|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
April - June 2009 (Part-II) |
Number 3 |
||
|
|
||||
|
|
||||
|
|
||||
|
Published by : PROFESSIONAL MEDICAL PUBLICATIONS |
||||
|
ISSN 1681-715X |
||||
|
||||
|
- |
||||
|
ORIGINAL ARTICLE |
||||
|
- |
||||
|
Volume 25 |
April - June 2009 (Part-II) |
Number 3 |
||
|
|
||||
|
|
||||
Treatment of iatrogenic bilateral adductor vocal cord
immobility by endoscopic posterior transverse
cordotomy with cutting diathermy
Muhammad Azeem Aslam
ABSTRACT
Objectives: To access the efficacy, safety and complication rate of posterior transverse cordotomy with electrocautry in the treatment of iatrogenic bilateral vocal cord immobility.
Methodology: This prospective quasi-experimental study included 12 female patients with iatrogenic bilateral vocal cord immobility after thyroid surgery, which came to outpatient clinic of department of otolaryngology of a tertiary care teaching hospital in Rawalpindi, between January 2004 to December 2007. In all patients, endoscopic posterior transverse cordotomy was done with electrocautry under general anesthesia. These patients were followed up for six months and accessed for decannulation rate, postoperative voice and complications.
Results: Nine out of 12 patients (75%) had successful decannulation on 3rd postoperative day. Only two (16.6%) required revision surgery on opposite vocal cord and were decannulated making overall decannulation rate of 91.6%. Postoperative voice analysis showed that eight patients (66.6%) had ‘better’ voice, three (25%) had ‘same’ whereas only one patient (8.3%) had ‘worse’ voice. Postoperatively, six patients (50%) had no dyspnoea, five (41.6%) had mild and one (8.3%) patient had severe dyspnoea. None of the patients had aspiration or swallowing difficulty. The whole procedure took 8 to 19 minutes with mean duration of 10.6 minutes.
Conclusions: Treatment of iatrogenic bilateral vocal cord immobility with electrocautry can produce adequate postoperative airway and voice. This procedure is safe and not associated with any significant complications.
KEY WORDS: Vocal cords, Vocal cords paralysis, Laser surgery, Complication.
Pak J Med Sci April - June 2009 (Part-II) Vol. 25 No. 3 391-397
How to cite this article:
Aslam MA. Treatment of iatrogenic bilateral adductor vocal cord immobility by endoscopic posterior transverse cordotomy with cutting diathermy. Pak J Med Sci 2009;25(3): 391-397.
Dr. Muhammad Azeem Aslam FCPS
Associate Professor ENT
Department of Otolaryngology and
Head & Neck Surgery
Islamic International Medical College,
Rawalpindi - Pakistan.
Correspondence
Dr. Muhammad Azeem Aslam
House No. 57,
Main Road, Sector G-8/2,
Islamabad – Pakistan.
E-mail: drazeemaslam@gmail.com
* Received for Publication: December 30, 2008
* Accepted: May 5, 2009
INTRODUCTION
Iatrogenic bilateral vocal cord immobility is rare but a challenging problem for the laryngologist. Most commonly it arises as a result of damage to bilateral recurrent laryngeal nerves during thyroid surgery.
1,2 As both the vocal cords are in paramedian position, patient usually has satisfactory voice but airway is compromised. It can result in immediate postoperative stridor which is a life threatening condition and require immediate management by performing tracheotomy. Sometime it can present days to months or even years after the thyroid surgery.3 Wide variety of surgical techniques are being used to treat iatrogenic bilateral vocal cord immobility with varying degree of success. These include both external laryngeal surgical procedures and those done endoscopically. All these procedure can be broadly categorized as dynamic or static ones.4 The results of dynamic procedures are controversial so laryngologist are increasingly focusing on static ones. With the addition of laser in the armamentarium of laryngologist, a significant change is observed in favor of endoscopic static procedures for the treatment of bilateral vocal fold immobility.5 Whichever surgical procedure is adopted for the treatment of bilateral vocal fold immobility, the ultimate aim is to provide an adequate airway with preservation of voice and laryngeal competence.Static endoscopic procedures done with the help of laser, usually involves posterior transverse cordectomy with or without arytenoidectomy. The rationale behind these procedures are that anterior glottis is required for phonation and posterior glottis for respiration. As the aim of treatment is to restore an adequate airway without significantly affecting voice quality, so only posterior glottis should be widened without disturbing the anterior glottis.
