|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 23 |
October - December 2007 (Part-II) |
Number 6 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 23 |
October - December 2007 (Part-II) |
Number 6 |
||
|
|
||||
|
|
||||
Evaluating causes of acute renal
failure in newborn infants
Gharehbaghi MM1, Peirovifar A MD2
ABSTRACT
Objective: Acute renal failure (ARF) is a common problem in admitted neonates in intensive care units. In most patients ARF accompanies with a predisposing factor such as sepsis, heart failure, perinatal asphyxia or prematurity. The objective of this study was to determine the causes and outcome of ARF in hospitalized newborn infants.
Methodology: In a descriptive cross sectional study we evaluated neonates with ARF who had been hospitalized in Tabriz Children Hospital from March 2004 to September 2005.
Results: There were 85 cases with diagnosed ARF in 3000 hospitalized neonates (2.83%).The male to female ratio in patients with ARF was 2.03:1. Most of involved patients were term (70.6%). The prevalence of renal, pre renal and post renal causes of ARF was 49.4%, 43.5% and 7.1% respectively. The most common predisposing factors for ARF in our study were surgery (43.5%), perinatal asphyxia (36.5%), sepsis (32.9%), respiratory distress syndrome (25.9%), heart failure (20%) and feeding problems (20%). All patients had more than one predisposing factor. Among admitted neonates with ARF mortality rate was 20% and it was significantly higher in patients with assisted ventilation and sepsis (P<0.05).
Conclusion: Early recognition of risk factors such as sepsis, perinatal asphyxia or, perioperative problems and rapid effective treatment of contributing conditions will reduce ARF in neonatal period.
KEY WORDS: Acute renal failure, Newborns, Predisposing factors.
Pak J Med Sci October - December 2007 (Part-II) Vol. 23 No. 6 877-880
1. Dr. MM Gharehbaghi,
Assistant Professor of Pediatrics & Neonatologist
2. Dr. A Peirovifar,
Associate Professor of Anesthesiology and
Intensive Care Medicine,
1,2: Department of Neonatology and
Intensive Care Unit,
Tabriz University of Medical Sciences,
Tabriz � Iran.
Correspondence
Dr. MM Gharehbaghi, MD,
E-mail: gharehbaghimm@yahoo.comv
* Received for Publication: May 31, 2007
* Revision Received: September 1, 2007
* Revision Accepted: September 3, 2007
INTRODUCTION
Acute renal failure (ARF) is defined as an acute deterioration in ability of the kidneys to maintain homeostasis of body fluids, electrolytes and is associated with acute decrease in the rate of glumerolar filtration (GFR) that leads to retention of wasted and toxic metabolic end products.
1,2 Neonatal ARF in first few days of life is suggested by a progressive increase in the infants plasma creatinine (Pcr) above normal values for age in the context of normal maternal renal function.2 Most reports estimate the incidence of ARF in hospitalized neonatal population to be 8-24%.1-7 Normal urine output is found in approximately one-third of neonates with ARF, although low urine output may occur in the absence of ARF. So, if urine output alone is used to assess renal function, ARF often will be either overlooked or over diagnosed.The incidence of intrinsic oliguric ARF in newborn infants admitted to the NICU ranges between 1-6% in retrospective studies and 6-8% in prospective studies.
2 The serum creatinine level is the simplest and most commonly used indicator of neonatal kidney function. The Pcr concentration immediately after birth reflects the maternal creatinine concentration. The Pcr level gradually decreases from 1.1mg/dl in term infants (1.3mg/dl in preterm infants) to a mean value of 0.4mg/dl within the first two weeks of life. In general each doubling of the serum creatinine level represents a 50% reduction in GFR.1,2 Although the criteria for ARF has varied between studies. ARF is characterized by decreased GFR and renal tubular function compared to normal values for post conceptional age. In term neonates diagnosis of ARF is strongly suggested by increased Pcr concentrations above 1.5mg/dl at least for 24-48 hours. Thus measuring GFR or following Pcr over time is required to diagnose ARF in a newborn infant.1,2,6,7 A rising of >0.3mg/dl/day in Pcr concentration has been proposed to improve the definition of ARF. The plasma concentration of creatinine can not reflect GFR in preterm infants during first days of life because of the effect of maternal creatinine load on creatinine concentration, tubular secretion of creatinine and its passive back diffusion across leaky tubules in extremely preterm infants. In these infants Pcr increases in the first 36 to 96 hours of life and then decreases gradually within the first two weeks.2,8A wide variety of predisposing factors such as sepsis, congenital heart diseases, metabolic disorders, perinatal asphyxia may cause neonatal renal failure. This study was performed to determine the causes and outcome of ARF in hospitalized newborn infants.
METHODOLOGY
The study was conducted in a referral neonatal intensive care unit of a teaching hospital in north east of Iran admitting out born neonates. Three thousand out born newborn infants that were referred and admitted in Tabriz Children Hospital form March 2004 to September 2005 were evaluated for presence of acute renal failure. ARF was defined as Pcr concentration >1.5mg/dl and blood urea nitrogen (BUN) >20mg/dl on two separate test at least 12 hours apart. Oliguria was defined as urine output less than 1ml/kg/h. During the 18 months of study period ARF was diagnosed in 85 patients. Data were collected through detailed questionnaires including demographic information of newborn infant, predisposing conditions, clinical course and outcome of ARF. Statistical analysis was performed using the statistical package for social sciences for windows (SPSS 12). P. Value < 0.05 considered statistically significant.
RESULTS
ARF was diagnosed in 2.83% (85 cases) of admitted newborn infants of which 57 cases (67%) were male and 28(33%) female. The male to female ratio was 2.03:1. Most of the patients with ARF were term (60 cases or 70.6%). Twenty two cases (25.9%) had prematurity and three cases (3.5%) were post term. Demographic characteristics and renal function tests of newborn infants are summarized in Table-I.
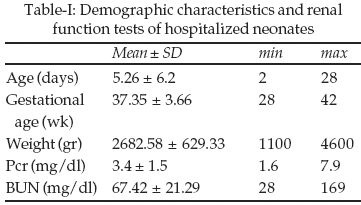
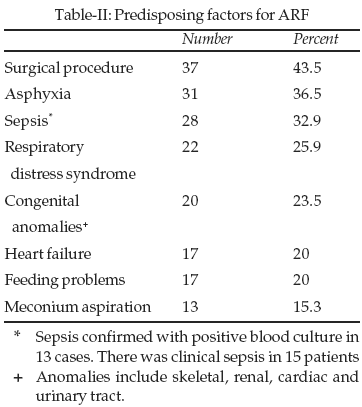
Oliguric ARF was found in 28 cases (32.8%) the prevalence of renal, prerenal and post renal types of ARF were 49.4%, 43.5% and 7.1% respectively. Predisposing factors for ARF are shown in Table-II. There were more than one predisposing factor in all patients.
Congenital renal anomalies were determined in six patients which include renal hypoplasia in three cases, polycystic kidney in two and multicystic dysplastic kidney in one patient. Obstructive uropathy was diagnosed in six patients, three cases of them had uretropelvic junction obstruction (upjo) and three neonates had posterior urethral value. Mortality among hospitalized neonates with ARF was 20% (17 cases). Male to female ratio of them was 7:10. Mortality in girls was significantly higher than boys (P=0.01). Patients with positive blood culture sepsis (P=0.003), clinical sepsis (P=0.01) and infants on assisted ventilation (P=0.002) had significantly higher mortality rate.
DISCUSSION
A wide variety of malformations or prenatal, perinatal and postnatal events may cause ARF. The commonest type of ARF in neonates is prerenal which is characterized by inadequate renal perfusion. Immediate and aggressive management of pre renal azotemia often leads to rapid improvement of renal function and urinary output.
1,2,7In this study, there was 43.5% pre renal azotemia which is less than renal type. This may be due to delayed hospitalization and management which may cause aggregation of renal injury. The most common intrinsic renal failure is acute tubular necrosis (ATN). Although ATN may be precipitated by a single event, its progression is multifactorial and involves vascular (hemodynamic), nephronal or cellular (metabolic) factors. Decreased renal blood flow may result from multiple mechanisms such as hypotension, heart failure and vasoconstriction.
1,2,7 In this study 2.83% of hospitalized neonates had ARF. As in other studies, the commonest predisposing factors for ARF in our patients were surgical procedures, Asphyxia and sepsis.4,6,7,9,10 The risk and severity of ARF increases with the severity of asphyxia. ARF associated with asphyxia is predominantly nonoliguric. Thus, if plasma creatinine is not monitored daily in severely asphyxiated neonate, renal failure will be easily missed. Oligoanuria in these infants may result from pre renal failure mediated by endothelin, intrinsic renal failure (ATN) or syndrome of inappropriate secretion of ADH (SIADH). In our study 31 newborn infants were moderately to severely asphyxiated and their ARF was non oliguric in 28 cases.The prevalence of ARF in boys is more than girls (male to female ratio 1.34-3.3:1) in several studies
7,11,12 and it was same in our patients. It assumes that predisposing factors of ARF such as sepsis and respiratory distress syndrome are more common in boys than girls. There were 28 (32.9%) oliguric renal failures in this study which is less than other reports.2,4 This may be due to high prevalence of asphyxia in our patients which predispose to nonoliguric ARF.Short term prognosis for neonatal ARF depends on general condition and status of all major organ systems of infant. In some studies, the mortality rate in oliguric ARF due to aquired conditions such as asphyxia and sepsis was 60% and there are reports of higher mortality rate in the presence of heart disease. The prognosis for nonoliguric renal failure or for prerenal failure is excellent, unless major arrhythmia secondary to hyperkalemia or multiorgan failure develops.
2,7 In this study, mortality in hospitalized neonates with ARF was 17 cases (20%) and the most important risk factors for mortality were sepsis and assisted ventilation. Mortality in girls was significantly higher than boys.RECOMMENDATIONS
The first step for prevention and treatment of neonatal ARF is to identify infants at high risk for renal failure and detection of oliguria immediately after predisposing events. For this infants urine output, vital signs, electrolytes and renal function should be followed serially. If urinary tract anomalies are suspected, a complete urologic work up should be considered. Early recognition of risk factors and rapid effective treatment of contributing conditions will reduce mortality and morbidity in neonatal ARF.
CONCLUSIONS
In high risk newborn infants with positive history of predisposing factors for ARF, correction of any abnormality of oxygenation, ventilation, cardiac output, blood pressure and early treatment of sepsis is needed for prevention and effective management of ARF.
REFERENCES
1. Vogt BA, Avner ED. The kidney and urinary tract. In: Fanaroff AA, Martin RJ. Neonatal-Perinatal Medicine: Diseases of Fetus and Newborn Infant. 8th ed. St, louis Mosby 2006;2:1666-70.
2. Avery GB, Flectcher MA, Mac Donald MG. Neonatology: Pathophysiology and management of newborn. 6th ed. Philadelphia. Lippincott Williams & Wilkins. 2005;2:1000-9.
3. Gouyon JB, Guignard JP. Management of acute renal failure in newborns. Pediatr Nephrol 2000;14(10-11):1037-44.
4. Agras PI, Tarcan A, Baskin E, Cengiz N, Gurakan B, Saatci U. Acute renal failure in neonatal period. Ren Fail 2004;26(3):305-9.
5. Stapleton FB, Jones DP, Green RS. Acute renal failure in neonates: Incidence, etiology and outcome. Pediatr Nephrol 1987;1(3):314-20.
6. Mathur NB, Agarwal Himanshu S, Arti M. Acute renal failure in neonatal sepsis. Indian J Pediatr 2006;73(6):499-502.
7. Airede A, Bello M, Weerasinghe HD. Acute renal failure in newborn: Incidence and outcome. J Pedaitr Child Health 1997;33(3):246-9.
8. Guzzolin L, Fanos V, Pinna B, Marzio M, Perin M, Tramontozzi P, et al. Postnatal renal function in pretern newborns: A role of disease, drugs and therapeutic interventions. Pediatr Nephrol 2006;21(7):931-8.
9. Mohan PV, Pai PM. Renal insult in asphyxia neonaturum. Indian Pediatrics 2000;37(10):1102-6.
10. Andreoli SP. Acute renal failure in the newborn. Semin Perionatol 2004;28(2):112-23.
11. Kandoth PW, Agarwal GJ, Dharnidharka VR. Acute renal failure in children requiring dialysis therapy. Indian Pediatr 1994;31(3):305-9.
12. Bourquia A, Zaid D. Acute renal insufficiency in children: Retrospective study of 89 cases. Ann Pediatr 1993;40(10):603-8.
13. Haycock GB. Management of acute and chronic renal failure in the newborn. Semin Neonatol 2003;8(4):325-34.
14. Pejovic B, Peco-Antic A, Dunjic R. Acute oliguric renal failure in hypoxic neonates born at full term. Srp Arh Celok Lek 2002;130(11-12):367-70.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk