sinus after surgery. Otolaryngol Head Neck Surgery
1989;101:33-7.
24. Pandolfi PJ, Yavuzer R, Jackson IT. Three layer closure
of an oroantral – cutanous defect. Int J Oral Maxillary Surgery 2000;29:24-6.
25. Ishibashi T, Ishio K, Ichimura K, Mizuno M, Fukaya T.
Endoscopic sinus surgery for unilateral chronic sinusitis. Nippon Jibiinkoka
Gakkai Kaiho 1999;102(7):871-7.
26. Närkiö M, Qvarnberg Y. Endoscopic sinus surgery or Caldwell-Luc
operation in treatment of chronic and recurrent maxillary sinusitis. Acta
Otolaryngol Suppl 1997;529:177-80.
HOME
| SEARCH
| CURRENT
ISSUE | PAST
ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@