6Laser cordectomy with or without arytenoidectomy is most popular now a days but laser equipment is not only costly but also the facility is available in few selected centers in Pakistan.
5 In the present study we performed posterior transverse cordotomy by electrocautry and evaluated its results. No special or costly equipment is required for this technique. Electrocautry machine is available in almost all operation theatres. This equipment is considerably cheap as compared to laser and does not require any special operative precautions. Therefore, treatment by electrocautry will not be a financial burden on the patient as compared to laser treatment. This will benefit not only the poor patients but will not be a burden on our already taxed health system. Considering the above mentioned factors, we studied the efficacy of treatment of bilateral vocal cords immobility by using electrocautry as an alternative to laser, for performing posterior transverse cordotomy.METHODOLOGY
This prospective quasi-experimental study included 12 female patients who were diagnosed with bilateral vocal folds immobility after surgery for benign thyroid disease. These patients came to outpatient clinic of the department of otolaryngology and head & neck surgery of a tertiary care teaching hospital in Rawalpindi, between January 2004 to December 2007. The age of these patients ranged between 30 to 58 years with mean age of 42.8 years. All these patients were subjected to detailed history, routine systemic, neurological and otolaryngological examinations including direct examination of larynx by fiberoptic nasopharyngoscopy under local anesthesia and findings were recorded on a predesigned Performa. Patients with failed prior treatment, recent onset of paralysis (<6 months) and those who had less than six months of follow up were excluded from the study. Data collection included symptoms of hoarseness, stridor, dyspnoea, aspiration and swallowing problems. Time interval between thyroid surgery and onset of symptoms, severity and duration of these symptoms were also recoded. Voice recordings were made immediately before and six months after surgery and analyzed not only by an experienced speech therapist but also subjectively by the patient herself. Voice was graded into ‘better’, ‘same’ or ‘worse’ than the voice before surgery. Postoperatively, aspiration and swallowing was evaluated according to the Pearson scale
7 mentioned in Table-I.

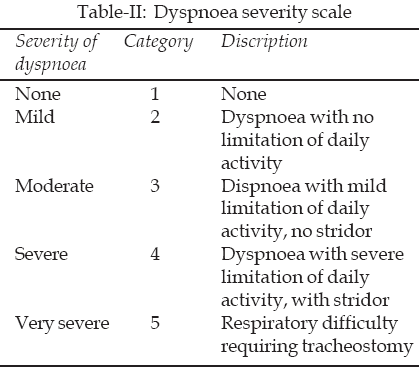
Severity of dyspnoea in the pre-operative and post-operative period was categorized into none, mild, moderate, severe and very severe according to the criteria8 mentioned in Table-II.
Surgical Technique:
In all patients surgery was performed under general anesthesia. Those patients who had tracheotomy in situ at the time of presentation were given anesthetic gases through tracheotomy tube while those without tracheotomy were intubated per orally utilizing small sized endotrachial tube. An appropriate sized laryngoscope was used and suspended to expose the larynx. Larynx was sprayed with 4% xylocaine solution. Ziess OPMI microscope with 400 mm lens was used to visualize the vocal cords. The junction of vocal process of arytenoids with membranous part of vocal cord was identified by palpation with micro-bore metallic laryngeal suction catheter. The passive electrode of the electrocautry machine was applied to the left calf and a 30 cm long active electrode (Fig-1) was used to make a transverse incision at posterior part of membranous vocal cord just anterior to the vocal process of arytenoid, a site which was earlier identified by palpation.

Care was taken not to expose the cartilage. Active electrode is insulated throughout its length to avoid mucosal injury except at its distal cutting edge. For better control, foot switch of electrocautry is used by the surgeon to activate the cautry. Injury to the anterior two thirds of vocal cord and to any other part of laryngeal mucosa is avoided. Transverse incision with electrocautry was carried out through the entire vocalis and thyroarytenoid muscle. In this way a wedge shaped area was created due to recoil of the cut ends of membranous cord. (Fig-2 & 3)
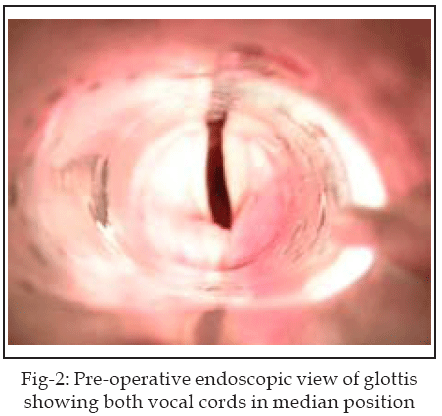
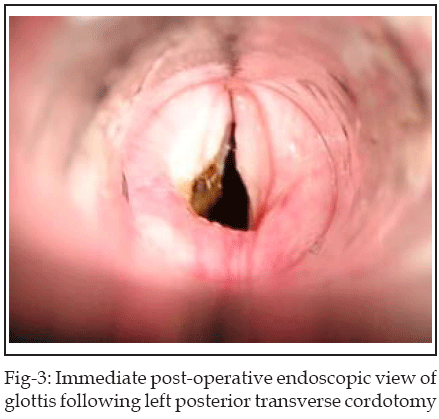
The decision to perform right or left cordotomy was left to the surgeon’s discretion. Only one side is operated at a time. If bleeding was encountered, it was controlled by applying pressure with cotton swab soaked in adrenaline (1:1000) to the cauterized area with laryngeal cup forceps for few minutes.
Patients without tracheotomy were given intraoperative dexamethosone 4mg i.v. to reduce laryngeal oedma. This was repeated twice in next 24 hours. All patients were given broad spectrum prophylactic oral antibiotics for five days after the operation.
Decannulation was attempted on third post operative day. Those patients who cannot tolerate decannulation on third post operative day was given five days course of oral steroids (prednisone 1mg/kg body weight) which was tapered over next five days. If decannulation was not achieved two weeks after the operation, cordectomy was repeated on the opposite vocal cord utilizing the same procedure mentioned earlier.
Initially patients were followed up at one weak interval for one months and then at monthly interval for next six months. On each follow up visit, fiberoptic direct laryngoscopy was done under local anesthesia to look for any complication e.g., odema, granulations, aspiration, web formation. Voice recording was done on each follow up visit.
RESULTS
A total of 12 female patients with post thyroidectomy bilateral adductor vocal cord paralysis were included in this study. Age range was between 30 to 58 years with the mean age of 42.8 years. Seven patients (58.3%) had tracheotomy in situ at the time of presentation. Prophylactic tracheotomy was done in four patients (33.3%) immediately before the surgical procedure. In one patient (8.3%), cordotomy was done without prophylactic tracheotomy. Time interval between thyroidectomy and appearance of stridor and dyspnoea varied widely, it ranged between 0 (i.e., immediate postoperatively) to 21 years after the operation. In five patients (41.6%), stridor started as soon as patient was extubated after thyroid surgery which resulted in tracheotomy in these patients.
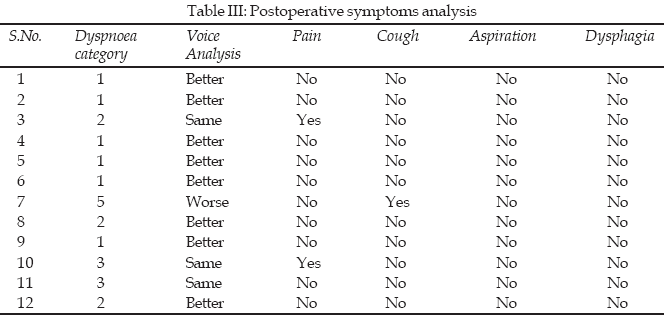
Fiberoptic laryngoscopic examination done at the time of presentation revealed bilateral vocal cords immobilized in paramedian position in all the patients. In all patients posterior transverse cordectomy was done with electrocautry under general anesthesia. Right sided cordotomy was done in six patients (50%) whereas in remaining six, cordotomy was done on left side. No serious per-operative or immediately postoperative complication was encountered except mild laryngospasm in one patient during recovery from anesthesia which settled with systemic steroid and oxygenation. Prophylactic tracheotomy was not done in this patient. In another patient, bleeding occurred immediately after cordotomy which was controlled by applying pressure with adrenaline soaked cotton swab with the help of laryngeal cup forceps for five minutes before recovery from anesthesia. The whole procedure took eight to 19 minutes with average duration of 10.6 minutes. Patient’s symptoms in postoperative period and during follow-up are summarized in Table III. Postoperatively, nine patients (75%) had dyspnoea category of one and two, two patients (16.6%) had category three dyspnoea and only one (8.3%) had category five dyspnoea. Two patients (16.6%) complained of pain at the operated site which was cured within four days by prescribing diclofenac sodium 50 mg tablet twice daily. Postoperative cough was observed in one patient (8.3%) which resolved in five days with anti-tussive medication (dextrom-ethorpahn syrup). None of the patient had aspiration or swallowing difficulty in the post operative period and during follow-up.
Postoperative voice analysis by patients herself and speech therapist was done at each follow up visit and at the end of 6 months of follow-up. Eight (66.6%) had ‘better’ voice, 3 (25%) stated that their voice is ‘same’ whereas one patient (8.3%) reported her voice became ‘worse’ after surgery.
Decannulation was attempted on 3
rd postoperative day. Nine out of 12 patients (75%) had successful decannulation with no stridor or dyspnoea at rest. Two patients (16.6%) among them complained of mild dyspnoea on moderate exertion. Three patients who did not tolerate decannulation were given oral steroids (prednisolone 1 mg/kg body weight/day) for five days and then tapered in next five days. Decannulation was again tried after that period but was not successful. In two out of three patients who failed decannulation, same surgical procedure was repeated on previously non-operated vocal cord on 20 and 41 days after the first procedure. Both were decannulated on 3rd and 5th postoperative day respectively without any complications. Third patient refused surgery at that time. She came after 22 months and requested decannulation. Surgical procedure was repeated on opposite vocal cord by using same technique. Decannulation was attempted on 3rd postoperative day but was not successful. Fiberoptic laryngoscopy revealed no granulations or obstructive pathology in supraglottic or subglottic area. Patient refused any further treatment however she came for regular follow-up for six months. No complication developed in that period.DISCUSSION
In the present study, we utilized cutting diathermy instead of laser for performing posterior transverse cordotomy for the treatment of bilateral iatrogenic vocal cord immobility, to achieve an adequate airway while preserving voice and laryngeal competence. Basically, laser act as a hot knife which by concentrating intense energy at the site of procedure, ablate instead of cutting the tissues.
9Twelve patients with iatrogenic bilateral vocal cord immobility were included in the present study. It is generally believed that in majority of cases, symptoms of respiratory distress manifest immediately after thyroid surgery in case of bilateral recurrent laryngeal nerve damage causing bilateral vocal cord immobility. The time interval between thyroid surgery and appearance of symptoms varied widely in the present study, ranging between immediately after surgery in four patients to up to 21 years after surgery in remaining patients. In another study, symptom free interval after thyroid surgery varied from six months to eight years.
10 Symptoms free interval of many years after thyroid surgery is difficult to explain.Seven patients in this study were tracheostomised whereas in four patients, tracheotomy was done preoperatively. In one patient, cordotomy was done without prophylactic tracheotomy, but that patient developed laryngospasm in the immediate postoperative period which was managed successfully by giving systemic steroids and with improved oxygenation. This showed that prophylactic tracheotomy is safe before endoscopic cordotomy but several other studies in which laser cordoctomy was done, showed a difference of opinion as far as prophylactic preoperative tracheotomy is concerned.
2,4,8,11In our study, nine out of twelve patients (75%) were decannulated successfully on 3
rd postoperative day without any dyspnoea or stridor at rest after decannulation. Three patients did not tolerate decannulation even after receiving ten day course of oral steroids. Revision procedure was done in two of those followed by successful decannulation. Thus, overall successful decannulation was achieved in eleven out of twelve patients making our decannulation rate 91.66%. In a study utilizing laser cordotomy in 18 patients achieved decannulation rate of 88.8%.2 In literature, decannulation rates ranging between 80 to 100% have been achieved using laser equipment. Our decannulation rate correlates well with these studies.2,12,13Revision procedure, in our study, was required in only two patient (16.6%) which is quiet low if we compare it with other studies in which cordotomy was done with laser. Revision rate reported in literature is between 19 to 66%.
8 In a study in which CO2 and KTP-532 lasers were used for cordectomy,2 revision surgery was required in 50% of cases. In another study, in which radiofrequency was used for cordotomy instead of laser, revision surgery was not required in any case.4 Revision procedure is required mostly as a result of granuloma formation at the site of surgery.2,4 Dursun G and Gokcan MK suggested that laser should be used at low power in pulsed mode to decrease thermal injury which will result in decrease risk of granuloma formation.8 We did not found this complication in any of our patient. Probable reason may be that electrocautry produces less thermal energy as compared to laser. Another reason for granuloma formation is exposed cartilage.2 We did not perform arytenoidectomy in any patient included in this study, which may result in exposing bare cartilage leading to granuloma formation.Nine patients in the present study experienced either no or mild dyspnoea without limitation of daily activities. In one patient, dyspnoea resulted in mild limitation of daily activity. Only one patient had severe dyspnoea on decannulation. Although revision surgery on opposite vocal cord was done but decannulation was still not possible and patient refused further treatment.
None of our patients experienced aspiration or swallowing problems. Probable reason was that we preserved arytenoids and surgical procedure was limited to cordectomy. Similar finding was also observed in another study in which laser cordectomy was done without arytenoidectomy. Whereas in one study involving 22 patients, in which cordectomy with partial arytenoidectomy was done, six patients (27.2%) experienced postoperative aspiration
11. This suggests that arytenoids preservation prevents postoperative aspiration problems.Only two patients complained of pain at the operated site which was cured within 4 days by prescribing diclofenac sodium 50 mg tablet twice daily. Postoperatively, pain at operative site is more common with laser procedures as compared to conventional surgery. Cutting diathermy produces much lower temperatures necessary to ablate the tissues as compared to laser. The higher temperatures produced by the laser results in significant heat propagation damaging adjacent tissues which results in pain at the operated site.
14Average duration of procedure in this study was only 10.6 minutes. In laser surgery, more time is required to prepare the laser apparatus and observe necessary precautions. Voice quality of patients in postoperative period was accessed by patients themselves as well as by a speech therapist. Pre and post operative voice recordings were compared. It is generally believed that increase in airway results in deterioration of voice quality. This view is not supported by the present study. Majority (66.6%) of patients in this study rated their voice as ‘better’ where as 25% said that there is no change in their voice. In only one case, voice became ‘worse’ after surgery. We believe that by performing posterior transverse cordotomy, anterior vocal cords are preserved resulting in airway enlargement with good voice preservation. This opinion is shared by many other studies.
2,15,16CONCLUSIONS
This study illustrates that the treatment of iatrogenic bilateral vocal cords immobiltiy with electrocautry can produce good outcome in terms of adequate post operative airway and voice. This procedure is technically easy to perform, requires very short time and is not associated with any significant complication. Therefore it can be considered as an alternative to laser in the treatment of iatrogenic bilateral vocal cords immobility at places where facility of laser treatment is not available.
REFERENCES
1. Benninger MS, Gillen JB, Altman JS. Changing etiology of vocal fold immobility. Laryngoscope 1998;108:1346-50.
2. Manolopoulos L, Stavroulaki P, Yiotakis J, Segas J, Adamopoulos G. CO2 and KTP-532 laser cordectomy for bilateral vocal fold paralysis. J Laryngol Otol 1999;113:637-41.
3. Watkinson JC, Gaze MN, Wilson JA. Stell and Maran’s Head and Neck Surgery. 4th Ed. India. Butterworth-Heinemann Publishers; 2000:362.
4. Elsherief S, Elsheikh MN. Endoscopic radiosurgical posterior transverse cordotomy for bilateral median vocal fold immobility. J Laryngol Otol 2004;118:202-206.
5. Waleem SSU, Rashid D. CO2 laser treatment of benign laryngeal diseases. Pak J Otolaryngol 2002;20:44-7.
6. Crumley RL. Endoscopic laser medial arytenoidectomy for airway management in bilateral laryngeal paralysis. Ann Otol Rhinol Laryngol 1993;102:81-4.
7. Pearson BW. Subtotal laryngectomy. Laryngoscope 1981;81:1904-12.
8. Dursun G, Gokcan MK. Aerodynamic, acoustic and functional results of posterior transverse laser cordotomy for bilateral abductor vocal fold paralysis. J Laryngol Otol 2006;120:282-88.
9. Hussain SS. Comparative study of laser and conventional surgery in laryngeal diseases. Pak Armed Forces Med J 2004;54:54-58.
10. Parsad U. CO2 surgical laser in the management of bilateral vocal cord paralysis. J Laryngol Otol 1985;99:891-94.
11. Shvero J, Koren R, Stern Y, Segal K, Feinmesser R, Hadar T. Laser posterior ventriculocordectomy with partial arytenoidectomy for the treatment of bilateral vocal fold immobility. J Laryngol Otol 2003;117:540-43.
12. Rontal M, Rontal E. Endoscopic laryngeal surgery for bilateral midline vocal fold obstruction. Annals Otology, Rhinology Laryngol 1990;99:605-10.
13. Worley G, Bajaj Y, Cavalli L, Hartley B. Laser arytenoidectomy in children with bilateral vocal fold immobility. J Laryngol Otol 2007;121:25-7.
14. Troell RJ, Powell NB, Riley RW, Kasey K, Guilleminault C. Comparison of postoperative pain between laser assisted uvulopalatoplasty, uvulopalatopharyngoplasty and radiofrequency volumetric tissue reduction of the palate. Otolaryngol Head Neck Surg 2000;122:402-9.
15. Friedman EM, deJong AL, Sulek M. Pediatric bilateral vocal fold immobility: the role of carbon dioxide laser posterior transverse partial cordectomy. Ann Otol Rhinol Laryngol 2001;110:723-8.
16. Segas J, Stavroulakis P, Manolopoulos L, Yiotakis J, Adamopoulos G. Management of bilateral vocal fold paralysis: Experience at University of Athens. Otolaryngol Head Neck Surg 2001;124:68-71.
HOME | SEARCH | CURRENT ISSUE | PAST ISSUES
Professional
Medical Publications
Room No. 522, 5th Floor, Panorama Centre
Building No. 2, P.O. Box 8766, Saddar, Karachi - Pakistan.
Phones : 5688791, 5689285 Fax : 5689860
pjms@pjms.com.pk