|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
CASE REPORT |
||||
|
- |
||||
|
Volume 25 |
October - December 2009 (Part-II) |
Number 6 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
CASE REPORT |
||||
|
- |
||||
|
Volume 25 |
October - December 2009 (Part-II) |
Number 6 |
||
|
|
||||
|
|
||||
Castleman’s disease in association with follicular
dendritic cell sarcoma presenting as a neck mass
S. Hassan1, Y. Suhaimi2, A. Baharudin3
ABSTRACT
Castleman’s disease is a condition which usually occurs in the mediasternum. Very few cases have been reported to present as a neck swelling. Castleman’s disease is rarely associated with follicular dendritic sarcoma. We report a case of 65 years old male with painless and slowly progressive right neck swelling who was initially suspected to be schwannoma but proved to be a Castleman’s disease with associated follicular dendritic sarcoma.
KEY WORDS:
Castleman’s disease, Follicular dendritic sarcoma, Neck swelling.Pak J Med Sci October - December 2009 (Part-II) Vol. 25 No. 6 1021-1024
How to cite this article:
Hassan S, Suhaimi Y, Baharudin A. Ischemia modified albumin a potent marker in acute myo ardial infarction in normolipidaemic. Pak J Med Sci 2009;25(6):1021-1024.
1. S. Hassan (DLO MCPS)
2. Suhaimi MMED ORL-HNS (USM),
3. Baharudin A MMED ORL-HNS (USM)
1-3: Dept. ORL-HNS,
School of Medical Sciences,
Univ. Sains Malaysia, Kubang Kerian 16150,
Kelantan, Malaysia.
Correspondence
Dr Baharudin Abdullah MBBS(Mal), MMED ORL-HNS (USM)
Department of Otolaryngology,
Head and Neck Surgery(ORL-HNS),
School of Medical Sciences, Universiti Sains Malaysia,
Kubang Kerian 16150, Kelantan, Malaysia.
Email: baharudin@kb.usm.my
* Received for Publication: July 7, 2009
* Accepted: October 31st 2009
INTRODUCTION
Castleman’s disease (CD) is a rare heterogeneous group of lymphoproliferative disorder with a typical presentation of a lymphadenopathy in the mediasternum. Only six percent of cases have been reported to present in the neck.
1 The etiology and pathogenesis of this entity is still unclear. It is histologically and prognostically distinct from malignant lymph-node hyperplasia. It was first described in 1956 by Castleman et al2 in a group of patients with benign localised hyperplastic lymph-nodes. Histologically, it is characterized by angiofollicular lymph-node hypertrophy.CD can be either localized (hyaline-vascular and plasma type), multicentric or mixed. Localised CD by definition is localized to one site. Fifty one percent of patients are asymptomatic especially in hyaline-vascular type.
3 Usually they are discovered incidentally during routine physical examination, chest X- ray or abdominal ultrasound. It features lymphoid hyperplasia associated with excessive angiogenesis.About seventy percent of affected patients are less than 30 years old and males are affected more than females (4:1). Presentation can be asthenia (20%), fever (20%), weight loss (10%), abdominal or thoracic pain which mostly associated with plasma type.
CASE REPORT
A 65 years old man presented with a painless right sided neck swelling which progressively increased in size for three years. He experienced neck discomfort and mild difficulty in swallowing especially to solid food. He didn’t have any difficulty of breathing or any constitutional symptoms. He also denied any history of exposure to any patient with tuberculosis.
On examination, there was a large right sided neck swelling measuring five centimeters by ten centimeters which extended from upper third of the neck down to the clavicle. The swelling had a smooth surface, well defined border, hard in consistency and not tender. The anterior part of the mass extended down to the upper mediasternum. No other cervical lymph nodes were palpable. Examination of both vocal cords showed normal movement. Other examinations revealed no significant finding.
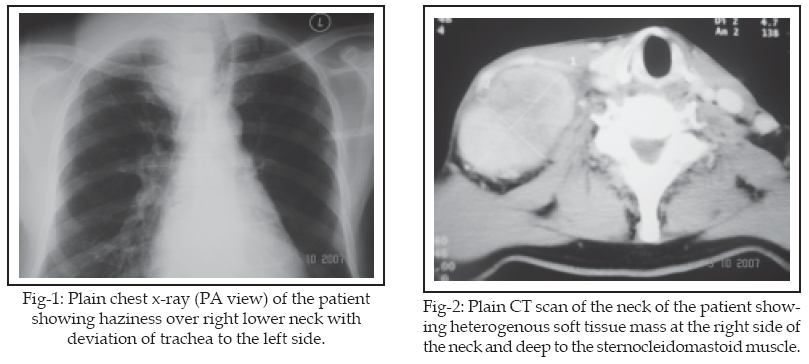
Fine needle aspiration and cytology showed mesenchymal lesion with atypia. CT scan from base of skull to thoracic inlet showed fairly well defined heterogeneously enhancing soft tissue density lesion with area of necrosis at the right side of the neck and deep to the sternocleidomastoid muscle. The carotid and internal jugular vein on the right side are splayed.
The right internal jugular vein was displaced laterally to the right side. Adjacent brachiocephalic vein was stretched. The mass extended to the anterior mediasternum on the right side. The right carotid was displaced anteromedially. Multiple small soft tissue density lesions suggestive of lymph nodes were seen in the right cervical region and lymphadenopathy was also noted adjacent to the lesion.
Based on the location of the lesion, the features are suggestive of mass from neural origin such as schwannoma or neurofibroma. Patient had undergone excision of the right neck mass with selective posterolateral neck dissection. During procedure, the mass was noted to be situated in between internal jugular vein and common carotid artery. Part of the mass at the upper anterior mediasternum was excised without opening of the sternum. Grossly, the mass was irregular in shape attached by fibrocollagenous band. It was encapsulated with greyish brown in colour. The cut section of the mass showed greyish white lobulated areas with foci of calcification, necrosis and cystic area. It also consists of fibro fatty tissue with attached lymph nodes.
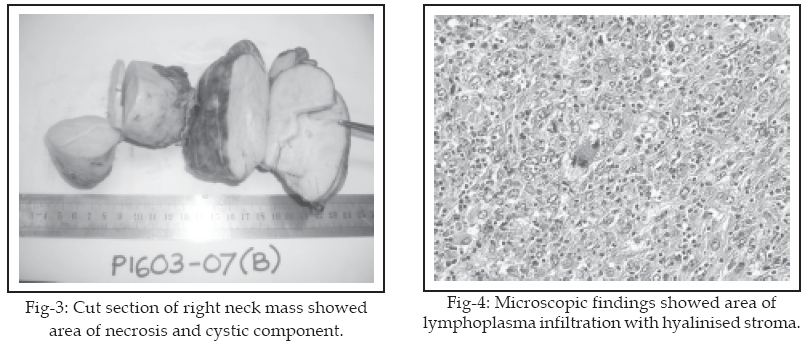
There was also prominent lymphoplasma cells infiltrate and clusters of foamy macrophages with scattered eosinophils were present in the stroma through out the tumour. Mitotic figures are scanty in these cellular areas with hyalinised stroma. Other areas display highly cellular foci with sheet of cells separated by fibrovascular septi. Lymphoid follicles of varying sizes with germinal centre also scattered in the background. Several follicles appear burnt out with hyalinised venules at the centre. Tumour necrosis was seen focally but was not prominent. Immunohistochemical stained was positive for Vimentin, CD 68 and Ki-67.
DISCUSSION
Multicentric or generalized CD is characterized by manifestation of multisystem involvement with predominant lymphadenopathy presentation especially involving peripheral lymph nodes. Individuals with this type of CD often exhibit symptoms similar to those associated with the plasma cell type. In addition, some individuals may have an enlarged liver and spleen (hepatosplenomegaly). Patients with multicentric disease tend to be older individuals in their fifth or sixth decade. Patient may present with asthenia (65%), weight loss (67%) and fever (69%) which is as consequence of elevated Interleukin-6 (IL-6). 24% of cases have been associated with POEMS (Peripheral polyneuropathy, Organomegaly, Endocrinopathy, Monoclonal gammopathy (M-Protein) and Skin signs) Syndrome. Non-Hodgkins lymphoma and Kaposi’s sarcoma was also documented to occur with increased frequency in patients with the multicentric variant.
4Follicular dendritic sarcoma (FDS) was described to be associated with CD (hyaline – vascular type) in 10% to 20% of cases.
5 However, these localizations of FDS associated with CD were different from the usual site distribution of this disease. Only one report has demonstrated the evolution of CD toward follicular dendritic sarcoma.6 In one study, they postulated that the CD is a reactive stage of the FDS tumor rather than a precursor lesion. However in some cases FDS appeared many years after the diagnosis of CD at the same anatomic location. The probable progression of FDS proliferation in the setting of CD is, at first limited to the follicles followed by overgrowth in the interfollicular and finally in the form of a Follicular Dendritic Sarcoma .67According to the World Health Organization classification of tumors of hematopoietic and lymphoid tissues, FDS belongs to histiocytic and dendritic cell neoplasms.
8 The tumors located in cervical lymph nodes and tonsils are relatively well-circumscribed nodular or bosselated masses.Histologically, it is composed of spindle or oval cells, arranged in sheets and focally showing a storiform or whorled growth pattern. Epithelioid cells and multinucleated giant cells may be seen. The immunophenotype of FDCS is positive for CD21, CD35, Ki-M4p, and Ki-FDC1p; and variably positive for vimentin, S-100 protein, CD68, and specific muscle actin.
8,9The differential diagnosis for FDS including squamous cell carcinoma, undifferentiated carcinoma, large cell lymphoma, meningioma, malignant melanoma, thymoma, malignant fibrous histiocytoma, peripheral nerve sheath tumor, angiosarcoma, and inflammatory pseudotumor.
10 These diagnoses can be ruled out by immunohistochemical studies because the tumor cells do not express specific FDC markers. 11 However, there may be diagnostic difficulties with these rare tumors especially at extra nodal site where they can be misdiagnosed since FDC markers are not routinely used in the immunohistochemical study of poorly differentiated tumors.8,10Surgery is the mainstay of treatment for follicular dendritic sarcoma. In this case, total excision of tumour and selective posterolateral neck dissection was performed despite no confirmation of preoperative tissue diagnosis. There is a role of radiotherapy and chemotherapy especially when the tumour is aggressive, high volume and surgically inaccessible.
12CONCLUSION
Since Castleman disease with follicular dendritic sarcoma is very rare, it is important to get a definite tissue diagnosis prior to definite management especially if the patient presents with neck swelling and systemic symptoms.
REFERENCES
1. Kooper DP, Tiwari RM, van der Valk P. Castleman’s disease as an uncommon cause of a neck mass. Eur Arch Otorhinolaryngol 1994 ;251:370–372.
2. Castleman B, Iverson L, Menendez VP. Localized mediastinal lymph-node hyperplasia resembling thymoma. Cancer 1956; 4:822-830.
3. Herrada J, Cabanillas F, Rice L, Manning J, Pugh W. The clinical behavior of localized and multicentric Castleman disease. Ann Intern Med. 1998;128(8):657-62.
4. Oksenhendler E, Duarte M, Soulier J, Cacoub P, Welker Y, Cadranel J, et al.. Multicentric Castleman’s disease in HIV infection: a clinical and pathological study of 20 patients. AIDS 1996;10(1):61-7.
5. B. Perez-Ordon, Rosai J. Follicular dendritic cell tumor: review of the entity, Semin Diagn Pathol 1998;15:144–154.
6. Chan AC, Chan KW, Chan JK. Development of follicular dendritic cell sarcoma in hyaline-vascular Castleman’s disease of the nasopharynx: tracing its evolution by sequential biopsies, Histopathology 2001;38:510–518.
7. Loo CK, Henderson C, Rogan K. Intrabdominal follicular dendritic cell sarcoma: report of a case with fine needle aspiration finding. Acta Cytol 2001;45:999-1004.
8. Satoh K, Hibi G, Yamamoto Y. Follicular dendritic cell tumor in the oro-pharyngeal region: report of a case and a review of the literature, Oral Oncol 2003;39:415–419.
9. Chan JK, Fletche CD, Nayler S. Follicular dendritic cell sarcoma. Clinicopathologic analysis of 17 cases suggesting malignant potential higher than currently recognized, Cancer 1997; 79 :294–313.
10. Idrees MT, Brandwein-Gensler M, Strauchen JA. Extranodal follicular dendritic cell tumor of the tonsil. Report of a diagnostic pitfall and literature review, Arch Otolaryngol Head Neck Surg 2004;130:1109–1113.
11. Tisch M, Hengstermann F, Kraft K, von Hinüber G, Maier H. Follicular dendritic cell sarcoma of the tonsil: Report of a rare case. Ear Nose Throat J. 2003;82(7):507-9.
12. Moz U, Pignatelli U, Forner Candiago PE, D’Addazio G, Casirati C, Gamba P. Follicular dendritic cell tumour of the cervical lymph node: case report and brief review of literature: Acta Otorhinolaryngol Ital 2004;24:223-225.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk